Lipohypertrophy in Elderly Insulin-Treated Patients With Type 2 Diabetes
- PMID: 33219928
- PMCID: PMC7843727
- DOI: 10.1007/s13300-020-00954-3
Lipohypertrophy in Elderly Insulin-Treated Patients With Type 2 Diabetes
Abstract
Background: The number of older adults with insulin-treated diabetes mellitus (DM) is steadily increasing worldwide. Errors in the insulin injection technique can lead to skin lipohypertrophy (LH), which is the accumulation of fat cells and fibrin in the subcutaneous tissue. While lipohypertrophic lesions/nodules (LHs) due to incorrect insulin injection techniques are very common, they are often flat and hardly visible and thus require thorough deep palpation examination and ultrasonography (US) for detection. Detection is crucial because such lesions may eventually result in poor diabetes control due to their association with unpredictable insulin release patterns. Skin undergoes fundamental structural changes with aging, possibly increasing the risk for LH. We have therefore investigated the effect of age on the prevalence of LHs and on factors potentially associated with such lesions.
Methods: A total of 1227 insulin-treated outpatients with type 2 DM (T2DM) referred to our diabetes centers were consecutively enrolled in the study. These patients underwent a thorough clinical and US evaluation of the skin at injection sites, as previously described, with up to 95% concordance betweenthe clinical and US screening techniques. Of these 1227 patients, 718 (59%) had LH (LH+) and 509 (41%) were LH-free (LH-). These patients were then assigned to two age class groups (≤ 65 years and > 65 years), and several clinical features, diabetes complication rates, and injection habits were investigated.
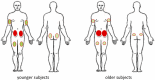
Results: Comparison of the two age subgroups revealed that 396 (48%) and 322 (79%) patients in the younger and older groups, respectively, had LHs (p < 0.001). Compared to the younger subgroup, the older subgroup displayed a higher LH rate in the abdomen (52.9 vs. 38.3%; p < 0.01) and a lower rate in the arms (25.4 vs. 35.8%; p < 0.05), thighs (26.7 vs. 33.4%; p < 0.05), and buttocks (4.9 vs. 26.2%; p < 0.01). In older subjects, the most relevant parameters were: habit of injecting insulin into LH nodules (56 vs. 47% [younger subjects]; p < 0.01), rate of post-injection leakage of insulin from injection site (drop-leaking rate; 47 vs. 39% [younger subjects]; p < 0.05), and rate of painful injections (5 vs. 16% [younger subjects]; p < 0.001). Multivariate analysis showed a stronger association between LH and poor habits, as well as between several clinical parameters, among which the most relevant were hypoglycemic events and glycemic variability.
Discussion: The higher rate of post-injection drop-leaking and pain-free injections might find an explanation in skin changes typically observed in older adults, including lower thickness, vascularity and elasticity, and a more prominent fibrous texture, all of which negatively affect tissue distensibility. Consequently, in addition to the well-known association between aging skin impaired drug absorption rate, aging skin displays a progressively decreasing ability to accommodate large volumes of insulin-containing fluid.
Conclusions: The strong association between LH rate and hypoglycemic events plus glycemic variability suggests the need (1) to take specific actions to prevent and control the high risk of acute cardiovascular events expected to occur in older subjects in the case of hypoglycemic events, and (2) to identify suitable strategies to fulfill the difficult task of performing effective educational programs specifically targeted to the elderly.
Trial registration: Trial registration number 172-11:12.2019, Scientific and Ethical Committee of Campania University "Luigi Vanvitelli", Naples, Italy).
Keywords: Ageing; Diabetes; Insulin; Lipohypertrophy; Skin.
Figures
Similar articles
-
Role of Structured Education in Reducing Lypodistrophy and its Metabolic Complications in Insulin-Treated People with Type 2 Diabetes: A Randomized Multicenter Case-Control Study.Diabetes Ther. 2021 May;12(5):1379-1398. doi: 10.1007/s13300-021-01006-0. Epub 2021 Mar 18. Diabetes Ther. 2021. PMID: 33738775 Free PMC article.
-
Insulin-Induced Skin Lipohypertrophy in Type 2 Diabetes: a Multicenter Regional Survey in Southern Italy.Diabetes Ther. 2020 Sep;11(9):2001-2017. doi: 10.1007/s13300-020-00876-0. Epub 2020 Jul 18. Diabetes Ther. 2020. PMID: 32683659 Free PMC article.
-
Errors in insulin treatment management and risk of lipohypertrophy.Acta Diabetol. 2018 Jan;55(1):67-73. doi: 10.1007/s00592-017-1066-y. Epub 2017 Nov 2. Acta Diabetol. 2018. PMID: 29098390
-
Lipohypertrophy and Insulin: An Old Dog That Needs New Tricks.Endocr Pract. 2023 Aug;29(8):670-677. doi: 10.1016/j.eprac.2023.04.006. Epub 2023 Apr 23. Endocr Pract. 2023. PMID: 37098370 Review.
-
Worldwide Injection Technique Questionnaire Study: Injecting Complications and the Role of the Professional.Mayo Clin Proc. 2016 Sep;91(9):1224-30. doi: 10.1016/j.mayocp.2016.06.012. Mayo Clin Proc. 2016. PMID: 27594186 Review.
Cited by
-
Role of Structured Education in Reducing Lypodistrophy and its Metabolic Complications in Insulin-Treated People with Type 2 Diabetes: A Randomized Multicenter Case-Control Study.Diabetes Ther. 2021 May;12(5):1379-1398. doi: 10.1007/s13300-021-01006-0. Epub 2021 Mar 18. Diabetes Ther. 2021. PMID: 33738775 Free PMC article.
-
Unveiling Diabetes: Categories, Genetics, Diagnostics, Treatments, and Future Horizons.Curr Diabetes Rev. 2024;20(4):e180823219972. doi: 10.2174/1573399820666230818092958. Curr Diabetes Rev. 2024. PMID: 37594107 Review.
-
Bruising: A Neglected, Though Patient-Relevant Complication of Insulin Injections Coming to Light from a Real-Life Nationwide Survey.Diabetes Ther. 2021 Apr;12(4):1143-1157. doi: 10.1007/s13300-021-01026-w. Epub 2021 Mar 9. Diabetes Ther. 2021. PMID: 33687646 Free PMC article.
-
Lipohypertrophy and Insulin: An Update From the Diabetes Technology Society.J Diabetes Sci Technol. 2023 Nov;17(6):1711-1721. doi: 10.1177/19322968231187661. Epub 2023 Aug 9. J Diabetes Sci Technol. 2023. PMID: 37555266 Free PMC article.
-
The Durability of an Intensive, Structured Education-Based Rehabilitation Protocol for Best Insulin Injection Practice: The ISTERP-2 Study.Diabetes Ther. 2021 Sep;12(9):2557-2569. doi: 10.1007/s13300-021-01108-9. Epub 2021 Aug 12. Diabetes Ther. 2021. PMID: 34383261 Free PMC article.
References
-
- World Health Organization, National Institute on Aging, National Institutes of Health, US Department of Health and Human Services. Global health and aging. https://www.who.int/ageing/publications/global_health.pdf. Accessed 25 Mar 2020.
Publication types
LinkOut - more resources
Full Text Sources

