Differential type I interferon response and primary airway neutrophil extracellular trap release in children with acute respiratory distress syndrome
- PMID: 33149247
- PMCID: PMC7642368
- DOI: 10.1038/s41598-020-76122-1
Differential type I interferon response and primary airway neutrophil extracellular trap release in children with acute respiratory distress syndrome
Abstract
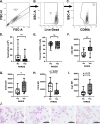
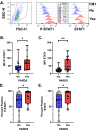
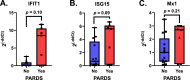
Acute respiratory distress syndrome (ARDS) is a heterogeneous condition characterized by the recruitment of large numbers of neutrophils into the lungs. Neutrophils isolated from the blood of adults with ARDS have elevated expression of interferon (IFN) stimulated genes (ISGs) associated with decreased capacity of neutrophils to kill Staphylococcus aureus and worse clinical outcomes. Neutrophil extracellular traps (NETs) are elevated in adults with ARDS. Whether pediatric ARDS (PARDS) is similarly associated with altered neutrophil expression of ISGs and neutrophil extracellular trap release is not known. Tracheal aspirate fluid and cells were collected within 72 h from seventy-seven intubated children. Primary airway neutrophils were analyzed for differential ISG expression by PCR, STAT1 phosphorylation and markers of degranulation and activation by flow cytometry. Airway fluid was analyzed for the release of NETs by myeloperoxidase-DNA complexes using an ELISA. Higher STAT1 phosphorylation, markers of neutrophil degranulation, activation and NET release were found in children with versus without PARDS. Higher NETs were detected in the airways of children with ventilator-free days less than 20 days. Increased airway cell IFN signaling, neutrophil activation, and NET production is associated with PARDS. Higher levels of airway NETs are associated with fewer ventilator-free days.
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
Neutrophil Extracellular Traps Are Elevated in Patients with Pneumonia-related Acute Respiratory Distress Syndrome.Anesthesiology. 2019 Apr;130(4):581-591. doi: 10.1097/ALN.0000000000002619. Anesthesiology. 2019. PMID: 30676417
-
Carnosic acid inhibits reactive oxygen species-dependent neutrophil extracellular trap formation and ameliorates acute respiratory distress syndrome.Life Sci. 2023 May 15;321:121334. doi: 10.1016/j.lfs.2022.121334. Epub 2022 Dec 30. Life Sci. 2023. PMID: 36587789
-
Bacteria-specific neutrophil dysfunction associated with interferon-stimulated gene expression in the acute respiratory distress syndrome.PLoS One. 2011;6(7):e21958. doi: 10.1371/journal.pone.0021958. Epub 2011 Jul 6. PLoS One. 2011. PMID: 21755013 Free PMC article.
-
Progression of Cystic Fibrosis Lung Disease from Childhood to Adulthood: Neutrophils, Neutrophil Extracellular Trap (NET) Formation, and NET Degradation.Genes (Basel). 2019 Feb 26;10(3):183. doi: 10.3390/genes10030183. Genes (Basel). 2019. PMID: 30813645 Free PMC article. Review.
-
A Narrative Review: The Role of NETs in Acute Respiratory Distress Syndrome/Acute Lung Injury.Int J Mol Sci. 2024 Jan 25;25(3):1464. doi: 10.3390/ijms25031464. Int J Mol Sci. 2024. PMID: 38338744 Free PMC article. Review.
Cited by
-
Cluster analysis and profiling of airway fluid metabolites in pediatric acute hypoxemic respiratory failure.Sci Rep. 2021 Nov 26;11(1):23019. doi: 10.1038/s41598-021-02354-4. Sci Rep. 2021. PMID: 34836982 Free PMC article.
-
Type I IFN-mediated NET release promotes Mycobacterium tuberculosis replication and is associated with granuloma caseation.Cell Host Microbe. 2024 Dec 11;32(12):2092-2111.e7. doi: 10.1016/j.chom.2024.11.008. Epub 2024 Dec 4. Cell Host Microbe. 2024. PMID: 39637864
-
Neutrophil responsiveness to IL-10 impairs clearance of Streptococcus pneumoniae from the lungs.J Leukoc Biol. 2024 Jan 5;115(1):4-15. doi: 10.1093/jleuko/qiad070. J Leukoc Biol. 2024. PMID: 37381945 Free PMC article.
-
Endothelial Damage in Acute Respiratory Distress Syndrome.Int J Mol Sci. 2020 Nov 20;21(22):8793. doi: 10.3390/ijms21228793. Int J Mol Sci. 2020. PMID: 33233715 Free PMC article. Review.
-
Expression Patterns of Airway Fluid Cytokines From Intubated Children With Pediatric Acute Respiratory Distress Syndrome.Crit Care Explor. 2022 Dec 14;4(12):e0819. doi: 10.1097/CCE.0000000000000819. eCollection 2022 Dec. Crit Care Explor. 2022. PMID: 36567781 Free PMC article.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

