Outcomes of a Series of Patients with Post-Prostatectomy Incontinence Treated with an Adjustable Transobturator Male System or Artificial Urinary Sphincter
- PMID: 33230712
- PMCID: PMC7854436
- DOI: 10.1007/s12325-020-01563-z
Outcomes of a Series of Patients with Post-Prostatectomy Incontinence Treated with an Adjustable Transobturator Male System or Artificial Urinary Sphincter
Abstract
Introduction: A prospective evaluation of outcomes in a series of patients with post-prostatectomy incontinence (PPI) treated with two different devices is presented.
Methods: Consecutive patients with PPI underwent interventions with an adjustable transobturator male system (ATOMS) or artificial urinary sphincter (AUS). Decisions were based on patient preference after physician counselling. Patient characteristics and operative and postoperative parameters including dryness, satisfaction, complications, revision and device durability were evaluated.
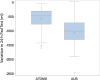
Results: One hundred twenty-nine patients were included: 102 (79.1%) received ATOMS and 27 (20.9%) AUS. Mean follow-up was 34.9 ± 15.9 months. No difference was observed between patient age (p = 0.56), ASA score (p = 0.13), Charlson index (p = 0.57) and radiation (p = 0.3). BMI was higher for AUS (27.1 vs. 29.7; p = 0.003) and also baseline incontinence severity (7.9% mild, 44.1% moderate and 48% severe for ATOMS vs. 11.1% moderate and 88.9% severe for AUS; p = 0.0007). Differential pad test was higher for AUS (- 470 vs. - 1000 ml; p < 0.0001) and so was ICIQ-SF (15.62 vs. 18.3; p < 0.001), but total dryness (76.5 vs. 66.7%; p = 0.33), social continence (90.2 vs. 85.2%; p = 0.49) and satisfaction (92.2 vs. 88.9%; p = 0.69) were equivalent. The postoperative complication rate was similar (22.6 vs. 29.6%; p = 0.4). The surgical revision rate was higher for AUS (6.9 vs. 22.2%; p = 0.029) and also the explant rate but did not reach statistical significance (4.9 vs. 14.8%; p = 0.09). Time to explant was shorter for AUS (log-rank p = 0.021). Regression analysis revealed radiation (p = 0.003) and incontinence severity (p = 0.029) predict total dryness, while complications (p < 0.005) and type of device (p = 0.039) independently predict surgical revision.
Conclusions: Both ATOMS and AUS are effective devices. Pad test change for AUS exceeds that of ATOMS. The revision rate is higher for AUS, and durability is superior for ATOMS. The satisfaction rate is equivalent. Larger series and longer follow-up are needed to compare both devices more appropriately. According to our experience, the AUS is not the only gold standard for PPI.
Keywords: Adjustable transobturator male system; Artificial urinary sphincter; Effectiveness; Post-prostatectomy incontinence; Safety; Urology.
Figures



Similar articles
-
Artificial urinary sphincter significantly better than fixed sling for moderate post-prostatectomy stress urinary incontinence: a propensity score-matched study.BJU Int. 2021 Feb;127(2):229-237. doi: 10.1111/bju.15197. Epub 2020 Aug 26. BJU Int. 2021. PMID: 32744793
-
Artificial urinary sphincter or a second adjustable transobturator male system offer equivalent outcomes in patients whom required revision on the initial ATOMS device: An international multi-institutional experience.Neurourol Urodyn. 2021 Mar;40(3):897-909. doi: 10.1002/nau.24646. Epub 2021 Mar 1. Neurourol Urodyn. 2021. PMID: 33645867
-
Adjustable Transobturator Male System after Failed Surgical Devices for Male Stress Urinary Incontinence: A Feasibility Study.Urol Int. 2018;101(1):106-113. doi: 10.1159/000489316. Epub 2018 Jun 28. Urol Int. 2018. PMID: 29953998
-
Effectiveness of Adjustable Transobturator Male System (ATOMS) to Treat Male Stress Incontinence: A Systematic Review and Meta-Analysis.Adv Ther. 2019 Feb;36(2):426-441. doi: 10.1007/s12325-018-0852-4. Epub 2018 Dec 17. Adv Ther. 2019. PMID: 30560525 Free PMC article.
-
Systematic review and meta-analysis comparing Adjustable Transobturator Male System (ATOMS) and Adjustable Continence Therapy (ProACT) for male stress incontinence.PLoS One. 2019 Dec 2;14(12):e0225762. doi: 10.1371/journal.pone.0225762. eCollection 2019. PLoS One. 2019. PMID: 31790490 Free PMC article.
Cited by
-
ATOMS (Adjustable Trans-Obturator Male System) in Patients with Post-Prostatectomy Incontinence and Previously Treated Urethral Stricture or Bladder Neck Contracture.J Clin Med. 2022 Aug 19;11(16):4882. doi: 10.3390/jcm11164882. J Clin Med. 2022. PMID: 36013121 Free PMC article.
-
Efficacy of surgical treatment for post-prostatectomy urinary incontinence: a systematic review and network meta-analysis.Int J Surg. 2023 Mar 1;109(3):401-411. doi: 10.1097/JS9.0000000000000170. Int J Surg. 2023. PMID: 36912884 Free PMC article.
-
Outcomes with the Adjustable Transobturator Male System (ATOMS) for the Treatment of Male Stress Urinary Incontinence After Prostate Surgery and the Impact of Previous Radiotherapy.Eur Urol Open Sci. 2024 Mar 4;62:68-73. doi: 10.1016/j.euros.2024.02.016. eCollection 2024 Apr. Eur Urol Open Sci. 2024. PMID: 38468862 Free PMC article.
-
Results of Adjustable Trans-Obturator Male System for Stress Urinary Incontinence after Transurethral Resection or Holmium Laser Enucleation of the Prostate: International Multicenter Study.J Clin Med. 2024 Aug 7;13(16):4628. doi: 10.3390/jcm13164628. J Clin Med. 2024. PMID: 39200769 Free PMC article.
-
Complications of Prostate Cancer Treatment: Open Issues.J Clin Med. 2024 May 24;13(11):3090. doi: 10.3390/jcm13113090. J Clin Med. 2024. PMID: 38892801 Free PMC article.
References
-
- Averbeck MA, Marcelissen T, Anding R, Rahnama'i MS, Sahai A, Tubaro A. How can we prevent postprostatectomy urinary incontinence by patient selection, and by preoperative, peroperative, and postoperative measures? International Consultation on Incontinence-Research Society 2018. Neurourol Urodyn. 2019;38(Suppl 5):S119–S126. - PubMed
-
- Van der Aa F, Drake MJ, Kasyan GR, Petrolekas A, Cornu JN, Young Academic Urologists Functional Urology Group The artificial urinary sphincter after a quarter of a century: a critical systematic review of its use in male non-neurogenic incontinence. Eur Urol. 2013;63:681–689. doi: 10.1016/j.eururo.2012.11.034. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

