Acute generalized exanthematous pustulosis and Stevens-Johnson syndrome overlap due to hydroxychloroquine: a case report
- PMID: 33138853
- PMCID: PMC7605900
- DOI: 10.1186/s13256-020-02504-8
Acute generalized exanthematous pustulosis and Stevens-Johnson syndrome overlap due to hydroxychloroquine: a case report
Abstract
Background: Since the World Health Organization declared a global pandemic due to the novel coronavirus disease2019, there have been targeted efforts to establish management modalities. Hydroxychloroquine has been suggested as a possible treatment; however, it is associated with multiple adverse reactions. We report a rare case of a patient with acute generalized exanthematous pustulosis with Stevens-Johnson syndrome due to hydroxychloroquine. Acute generalized exanthematous pustulosis is characterized by acute onset of a generalized rash that is pustular and erosive in nature, affecting limbs; trunk; face; and, less often, mucosal membranes. Although rare, it is important to be mindful of this side effect because the diagnosis is often delayed, and the disease has the potential to be life-threatening.
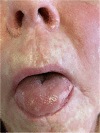
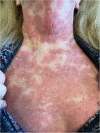
Case presentation: A 68-year-old American woman presented to our hospital with a painful, rapidly spreading rash. Its morphologic features included erythema multiforme-like lesions with extensive skin sloughing in various regions of the head, neck, and trunk and mucosal involvement. Her Nikolsky sign was negative, and she had no evidence of lesions on areas of skin trauma. Four weeks prior, she had been initiated on hydroxychloroquine for a presumed diagnosis of cutaneous sarcoidosis. Three punch biopsies of the head and neck area revealed subcorneal pustules consistent with acute generalized exanthematous pustulosis. Treatment began with high doses of methylprednisolone, leading to only minimal improvement of existing areas and ongoing spread to new areas. Treatment with intravenous immunoglobulin was initiated, at which point disease stability was achieved. The patient's rash ultimately resolved, as did her cutaneous pain and pruritus.
Conclusions: Among many potential adverse reactions involving hydroxychloroquine, cutaneous side effects are varied and can lead to significant morbidity or even death. The drug is currently being investigated in a multitude of trials for coronavirus disease2019 treatment, prevention, and prophylaxis after exposure to severe acute respiratory syndrome coronavirus 2. Acute generalized exanthematous pustulosis is a rare side effect of hydroxychloroquine, and even fewer cases demonstrate histologic evidence of acute generalized exanthematous pustulosis while clinically presenting with Stevens-Johnson syndrome. Patients who develop Stevens-Johnson syndrome/toxic epidermal necrolysis require best supportive care with aggressive fluid and electrolyte replacement and prevention of further breakdown of the skin barrier. With the potential of widespread hydroxychloroquine use, it is important that providers be aware of its potential severe adverse drug reactions.
Keywords: AGEP; COVID-19; Case report; Hydroxychloroquine.
Conflict of interest statement
The authors declare they have no competing interests.
Figures
Similar articles
-
Delayed Presentation of Acute Generalized Exanthematous Pustulosis Following Treatment with Cefepime in a Patient with COVID-19 without the Use of Hydroxychloroquine.Am J Case Rep. 2020 Oct 24;21:e926901. doi: 10.12659/AJCR.926901. Am J Case Rep. 2020. PMID: 33097683 Free PMC article.
-
Generalized pustular figurate erythema: A newly delineated severe cutaneous drug reaction linked with hydroxychloroquine.Dermatol Ther. 2020 May;33(3):e13380. doi: 10.1111/dth.13380. Epub 2020 Apr 16. Dermatol Ther. 2020. PMID: 32253799 Free PMC article. Review.
-
Clinical presentation and management of atypical and recalcitrant acute generalized exanthematous pustulosis.J Am Acad Dermatol. 2022 Sep;87(3):632-639. doi: 10.1016/j.jaad.2020.09.024. Epub 2020 Sep 11. J Am Acad Dermatol. 2022. PMID: 32926975 Review.
-
Severe cutaneous adverse reactions: acute generalized exanthematous pustulosis, toxic epidermal necrolysis and Stevens-Johnson syndrome.Med Clin North Am. 2010 Jul;94(4):727-42, x. doi: 10.1016/j.mcna.2010.04.004. Med Clin North Am. 2010. PMID: 20609860 Review.
-
Prolonged pustular eruption from hydroxychloroquine: an unusual case of acute generalized exanthematous pustulosis.Cutis. 2016 Mar;97(3):212-6. Cutis. 2016. PMID: 27023083
Cited by
-
Marginal corneal infiltrates as an ocular manifestation of acute generalized exanthematous pustulosis.Am J Ophthalmol Case Rep. 2023 Nov 9;32:101953. doi: 10.1016/j.ajoc.2023.101953. eCollection 2023 Dec. Am J Ophthalmol Case Rep. 2023. PMID: 38045987 Free PMC article.
-
Clinical features of acute generalized exanthematous pustulosis caused by hydroxychloroquine in rheumatology patients and exploration of CARD14 gene mutations.Front Med (Lausanne). 2023 Apr 6;10:1161837. doi: 10.3389/fmed.2023.1161837. eCollection 2023. Front Med (Lausanne). 2023. PMID: 37089611 Free PMC article.
-
Drug Triggers and Clinic of Acute Generalized Exanthematous Pustulosis (AGEP): A Literature Case Series of 297 Patients.J Clin Med. 2022 Jan 13;11(2):397. doi: 10.3390/jcm11020397. J Clin Med. 2022. PMID: 35054090 Free PMC article. Review.
-
Safety of Hydroxychloroquine: What a Dermatologist Should Know.Am J Clin Dermatol. 2025 Mar;26(2):251-264. doi: 10.1007/s40257-025-00919-x. Epub 2025 Feb 3. Am J Clin Dermatol. 2025. PMID: 39899183 Free PMC article. Review.
References
-
- Rainsford K, Parke AL, Clifford-Rashotte M, Kean W. Therapy and pharmacological properties of hydroxychloroquine and chloroquine in treatment of systemic lupus erythematosus, rheumatoid arthritis and related diseases. Inflammopharmacology. 2015;23:231–269. doi: 10.1007/s10787-015-0239-y. - DOI - PubMed
-
- Page RL, 2nd, O’Bryant CL, Cheng D, et al. Drugs that may cause or exacerbate heart failure: a scientific statement from the American Heart Association [published correction appears in Circulation. 2016;134(12):e261] Circulation. 2016;134(6):e32–e69. doi: 10.1161/CIR.0000000000000426. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical