The Impact of a Comprehensive Risk Prediction Model for Colorectal Cancer on a Population Screening Program
- PMID: 33134836
- PMCID: PMC7583148
- DOI: 10.1093/jncics/pkaa062
The Impact of a Comprehensive Risk Prediction Model for Colorectal Cancer on a Population Screening Program
Abstract
Background: In many countries, population colorectal cancer (CRC) screening is based on age and family history, though more precise risk prediction could better target screening. We examined the impact of a CRC risk prediction model (incorporating age, sex, lifestyle, genomic, and family history factors) to target screening under several feasible screening scenarios.
Methods: We estimated the model's predicted CRC risk distribution in the Australian population. Predicted CRC risks were categorized into screening recommendations under 3 proposed scenarios to compare with current recommendations: 1) highly tailored, 2) 3 risk categories, and 3) 4 sex-specific risk categories. Under each scenario, for 35- to 74-year-olds, we calculated the number of CRC screens by immunochemical fecal occult blood testing (iFOBT) and colonoscopy and the proportion of predicted CRCs over 10 years in each screening group.
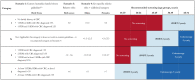
Results: Currently, 1.1% of 35- to 74-year-olds are recommended screening colonoscopy and 56.2% iFOBT, and 5.7% and 83.2% of CRCs over 10 years were predicted to occur in these groups, respectively. For the scenarios, 1) colonoscopy was recommended to 8.1% and iFOBT to 37.5%, with 36.1% and 50.1% of CRCs in each group; 2) colonoscopy was recommended to 2.4% and iFOBT to 56.0%, with 13.2% and 76.9% of cancers in each group; and 3) colonoscopy was recommended to 5.0% and iFOBT to 54.2%, with 24.5% and 66.5% of cancers in each group.
Conclusions: A highly tailored CRC screening scenario results in many fewer screens but more cancers in those unscreened. Category-based scenarios may provide a good balance between number of screens and cancers detected and are simpler to implement.
© The Author(s) 2020. Published by Oxford University Press.
Figures

Similar articles
-
Fecal occult blood test for colorectal cancer screening: an evidence-based analysis.Ont Health Technol Assess Ser. 2009;9(10):1-40. Epub 2009 Sep 1. Ont Health Technol Assess Ser. 2009. PMID: 23074514 Free PMC article.
-
Interval Colorectal Cancer Incidence Among Subjects Undergoing Multiple Rounds of Fecal Immunochemical Testing.Gastroenterology. 2017 Aug;153(2):439-447.e2. doi: 10.1053/j.gastro.2017.05.004. Epub 2017 May 5. Gastroenterology. 2017. PMID: 28483499
-
Revised Australian national guidelines for colorectal cancer screening: family history.Med J Aust. 2018 Nov 19;209(10):455-460. doi: 10.5694/mja18.00142. Epub 2018 Oct 29. Med J Aust. 2018. PMID: 30359558
-
Improving Australian National Bowel Cancer Screening Program outcomes through increased participation and cost-effective investment.PLoS One. 2020 Feb 3;15(2):e0227899. doi: 10.1371/journal.pone.0227899. eCollection 2020. PLoS One. 2020. PMID: 32012174 Free PMC article.
-
Colon cancer screening: which non-invasive filter tests?Dig Dis. 2011;29 Suppl 1:56-9. doi: 10.1159/000331127. Epub 2011 Nov 15. Dig Dis. 2011. PMID: 22104755 Review.
Cited by
-
The SCRIPT trial: study protocol for a randomised controlled trial of a polygenic risk score to tailor colorectal cancer screening in primary care.Trials. 2022 Sep 27;23(1):810. doi: 10.1186/s13063-022-06734-7. Trials. 2022. PMID: 36163034 Free PMC article.
-
The use of individual and multilevel data in the development of a risk prediction model to predict patients' likelihood of completing colorectal cancer screening.Prev Med Rep. 2023 Aug 11;36:102366. doi: 10.1016/j.pmedr.2023.102366. eCollection 2023 Dec. Prev Med Rep. 2023. PMID: 37732019 Free PMC article.
-
Polygenic scores in cancer.Nat Rev Cancer. 2023 Sep;23(9):619-630. doi: 10.1038/s41568-023-00599-x. Epub 2023 Jul 21. Nat Rev Cancer. 2023. PMID: 37479830 Review.
-
A scoping review of risk-stratified bowel screening: current evidence, future directions.Cancer Causes Control. 2022 May;33(5):653-685. doi: 10.1007/s10552-022-01568-9. Epub 2022 Mar 20. Cancer Causes Control. 2022. PMID: 35306592 Free PMC article.
-
A qualitative study of a new metric for estimating early-onset colorectal cancer risk in male veterans: "Colon Age".BMC Prim Care. 2025 Jul 15;26(1):226. doi: 10.1186/s12875-025-02854-6. BMC Prim Care. 2025. PMID: 40665259 Free PMC article.
References
-
- Malila N, Senore C, Armaroli P. European guidelines for quality assurance in colorectal cancer screening and diagnosis—organisation. Endoscopy. 2012;44(S 03):SE31–SE48. - PubMed
-
- Cancer Council Australia Colorectal Cancer Guidelines Working Party. Clinical Practice Guidelines for the Prevention, Early Detection and Management of Colorectal Cancer. Sydney, Australia: Colorectal Cancer in Australia; 2017.
-
- Jenkins MA, Ait Ouakrim D, Boussioutas A, et al.Revised Australian national guidelines for colorectal cancer screening: family history. Med J Aust. 2018;209(10):455–460. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
