Antiplatelet Therapy Improves the Prognosis of Patients with Hepatocellular Carcinoma
- PMID: 33142758
- PMCID: PMC7693153
- DOI: 10.3390/cancers12113215
Antiplatelet Therapy Improves the Prognosis of Patients with Hepatocellular Carcinoma
Abstract
Aims: Antiplatelet therapy has been reported to reduce liver fibrosis and hepatocellular carcinoma (HCC), and has exhibited antitumor properties in other cancers. However, the effects of antiplatelet therapy after diagnosis of HCC are unknown. We investigated the effects of antiplatelet therapy on prognosis, tumor progression, liver function and safety in HCC patients.
Methods: We retrospectively analyzed 772 HCC patients. Antiplatelet therapy was defined as the regular intake of aspirin or clopidogrel from HCC diagnosis through to an endpoint of either overall survival (OS) or liver-related death. Overall survival, liver-related death, tumor progression, Child-Pugh deterioration and hemorrhage were analyzed for patients who either had or had not undertaken antiplatelet therapy.
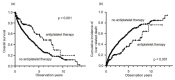
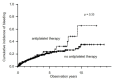
Results: The numbers of patients who did and did not undertake antiplatelet therapy were 111 and 661, respectively. Patients who undertook antiplatelet therapy were older and had better liver function at diagnosis. Antiplatelet therapy resulted in significant improvements in OS (p < 0.01) and lower risk of liver-related death (p < 0.01). Multivariate Cox regression analysis revealed that antiplatelet therapy had a significant negative association with liver-related death (hazard ratio (HR): 0.64, 95% confidence interval (CI): 0.44-0.93, p = 0.02). In patients who underwent transcatheter arterial chemoembolization (TACE) as the first treatment, antiplatelet therapy prevented tumor progression (p < 0.01) and Child-Pugh deterioration (p < 0.01). Antiplatelet therapy did not increase the risk of hemorrhagic events.
Conclusions: Antiplatelet therapy reduced liver-related death and improved OS safely in HCC patients.
Keywords: antiplatelet therapy; hepatocellular carcinoma; prognosis.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures


Similar articles
-
Antiplatelet Therapy is Associated with a Better Prognosis for Patients with Hepatitis B Virus-Related Hepatocellular Carcinoma after Liver Resection.Ann Surg Oncol. 2016 Dec;23(Suppl 5):874-883. doi: 10.1245/s10434-016-5520-9. Epub 2016 Aug 19. Ann Surg Oncol. 2016. PMID: 27541812
-
Antiplatelet therapy and the risk of hepatocellular carcinoma in chronic hepatitis B patients on antiviral treatment.Hepatology. 2017 Nov;66(5):1556-1569. doi: 10.1002/hep.29318. Epub 2017 Sep 29. Hepatology. 2017. PMID: 28617992
-
[Comparison of therapeutics effects of transcatheter arterial chemoembolization combined with iodine-125 seed implantation and sorafenib for the treatment of hepatocellular carcinoma with portal vein tumor thrombosis].Zhonghua Gan Zang Bing Za Zhi. 2018 Apr 20;26(4):298-304. doi: 10.3760/cma.j.issn.1007-3418.2018.04.013. Zhonghua Gan Zang Bing Za Zhi. 2018. PMID: 29996343 Chinese.
-
Transarterial chemoembolization versus hepatic resection in hepatocellular carcinoma treatment: a meta-analysis.Drug Des Devel Ther. 2015 Aug 10;9:4431-40. doi: 10.2147/DDDT.S86629. eCollection 2015. Drug Des Devel Ther. 2015. PMID: 26309396 Free PMC article. Review.
-
Liver resection versus transarterial chemoembolization for the initial treatment of Barcelona Clinic Liver Cancer stage B hepatocellular carcinoma.Hepatol Int. 2018 Sep;12(5):417-428. doi: 10.1007/s12072-018-9888-4. Epub 2018 Aug 2. Hepatol Int. 2018. PMID: 30073454
Cited by
-
Ensemble learning enhances the precision of preliminary detection of primary hepatocellular carcinoma based on serological and demographic indices.Front Oncol. 2024 Jun 17;14:1397505. doi: 10.3389/fonc.2024.1397505. eCollection 2024. Front Oncol. 2024. PMID: 38952558 Free PMC article.
-
The role of antiplatelet therapies on incidence and mortality of hepatocellular carcinoma.Eur J Clin Invest. 2023 Jan;53(1):e13870. doi: 10.1111/eci.13870. Epub 2022 Sep 16. Eur J Clin Invest. 2023. PMID: 36075611 Free PMC article.
-
Aspirin in Hepatocellular Carcinoma.Cancer Res. 2021 Jul 15;81(14):3751-3761. doi: 10.1158/0008-5472.CAN-21-0758. Epub 2021 Apr 23. Cancer Res. 2021. PMID: 33893087 Free PMC article. Review.
-
Platelets in Hepatocellular Carcinoma-From Pathogenesis to Targeted Therapy.Cancers (Basel). 2025 Jul 18;17(14):2391. doi: 10.3390/cancers17142391. Cancers (Basel). 2025. PMID: 40723273 Free PMC article. Review.
-
Aspirin in hepatocellular carcinoma: Is it an out-of-date or promising treatment?ILIVER. 2022 Mar 28;1(1):55-64. doi: 10.1016/j.iliver.2022.03.003. eCollection 2022 Mar. ILIVER. 2022. PMID: 40636145 Free PMC article. Review.
References
-
- Yasui Y., Tsuchiya K., Kurosaki M., Takeguchi T., Takeguchi Y., Okada M., Wang W., Kubota Y., Goto T., Komiyama Y., et al. Up-to-seven criteria as a useful predictor for tumor downstaging to within Milan criteria and Child-Pugh grade deterioration after initial conventional transarterial chemoembolization. Hepatol. Res. 2018;48:442–450. doi: 10.1111/hepr.13048. - DOI - PubMed
-
- Iqbal U., Dennis B.B., Li A.A., Cholankeril G., Kim D., Khan M.A., Ahmed A. Use of anti-platelet agents in the prevention of hepatic fibrosis in patients at risk for chronic liver disease: A systematic review and meta-analysis. Hepatol. Int. 2019;13:84–90. doi: 10.1007/s12072-018-9918-2. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

