Kaposi Sarcoma Rates Among Persons Living With Human Immunodeficiency Virus in the United States: 2008-2016
- PMID: 33140823
- PMCID: PMC8492218
- DOI: 10.1093/cid/ciaa999
Kaposi Sarcoma Rates Among Persons Living With Human Immunodeficiency Virus in the United States: 2008-2016
Abstract
Background: Recent studies have suggested that Kaposi sarcoma (KS) rates might be increasing in some racial/ethnic groups, age groups, and US regions. We estimated recent US trends in KS incidence among people living with human immunodeficiency virus (HIV; PLWH).
Methods: Incident KS patients aged 20-59 years were obtained from 36 cancer registries and assumed to be living with HIV. The number of PLWH was obtained from national HIV surveillance data from 2008 to 2016. Age-standardized KS rates and annual percent changes (APCs) in rates were estimated by age, sex, race/ethnicity, state, and region.
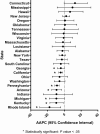
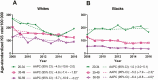
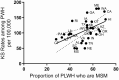
Results: Between 2008 and 2016, the age-adjusted KS rate among PLWH was 116/100 000. Rates were higher among males, in younger age groups, and among white PLWH. Washington, Maine, and California had the highest KS rates among PLWH. KS rates among PLWH decreased significantly (average APC = -3.2% per year, P < .001) from 136/100 000 to 97/100 000 between 2008 and 2016. There were no statistically significant increases in KS rates in any age, sex, or racial/ethnic group or in any geographic region or state. However, there were nondecreasing trends in some states and in younger age groups, primarily among black PLWH.
Conclusions: KS incidence rates among PLWH have decreased nationally between 2008 and 2016. Though there were no statistically significant increases in KS rates in any demographic or geographic group, nondecreasing/stagnant KS trends in some states and among younger and black PLWH highlight the need for early diagnosis and treatment of HIV infection.
Keywords: AIDS; HIV; Kaposi sarcoma; epidemiology; rates.
Published by Oxford University Press for the Infectious Diseases Society of America 2020.
Figures


References
-
- Martin JN, Ganem DE, Osmond DH, Page-Shafer KA, Macrae D, Kedes DH. Sexual transmission and the natural history of human herpesvirus 8 infection. N Engl J Med 1998; 338:948–54. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

