A Systemic Literature Review and Meta-Analysis Reporting the Prevalence and Impact of Methicillin-Resistant Staphylococcus aureus Infection in India
- PMID: 33223835
- PMCID: PMC7656882
- DOI: 10.1177/1178633720970569
A Systemic Literature Review and Meta-Analysis Reporting the Prevalence and Impact of Methicillin-Resistant Staphylococcus aureus Infection in India
Abstract
Aim and objective: This systematic review and meta-analysis was conducted to assess the prevalence, burden and epidemiology of methicillin-resistant S. aureus (MRSA). This systemic review was also aimed to highlight the challenges in the diagnosis and management of methicillin-resistant S. aureus (MRSA) in India (for all age groups). We also examined the published literature on the available treatment options and the role of prevention in the management of MRSA in India. By summarizing the currently available data, our objectives were to highlight the need for the prevention of MRSA infections and also emphasize the role of vaccination in the prevention of MRSA infections in India.
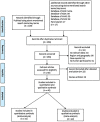
Methodology: Electronic databases such as PubMed and databases of the National Institute of Science Communication and Information Resources and Indian Council of Medical Research Embase were searched for relevant literature published from 2005/01/01 to 2020/05/13 in English language, according to the predefined inclusion and exclusion criteria. A manual search was also conducted using the key term "MRSA 'or' Methicillin Resistant Staphylococcus aureus 'and' India." An independent reviewer extracted data from the studies using a structured Microsoft Excel spreadsheet, and a meta-analysis of proportion for MRSA prevalence with a corresponding 95% confidence interval (CI) for all included individual studies were performed.
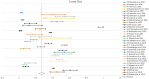
Result: A total of 34 studies involving 16 237 patients were included in the final meta-analysis. The pooled proportion of patients with MRSA infection was 26.8% (95% CI: 23.2%-30.7%). The MRSA infection was more prevalent among male patients (60.4%; 95% CI: 53.9%-66.5%) as compared to female patients (39.6%; 95% CI: 33.5%-46.1%), while the prevalence of MRSA was higher among adults (18 years and above; 32%; 95% CI: 5%-80%) in comparison to pediatric patients (0-18 years; 68%; 95% CI: 20%-94.8%). The degree of heterogeneity was found to be significant.
Conclusion: The prevalence of MRSA in India was relatively high at 27% with a higher proportion observed among men aged >18 years. The high prevalence of MRSA infections in India necessitates the implementation of surveillance and preventive measures to combat the spread of MRSA in both hospital and community settings.
Keywords: India; Methicillin resistant S. aureus; prevalence.
© The Author(s) 2020.
Conflict of interest statement
Declaration of conflicting interests:The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
References
LinkOut - more resources
Full Text Sources

