Technologic advances in the assessment and management of obstructive sleep apnoea beyond the apnoea-hypopnoea index: a narrative review
- PMID: 33145074
- PMCID: PMC7578472
- DOI: 10.21037/jtd-sleep-2020-003
Technologic advances in the assessment and management of obstructive sleep apnoea beyond the apnoea-hypopnoea index: a narrative review
Abstract
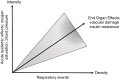
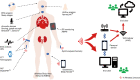
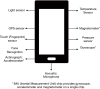
Obstructive sleep apnoea (OSA) is a growing and serious worldwide health problem with significant health and socioeconomic consequences. Current diagnostic testing strategies are limited by cost, access to resources and over reliance on one measure, namely the apnoea-hypopnoea frequency per hour (AHI). Recent evidence supports moving away from the AHI as the principle measure of OSA severity towards a more personalised approach to OSA diagnosis and treatment that includes phenotypic and biological traits. Novel advances in technology include the use of signals such as heart rate variability (HRV), oximetry and peripheral arterial tonometry (PAT) as alternative or additional measures. Ubiquitous use of smartphones and developments in wearable technology have also led to increased availability of applications and devices to facilitate home screening of at-risk populations, although current evidence indicates relatively poor accuracy in comparison with the traditional gold standard polysomnography (PSG). In this review, we evaluate the current strategies for diagnosing OSA in the context of their limitations, potential physiological targets as alternatives to AHI and the role of novel technology in OSA. We also evaluate the current evidence for using newer technologies in OSA diagnosis, the physiological targets such as smartphone applications and wearable technology. Future developments in OSA diagnosis and assessment will likely focus increasingly on systemic effects of sleep disordered breathing (SDB) such as changes in nocturnal oxygen and blood pressure (BP); and may also include other factors such as circulating biomarkers. These developments will likely require a re-evaluation of the diagnostic and grading criteria for clinically significant OSA.
Keywords: Obstructive sleep apnoea (OSA); beyond the apnoea-hypopnoea index (beyond the AHI); diagnosis; screening; smartphones; wearable technology.
2020 Journal of Thoracic Disease. All rights reserved.
Conflict of interest statement
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (Available at http://dx.doi.org/10.21037/jtd-sleep-2020-003). JFG reports that he has been a member of the European medical advisory board for BresoTec. WTM McNicholas serves as an unpaid Section Director of Sleep Section and an unpaid editorial board member of Journal of Thoracic Disease. The authors have no other conflicts of interest to declare.
Figures
References
Publication types
LinkOut - more resources
Full Text Sources
