Outcomes of patients with COVID-19 in the intensive care unit in Mexico: A multicenter observational study
- PMID: 33138974
- PMCID: PMC7577687
- DOI: 10.1016/j.hrtlng.2020.10.013
Outcomes of patients with COVID-19 in the intensive care unit in Mexico: A multicenter observational study
Abstract
Background: As of June 15, 2020, a cumulative total of 7,823,289 confirmed cases of COVID-19 have been reported across 216 countries and territories worldwide. However, there is little information on the clinical characteristics and outcomes of critically ill patients with severe COVID-19 who were admitted to intensive care units (ICUs) in Latin America. The present study evaluated the clinical characteristics and outcomes of critically ill patients with severe COVID-19 who were admitted to ICUs in Mexico.
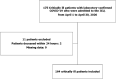
Methods: This was a multicenter observational study that included 164 critically ill patients with laboratory-confirmed COVID-19 who were admitted to 10 ICUs in Mexico, from April 1 to April 30, 2020. Demographic data, comorbid conditions, clinical presentation, treatment, and outcomes were collected and analyzed. The date of final follow-up was June 4, 2020.
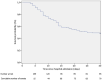
Results: A total of 164 patients with severe COVID-19 were included in this study. The mean age of patients was 57.3 years (SD 13.7), 114 (69.5%) were men, and 6.0% were healthcare workers. Comorbid conditions were common in patients with critical COVID-19: 38.4% of patients had hypertension and 32.3% had diabetes. Compared to survivors, nonsurvivors were older and more likely to have diabetes, hypertension or other conditions. Patients presented to the hospital a median of 7 days (IQR 4.5-9) after symptom onset. The most common presenting symptoms were shortness of breath, fever, dry cough, and myalgias. One hundred percent of patients received invasive mechanical ventilation for a median time of 11 days (IQR 6-14). A total of 139 of 164 patients (89.4%) received vasopressors, and 24 patients (14.6%) received renal replacement therapy during hospitalization. Eighty-five (51.8%) patients died at or before 30 days, with a median survival of 25 days. Age (OR, 1.05; 95% CI, 1.02-1.08; p<0.001) and C-reactive protein levels upon ICU admission (1.008; 95% CI, 1.003-1.012; p<0.001) were associated with a higher risk of in-hospital death. ICU length of stay was associated with reduced in-hospital mortality risk (OR, 0.89; 95% CI, 0.84-0.94; p<0.001).
Conclusions: This observational study of critically ill patients with laboratory-confirmed COVID-19 who were admitted to the ICU in Mexico demonstrated that age and C-reactive protein level upon ICU admission were associated with in-hospital mortality, and the overall hospital mortality rate was high.
Trial registration: ClinicalTrials.gov, NCT04336345.
Keywords: COVID-19; Coronavirus; Intensive care unit; Mexico; Outcomes; SARS-CoV-2 infection.
Copyright © 2020 Elsevier Inc. All rights reserved.
Conflict of interest statement
Declarations of Competing Interest The authors state that there are no conflicts of interest related to this study.
Figures
Comment in
-
ICU admission and outcome of patients with COVID-19: Does ICU stay improve survival?Heart Lung. 2021 May-Jun;50(3):470. doi: 10.1016/j.hrtlng.2021.01.017. Epub 2021 Jan 26. Heart Lung. 2021. PMID: 33526284 Free PMC article. No abstract available.
Similar articles
-
Characteristics and outcomes of patients with COVID-19 admitted to hospital and intensive care in the first phase of the pandemic in Canada: a national cohort study.CMAJ Open. 2021 Mar 8;9(1):E181-E188. doi: 10.9778/cmajo.20200250. Print 2021 Jan-Mar. CMAJ Open. 2021. PMID: 33688026 Free PMC article.
-
Risk Factors Associated With Mortality Among Patients With COVID-19 in Intensive Care Units in Lombardy, Italy.JAMA Intern Med. 2020 Oct 1;180(10):1345-1355. doi: 10.1001/jamainternmed.2020.3539. JAMA Intern Med. 2020. PMID: 32667669 Free PMC article.
-
Baseline Characteristics and Outcomes of 1591 Patients Infected With SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy.JAMA. 2020 Apr 28;323(16):1574-1581. doi: 10.1001/jama.2020.5394. JAMA. 2020. PMID: 32250385 Free PMC article.
-
Clinical course and outcomes of critically ill patients with COVID-19 infection: a systematic review.Clin Microbiol Infect. 2021 Jan;27(1):47-54. doi: 10.1016/j.cmi.2020.10.017. Epub 2020 Oct 23. Clin Microbiol Infect. 2021. PMID: 33190794 Free PMC article.
-
Global Impact of Coronavirus Disease 2019 Infection Requiring Admission to the ICU: A Systematic Review and Meta-analysis.Chest. 2021 Feb;159(2):524-536. doi: 10.1016/j.chest.2020.10.014. Epub 2020 Oct 15. Chest. 2021. PMID: 33069725 Free PMC article.
Cited by
-
The impact of different prophylactic anticoagulation doses on the outcomes of patients with COVID-19.Thromb Res. 2021 Jun;202:14-16. doi: 10.1016/j.thromres.2021.02.031. Epub 2021 Mar 6. Thromb Res. 2021. PMID: 33711753 Free PMC article.
-
Population-Based COVID-19 Screening in Mexico: Assessment of Symptoms and Their Weighting in Predicting SARS-CoV-2 Infection.Medicina (Kaunas). 2021 Apr 8;57(4):363. doi: 10.3390/medicina57040363. Medicina (Kaunas). 2021. PMID: 33917858 Free PMC article.
-
[Clinical characteristics related to mortality by COVID-19 in intensive care].Rev Med Inst Mex Seguro Soc. 2022 May 2;60(3):249-257. Rev Med Inst Mex Seguro Soc. 2022. PMID: 35759745 Free PMC article. Spanish.
-
Recent Advance Analysis of Recovery in Hospitalized People with COVID-19: A Systematic Review.Int J Environ Res Public Health. 2022 Nov 7;19(21):14609. doi: 10.3390/ijerph192114609. Int J Environ Res Public Health. 2022. PMID: 36361488 Free PMC article.
-
Sex differences in D-dimer and critical illness in patients with COVID-19: A systematic review and meta-analysis.Res Pract Thromb Haemost. 2023 Jan;7(1):100042. doi: 10.1016/j.rpth.2023.100042. Epub 2023 Jan 14. Res Pract Thromb Haemost. 2023. PMID: 36685003 Free PMC article.
References
-
- Coronavirus Disease (COVID-19): Situation Report-147. Geneva: World Health Organization (https://www.who.int/docs/default-source/coronaviruse/situation-reports/2... ).
-
- Conferencia 15 De Junio: Comunicado Técnico Diario. Mexico: Secretaría de Salud Federal (https://coronavirus.gob.mx/2020/06/15/conferencia-15-de-junio/).
-
- Knaus W.A., Draper E.A., Wagner D.P., Zimmerman J.E. APACHE II: a severity of disease classification system. Crit Care Med. 1985;13(10):818–829. - PubMed
-
- Vincent J.L., Moreno R., Takala J. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the working group on sepsis-related problems of the European society of intensive care medicine. Intensive Care Med. 1996;22(7):707–710. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous