Long-Term Anticoagulation in Secondary Ischemic Stroke Prevention: The Prospective Multicenter RESTAIC Registry
- PMID: 33193025
- PMCID: PMC7641639
- DOI: 10.3389/fneur.2020.575634
Long-Term Anticoagulation in Secondary Ischemic Stroke Prevention: The Prospective Multicenter RESTAIC Registry
Abstract
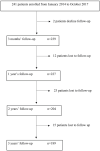
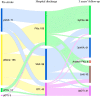
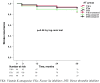
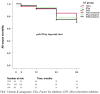
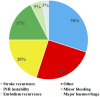
Background and Objective: Oral anticoagulation (OAC) for secondary stroke prevention is recommended in atrial fibrillation (AF) and other sources of cardioembolic stroke. Our objectives were to explore the differences in ischemic and hemorrhagic events when using OAC for secondary stroke prevention according to the type of anticoagulant treatment and to analyze the number and reasons for OAC switches during long-term follow-up. Methods: Ischemic stroke (IS) patients who were discharged on OAC for secondary stroke prevention from January 2014 to October 2017 were recruited in a prospective, multicenter, hospital-based registry. Follow-up at 3 months was scheduled at the outpatient clinic with subsequent annual phone interviews for 3 years. Patients were classified into three study groups according to OAC at discharge: Vitamin K antagonist (VKA), Factor Xa inhibitor (FXa), or direct thrombin inhibitor (DTI). We compared stroke recurrences, intracranial hemorrhage, major bleeding, and all-cause mortality during the follow-up. We recorded any switches in OAC and the main reasons for the change. Results: A total of 241 patients were included. An anticoagulant was indicated in the presence of a source of cardioembolic stroke in 240 patients (99.6%) and lupus plus antiphospholipid syndrome in one patient. Up to 86 patients (35.6%) were on OAC before the index stroke; in 71 (82.5%) of them, this was VKA. At hospital discharge, 105 were treated with FXa (43.8%), 96 with VKA (39.6%), and 40 with DTI (16.6%). The cumulative incidences at 3 years were 17% for stroke recurrence, 1.6% for intracranial hemorrhage, 4.9% for major hemorrhage, and 22.8% for all-cause mortality, with no differences among the OAC groups in any outcomes. During the follow-up, 40 OAC switches were recorded (63% of them to FXa), mostly due to stroke recurrence. Conclusion: Long-term OAC in secondary stroke prevention is associated with a lower frequency of bleeding complications than stroke recurrences. No differences between anticoagulant drugs were found in any of the analyzed outcomes. The main cause for OAC switch during follow-up was stroke recurrence.
Keywords: anticoagulant drugs; hemorrhage risk; multicenter registry; secondary stroke prevention; stroke recurrence.
Copyright © 2020 Gutiérrez-Zúñiga, Rigual, Torres-Iglesias, Sánchez-Velasco, Alonso de Leciñana, Masjuan, Álvarez Velasco, Navas, Izquierdo-Esteban, Fernández-Ferro, Rodríguez-Pardo, Ruiz-Ares, Zapata-Wainberg, Fuentes and Díez-Tejedor.
Figures
Similar articles
-
Recurrent vascular events in patients with ischemic stroke/TIA and atrial fibrillation in relation to secondary prevention at hospital discharge.Wien Klin Wochenschr. 2004 Dec 30;116(24):834-8. doi: 10.1007/s00508-004-0259-x. Wien Klin Wochenschr. 2004. PMID: 15690967
-
Oral anticoagulant therapy in atrial fibrillation patients at high stroke and bleeding risk.Prog Cardiovasc Dis. 2015 Sep-Oct;58(2):177-94. doi: 10.1016/j.pcad.2015.07.003. Epub 2015 Jul 7. Prog Cardiovasc Dis. 2015. PMID: 26162958 Review.
-
Effect of direct oral anticoagulant for acute major cerebral artery occlusion in cardioembolic stroke/transient ischemic attack patients with non-valvular atrial fibrillation.J Neurol Sci. 2019 Jul 15;402:162-166. doi: 10.1016/j.jns.2019.05.023. Epub 2019 May 23. J Neurol Sci. 2019. PMID: 31152970
-
Three-month risk-benefit profile of anticoagulation after stroke with atrial fibrillation: The SAMURAI-Nonvalvular Atrial Fibrillation (NVAF) study.Int J Stroke. 2016 Jul;11(5):565-74. doi: 10.1177/1747493016632239. Epub 2016 Feb 29. Int J Stroke. 2016. PMID: 26927811
-
Non-vitamin K antagonist oral anticoagulants in cardiovascular disease management: evidence and unanswered questions.J Clin Pharm Ther. 2014 Apr;39(2):118-35. doi: 10.1111/jcpt.12122. Epub 2014 Jan 3. J Clin Pharm Ther. 2014. PMID: 24383983 Review.
Cited by
-
Outcomes of non-vitamin K oral anticoagulants for secondary prevention in ischemic stroke with atrial fibrillation.Sci Rep. 2024 Apr 29;14(1):9838. doi: 10.1038/s41598-024-60660-z. Sci Rep. 2024. PMID: 38684879 Free PMC article.
-
Left Atrial Appendage Occlusion vs Standard of Care After Ischemic Stroke Despite Anticoagulation.JAMA Neurol. 2024 Sep 23;81(11):1150-8. doi: 10.1001/jamaneurol.2024.2882. Online ahead of print. JAMA Neurol. 2024. PMID: 39374446
-
LAA occlusion is effective and safe in very high-risk atrial fibrillation patients with prior stroke: results from the multicentre German LAARGE registry.Clin Res Cardiol. 2024 Oct;113(10):1451-1462. doi: 10.1007/s00392-024-02376-8. Epub 2024 Jan 31. Clin Res Cardiol. 2024. PMID: 38294498 Free PMC article.
-
Untangling areas of improvement in secondary prevention of ischemic stroke in patients with atrial fibrillation.Sci Rep. 2024 Dec 30;14(1):31596. doi: 10.1038/s41598-024-79961-4. Sci Rep. 2024. PMID: 39738279 Free PMC article.
-
Keeping prior anticoagulation treatment in the acute phase of ischaemic stroke: the REKOALA study.J Neurol. 2024 Jul;271(7):4086-4094. doi: 10.1007/s00415-024-12204-8. Epub 2024 Apr 5. J Neurol. 2024. PMID: 38578495 Free PMC article.
References
-
- Kernan WN, Ovbiagele B, Black HR, Bravata DM, Chimowitz MI, Ezekowitz MD, et al. . Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American heart association/American stroke association. Stroke. (2014) 45:2160–236. 10.1161/STR.0000000000000024 - DOI - PubMed
-
- Ruff CT, Giugliano RP, Braunwald E, Hoffman EB, Deenadayalu N, Ezekowitz MD, et al. . Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Lancet. (2014) 383:955–62. 10.1016/S0140-6736(13)62343-0 - DOI - PubMed
-
- Singer DE, O'Brien EC, Peterson ED, Piccini JP, Piccini JP. Factors associated with non–vitamin K antagonist oral anticoagulants for stroke prevention in patients with new-onset atrial fibrillation: results from the outcomes registry for better informed treatment of atrial fibrillation II (ORBIT-AF II). Am Heart J. (2017) 189:40–7. 10.1016/j.ahj.2017.03.024 - DOI - PubMed
LinkOut - more resources
Full Text Sources

