Preventive malaria treatment among school-aged children in sub-Saharan Africa: a systematic review and meta-analyses
- PMID: 33222799
- PMCID: PMC7721819
- DOI: 10.1016/S2214-109X(20)30325-9
Preventive malaria treatment among school-aged children in sub-Saharan Africa: a systematic review and meta-analyses
Abstract
Background: The burden of malaria infection in sub-Saharan Africa among school-aged children aged 5-15 years is underappreciated and represents an important source of human-to-mosquito transmission of Plasmodium falciparum. Additional interventions are needed to control and eliminate malaria. We aimed to assess whether preventive treatment of malaria might be an effective means of reducing P falciparum infection and anaemia in school-aged children and lowering parasite transmission.
Methods: In this systematic review and two meta-analyses, we searched the online databases PubMed, Embase, Cochrane CENTRAL, and Clinicaltrials.gov for intervention studies published between Jan 1, 1990, and Dec 14, 2018. We included randomised studies that assessed the effect of antimalarial treatment among asymptomatic school-aged children aged 5-15 years in sub-Saharan Africa on prevalence of P falciparum infection and anaemia, clinical malaria, and cognitive function. We first extracted data for a study-level meta-analysis, then contacted research groups to request data for an individual participant data meta-analysis. Outcomes of interest included prevalence of P falciparum infection detected by microscopy, anaemia (study defined values or haemoglobin less than age-adjusted and sex-adjusted values), clinical malaria (infection and symptoms on the basis of study-specific definitions) during follow-up, and code transmission test scores. We assessed effects by treatment type and duration of time protected, and explored effect modification by transmission setting. For study-level meta-analysis, we calculated risk ratios for binary outcomes and standardised mean differences for continuous outcomes and pooled outcomes using fixed-effect and random-effects models. We used a hierarchical generalised linear model for meta-analysis of individual participant data. This study is registered with PROSPERO, CRD42016030197.
Findings: Of 628 studies identified, 13 were eligible for the study-level meta-analysis (n=16 309). Researchers from 11 studies contributed data on at least one outcome (n=15 658) for an individual participant data meta-analysis. Interventions and study designs were highly heterogeneous; overall risk of bias was low. In the study-level meta-analysis, treatment was associated with reductions in P falciparum prevalence (risk ratio [RR] 0·27, 95% CI 0·17-0·44), anaemia (0·77, 0·65-0·91), and clinical malaria (0·40, 0·28-0·56); results for cognitive outcomes are not presented because data were only available for three trials. In our individual participant data meta-analysis, we found treatment significantly decreased P falciparum prevalence (adjusted RR [ARR] 0·46, 95% CI 0·40-0·53; p<0·0001; 15 648 individuals; 11 studies), anaemia (ARR 0·85, 0·77-0·92; p<0·0001; 15 026 individuals; 11 studies), and subsequent clinical malaria (ARR 0·50, 0·39-0·60; p<0·0001; 1815 individuals; four studies) across transmission settings. We detected a marginal effect on cognitive function in children older than 10 years (adjusted mean difference in standardised test scores 0·36, 0·01-0·71; p=0·044; 3962 individuals; five studies) although we found no significant effect when combined across all ages.
Interpretation: Preventive treatment of malaria among school-aged children significantly decreases P falciparum prevalence, anaemia, and risk of subsequent clinical malaria across transmission settings. Policy makers and programme managers should consider preventive treatment of malaria to protect this age group and advance the goal of malaria elimination, while weighing these benefits against potential risks of chemoprevention.
Funding: US National Institutes of Health and Burroughs Wellcome Fund/ASTMH Fellowship.
Copyright © 2020 The Author(s). Published by Elsevier Ltd. This is an Open Access article under the CC BY 4.0 license. Published by Elsevier Ltd.. All rights reserved.
Conflict of interest statement
Declaration of interests
We declare no competing interests.
Figures
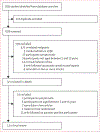



Comment in
-
Back to school for malaria prevention: a new tool in the era of malaria elimination?Lancet Glob Health. 2020 Dec;8(12):e1447-e1448. doi: 10.1016/S2214-109X(20)30347-8. Epub 2020 Oct 22. Lancet Glob Health. 2020. PMID: 33222798 No abstract available.
References
-
- WHO. World malaria report 2019. 2019. https://www.who.int/publications/i/item/world-malaria-report-2019 (accessed March 1, 2020).
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

