A comparison of protocols for simulating hemorrhage in humans: step versus ramp lower body negative pressure
- PMID: 33211600
- PMCID: PMC7948113
- DOI: 10.1152/japplphysiol.00230.2020
A comparison of protocols for simulating hemorrhage in humans: step versus ramp lower body negative pressure
Abstract
Lower body negative pressure (LBNP) elicits central hypovolemia, and it has been used to simulate the cardiovascular and cerebrovascular responses to hemorrhage in humans. LBNP protocols commonly use progressive stepwise reductions in chamber pressure for specific time periods. However, continuous ramp LBNP protocols have also been utilized to simulate the continuous nature of most bleeding injuries. The aim of this study was to compare tolerance and hemodynamic responses between these two LBNP profiles. Healthy human subjects (N = 19; age, 27 ± 4 y; 7 female/12 male) completed a 1) step LBNP protocol (5-min steps) and 2) continuous ramp LBNP protocol (3 mmHg/min), both to presyncope. Heart rate (HR), mean arterial pressure (MAP), stroke volume (SV), middle and posterior cerebral artery velocity (MCAv and PCAv), cerebral oxygen saturation (ScO2), and end-tidal CO2 (etCO2) were measured. LBNP tolerance, via the cumulative stress index (CSI, summation of chamber pressure × time at each pressure), and hemodynamic responses were compared between the two protocols. The CSI (step: 911 ± 97 mmHg/min vs. ramp: 823 ± 83 mmHg/min; P = 0.12) and the magnitude of central hypovolemia (%Δ SV, step: -54.6% ± 2.6% vs. ramp: -52.1% ± 2.8%; P = 0.32) were similar between protocols. Although there were no differences between protocols for the maximal %Δ HR (P = 0.88), the %Δ MAP during the step protocol was attenuated (P = 0.05), and the reductions in MCAv, PCAv, ScO2, and etCO2 were greater (P ≤ 0.08) when compared with the ramp protocol at presyncope. These results indicate that when comparing cardiovascular responses to LBNP across different laboratories, the specific pressure profile must be considered as a potential confounding factor.NEW & NOTEWORTHY Ramp lower body negative pressure (LBNP) protocols have been utilized to simulate the continuous nature of bleeding injuries. However, it unknown if tolerance or the physiological responses to ramp LBNP are similar to the more common stepwise LBNP protocol. We report similar tolerance between the two protocols, but the step protocol elicited a greater increase in cerebral oxygen extraction in the presence of reduced blood flow, presumably facilitating the matching of metabolic supply and demand.
Keywords: central hypovolemia; cerebral blood velocity; lower body negative pressure.
Conflict of interest statement
The content is solely the responsibility of the authors and does not necessarily represent the official views of the US Department of Defense.
No conflicts of interest, financial or otherwise, are declared by the authors.
Figures
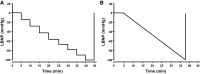




References
-
- Convertino VA. Lower body negative pressure as a tool for research in aerospace physiology and military medicine. J Gravit Physiol 8: 1–14, 2001. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

