Meta-analysis of echocardiographic quantification of left ventricular filling pressure
- PMID: 33230957
- PMCID: PMC7835555
- DOI: 10.1002/ehf2.13119
Meta-analysis of echocardiographic quantification of left ventricular filling pressure
Abstract
Aims: The clinical reliability of echocardiographic surrogate markers of left ventricular filling pressures (LVFPs) across different cardiovascular pathologies remains unanswered. The main objective was to evaluate the evidence of how effectively different echocardiographic indices estimate true LVFP.
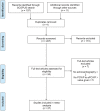
Methods and results: Design: this is a systematic review and meta-analysis.
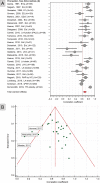
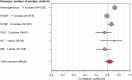
Data source: Scopus, PubMed and Embase. Eligibility criteria for selecting studies were those that used echocardiography to predict or estimate pulmonary capillary wedge pressure or left ventricular end-diastolic pressures. Twenty-seven studies met criteria. Only eight studies (30%) reported both correlation coefficient and bias between non-invasive and invasively measured LVFPs. The majority of studies (74%) recorded invasive pulmonary capillary wedge pressure as a surrogate for left ventricular end-diastolic pressures. The pooled correlation coefficient overall was r = 0.69 [95% confidence interval (CI) 0.63-0.75, P < 0.01]. Evaluation by cohort demonstrated varying association: heart failure with preserved ejection fraction (11 studies, n = 575, r = 0.59, 95% CI 0.53-0.64) and heart failure with reduced ejection fraction (8 studies, n = 381, r = 0.67, 95% CI 0.61-0.72).
Conclusions: Echocardiographic indices show moderate pooled association to invasively measured LVFP; however, this varies widely with disease state. In heart failure with preserved ejection fraction, no single echocardiography-based metric offers a reliable estimate. In heart failure with reduced ejection fraction, mitral inflow-derived indices (E/e', E/A, E/Vp, and EDcT) have reasonable clinical applicability. While an integrated approach of several echocardiographic metrics provides the most promise for estimating LVFP reliably, such strategies need further validation in larger, patient-specific studies.
Keywords: Echocardiography; Invasive heart catheterization; Left ventricular end-diastolic pressure.
© 2020 The Authors. ESC Heart Failure published by John Wiley & Sons Ltd on behalf of European Society of Cardiology.
Conflict of interest statement
None declared.
Figures


Similar articles
-
Correlation with invasive left ventricular filling pressures and prognostic relevance of the echocardiographic diastolic parameters used in the 2016 ESC heart failure guidelines and in the 2016 ASE/EACVI recommendations: a systematic review in patients with heart failure with preserved ejection fraction.Eur J Heart Fail. 2018 Sep;20(9):1303-1311. doi: 10.1002/ejhf.1220. Epub 2018 Jun 7. Eur J Heart Fail. 2018. PMID: 29877602
-
Echocardiographic estimation of left ventricular and pulmonary pressures in patients with heart failure and preserved ejection fraction: a study utilizing simultaneous echocardiography and invasive measurements.Eur J Heart Fail. 2017 Dec;19(12):1651-1660. doi: 10.1002/ejhf.957. Epub 2017 Oct 6. Eur J Heart Fail. 2017. PMID: 28984057
-
Echocardiographic indices do not reliably track changes in left-sided filling pressure in healthy subjects or patients with heart failure with preserved ejection fraction.Circ Cardiovasc Imaging. 2011 Sep;4(5):482-9. doi: 10.1161/CIRCIMAGING.110.960575. Epub 2011 Jul 25. Circ Cardiovasc Imaging. 2011. PMID: 21788358 Free PMC article.
-
Evaluation of elevated left ventricular end diastolic pressure in patients with preserved ejection fraction using cardiac magnetic resonance.Eur Radiol. 2019 May;29(5):2360-2368. doi: 10.1007/s00330-018-5955-4. Epub 2019 Jan 10. Eur Radiol. 2019. PMID: 30631923
-
Left atrial strain: a new parameter for assessment of left ventricular filling pressure.Heart Fail Rev. 2016 Jan;21(1):65-76. doi: 10.1007/s10741-015-9520-9. Heart Fail Rev. 2016. PMID: 26687372 Review.
Cited by
-
Improved diastolic dysfunction is associated with higher forward flow and better prognosis in chronic heart failure.Int J Cardiovasc Imaging. 2022 Apr;38(4):727-737. doi: 10.1007/s10554-021-02457-z. Epub 2021 Nov 2. Int J Cardiovasc Imaging. 2022. PMID: 34727251
-
Evaluation of Mortality and Hospitalization Due to Decompensated Heart Failure and Appropriate Shocks in Reduced Ejection Fraction in Patients with an Implantable Cardioverter-Defibrillator According to a Novel Tissue Doppler Echocardiographic Method.J Clin Med. 2025 May 6;14(9):3226. doi: 10.3390/jcm14093226. J Clin Med. 2025. PMID: 40364256 Free PMC article.
-
Effects of left atrial function on pulmonary arterial pressure in acute myocardial infarction, hypertrophic and dilated cardiomyopathy.BMC Cardiovasc Disord. 2022 Nov 26;22(1):507. doi: 10.1186/s12872-022-02952-8. BMC Cardiovasc Disord. 2022. PMID: 36435744 Free PMC article.
-
External validation of artificial intelligence for detection of heart failure with preserved ejection fraction.Nat Commun. 2025 Mar 25;16(1):2915. doi: 10.1038/s41467-025-58283-7. Nat Commun. 2025. PMID: 40133291 Free PMC article.
-
Cardiac Magnetic Resonance Left Ventricular Filling Pressure Is Associated with NT-proBNP in Patients with New Onset Heart Failure.Medicina (Kaunas). 2023 Oct 30;59(11):1924. doi: 10.3390/medicina59111924. Medicina (Kaunas). 2023. PMID: 38003973 Free PMC article.
References
-
- Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, Falk V, González‐Juanatey JR, Harjola V‐P, Jankowska EA, Jessup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GMC, Ruilope LM, Ruschitzka F, Rutten FH, Van der Meer P, ESC Scientific Document Group . 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J 2016; 37: 2129–2200. - PubMed
-
- Brienesse SC, Davies AJ, Khan A, Boyle AJ. Prognostic value of LVEDP in acute myocardial infarction: a systematic review and meta‐analysis. J Cardiovasc Transl Res 2018; 11: 33–35. - PubMed
-
- Fruhwald FM, Dusleag J, Eber B, Fruhwald S, Zweiker R, Klein W. Long‐term outcome and prognostic factors in dilated cardiomyopathy. Preliminary results. Angiology 1994; 45: 763–770. - PubMed
-
- Nagendran J, Norris CM, Appoo JJ, Ross DB, Nagendran J. Alberta Provincial Project for Outcome Assessment in Coronary Heart Disease (APPROACH) Investigators. Left ventricular end‐diastolic pressure predicts survival in coronary artery bypass graft surgery patients. Ann Thorac Surg 2014; 97: 1343–1347. - PubMed
-
- Satpathy C, Mishra TK, Satpathy R, Satpathy HK, Barone EJ. Diagnosis and management of diastolic dysfunction and heart failure. American family physician 2006; 73: 841–846. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

