A Retrospective Analysis of Children and Adolescents With Diabetic Ketoacidosis in the Intensive Care Unıt: Is It Significant that the Blood Ketone Level Becomes Negative in Diabetic Ketoacidosis?
- PMID: 33178500
- PMCID: PMC7651777
- DOI: 10.7759/cureus.10844
A Retrospective Analysis of Children and Adolescents With Diabetic Ketoacidosis in the Intensive Care Unıt: Is It Significant that the Blood Ketone Level Becomes Negative in Diabetic Ketoacidosis?
Abstract
Introduction: Diabetic ketoacidosis (DKA) is the most common cause of acute morbidity and mortality in children and adolescents with type 1 diabetes mellitus (T1DM). Because DKA management is associated with complications, endocrine communities have published guidelines and attempted to set standards for DKA diagnosis and management worldwide. In this study, for the patients followed up in the intensive care unit who have been treated according to DKA protocols, clinical and laboratory characteristics, differences between new and old diagnosed patients, and results of treatment were evaluated.
Methods: The records of 67 patients hospitalized in the pediatric intensive care unit for the past two years were reviewed retrospectively. Patients were grouped as newly diagnosed and old diagnosed diabetics.
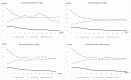
Results: The mean age of the patients was 8.66 ± 5.0 years (3 months to 17.9 years) and 39 (58.2%) were male. Forty-five patients (67.1%) presented with mild DKA and 22 (33.9%) with severe DKA. Fourteen (63.6%) of the severe DKA cases were newly diagnosed with T1DM. Six patients had hyponatremia (corrected serum Na level <135 mmol/L) and five had hypernatremia (serum Na level >145 mmol/L). Only one of the hyponatremic patients had severe acidosis, while four of the hypernatremic patients had severe acidosis. At the 14th hour, blood glucose levels were below 200 mg/dl, blood ketones became negative in 5.8 hours, and at 9.1 hours, blood pH and/or HCO3 levels were normalized, recovery criteria were completed, and subcutaneous (SC) insulin injection was started. Of the patients, 38 (56.7) were newly diagnosed with T1DM. The mean age of newly diagnosed T1DM patients was smaller (7.40 ± 4.96) than those with old diagnosis, respiratory rates (RRs) were higher and pCO2 levels were lower on admission. Blood glucose, blood ketone negativity, acidosis, and Glasgow coma score (GCS) scores of the newly diagnosed T1DM patients improved later than the previous diagnoses. Only one patient under two years of age with a pH of 6.89 was given HCO3. None of the patients had symptomatic brain edema and death.
Conclusions: As a result, DKA is an acute and serious complication of diabetes, whose results are promising when managed only with minimal individual changes according to guidelines. Bicarbonate administration is not needed except in patients with very severe acidosis. Bedside blood ketone monitoring seems to be important because it allows for early enteral feeding.
Keywords: diabetic ketoasidosis; dibetes mellitus; ketone.
Copyright © 2020, Kangin et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
Similar articles
-
[Frequency and clinical manifestation of diabetic ketoacidosis in children with newly diagnosed type 1 diabetes].Pediatr Endocrinol Diabetes Metab. 2013;19(4):143-7. Pediatr Endocrinol Diabetes Metab. 2013. PMID: 25612814 Polish.
-
Diabetic Ketoacidosis at the Onset of Type 1 Diabetes Mellitus Among Children and Adolescents in Jeddah, Saudi Arabia: A Study From the Emergency Department.Cureus. 2022 Apr 25;14(4):e24456. doi: 10.7759/cureus.24456. eCollection 2022 Apr. Cureus. 2022. PMID: 35651441 Free PMC article.
-
Impact of the COVID-19 pandemic on diabetic ketoacidosis management in the pediatric intensive care unit.Acute Crit Care. 2023 Aug;38(3):371-379. doi: 10.4266/acc.2023.00038. Epub 2023 Aug 31. Acute Crit Care. 2023. PMID: 37652866 Free PMC article.
-
Diabetic acidosis with severe fetal hypoxia in pregnancy: Narrative review and case study.Int J Gynaecol Obstet. 2024 Oct;167(1):105-108. doi: 10.1002/ijgo.15593. Epub 2024 May 15. Int J Gynaecol Obstet. 2024. PMID: 38747012 Review.
-
Diabetic ketoacidosis: risk factors and management strategies.Treat Endocrinol. 2003;2(2):95-108. doi: 10.2165/00024677-200302020-00003. Treat Endocrinol. 2003. PMID: 15871546 Review.
Cited by
-
Relationship Between Bedside Ketone Levels and Time to Resolution of Diabetic Ketoacidosis: A Retrospective Cohort Study.Diabetes Ther. 2021 Dec;12(12):3055-3066. doi: 10.1007/s13300-021-01167-y. Epub 2021 Oct 9. Diabetes Ther. 2021. PMID: 34628606 Free PMC article.
-
Treatment Outcome and Associated Factors among Type 1 Diabetic Children Admitted with DKA in Bahir Dar City Public Referral Hospital, Northwest, Ethiopia: A Cross-sectional Study.Glob Pediatr Health. 2024 Apr 23;11:2333794X241248320. doi: 10.1177/2333794X241248320. eCollection 2024. Glob Pediatr Health. 2024. PMID: 38660690 Free PMC article.
References
-
- Diabetic ketoacidosis in infants, children, and adolescents: a consensus statement from the American Diabetes Association. Wolfsdorf J, Glaser N, Sperling MA, American Diabetes Association. Diabetes Care. 2006 May;29:1150–1159. - PubMed
-
- ISPAD Clinical Practice Consensus Guidelines 2018: diabetic ketoacidosis and the hyperglycemic hyperosmolar state. Wolfsdorf JI, Glaser N, Agus M, et al. Pediatr Diabetes. 2018;27:155–177. - PubMed
-
- Incidence of type 1 diabetes mellitus during 26 years of observation and prevalence of diabetic ketoacidosis in the later years. Wojcik M, Sudacka M, Wasyl B, Ciechanowska M, Nazim J, Stelmach M, Starzyk JB. Eur J Pediatr. 2015;174:1319–1324. - PubMed
-
- Diabetic ketoacidosis at diagnosis in Austrian children in 1989-2008: a population-based analysis. Schober E, Rami B, Waldhoer T, Austrian Diabetes Incidence Study Group. Diabetologia. 2010;53:1057–1061. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous