Factors explaining variation in recommended care pathways following hospital-presenting self-harm: a multilevel national registry study
- PMID: 33234189
- PMCID: PMC7745229
- DOI: 10.1192/bjo.2020.116
Factors explaining variation in recommended care pathways following hospital-presenting self-harm: a multilevel national registry study
Abstract
Background: People who present to hospital following self-harm are at high risk of suicide. Despite this, there are considerable variations in the management of this group across hospitals and the factors influencing such variations are not well understood.
Aims: The aim of this study was to identify the specific hospital and individual factors associated with care pathways following hospital-presenting self-harm.
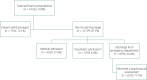
Method: Data on presentations to hospitals by those aged 18 years and over were obtained from the National Self-Harm Registry Ireland for 2017 and 2018. Factors associated with four common outcomes following self-harm (self-discharge, medical and psychiatric admission and psychosocial assessment before discharge) were examined using multilevel Poisson regression models.
Results: Care pathways following self-harm varied across hospitals and were influenced by both hospital and individual factors. Individual factors were primarily associated with self-discharge (including male gender, younger age and alcohol involvement), medical admission (older age, drug overdose as a sole method and ambulance presentations) and psychiatric admission (male gender, methods associated with greater lethality and older age). The hospital admission rate for self-harm was the only factor associated with all outcomes examined. The availability of psychiatric in-patient facilities and specialist mental health staff contributed to variation in psychiatric admissions and psychosocial assessments prior to discharge. Hospital factors explained the majority of observed variation in the provision of psychosocial assessments.
Conclusions: Characteristics of the presenting hospital and hospital admission rates influence the recommended care pathways following self-harm. Provision of onsite mental health facilities and specialist mental health staff has a strong impact on psychiatric care of these patients.
Keywords: Self-harm; emergency psychiatry; emergency services; hospital services; outpatient treatment.
Conflict of interest statement
None to declare.
Figures

Similar articles
-
Evaluation of a national clinical programme for the management of self-harm in hospital emergency departments: impact on patient outcomes and the provision of care.BMC Psychiatry. 2023 Dec 7;23(1):917. doi: 10.1186/s12888-023-05340-4. BMC Psychiatry. 2023. PMID: 38062378 Free PMC article.
-
Global prevalence of psychosocial assessment following hospital-treated self-harm: systematic review and meta-analysis.BJPsych Open. 2024 Jan 11;10(1):e29. doi: 10.1192/bjo.2023.625. BJPsych Open. 2024. PMID: 38205598 Free PMC article. Review.
-
Factors associated with the non-assessment of self-harm patients attending an Accident and Emergency Department: results of a national study.J Affect Disord. 2005 Dec;89(1-3):91-7. doi: 10.1016/j.jad.2005.08.011. Epub 2005 Oct 13. J Affect Disord. 2005. PMID: 16226810
-
Recommended next care following hospital-treated self-harm: Patterns and trends over time.PLoS One. 2018 Mar 1;13(3):e0193587. doi: 10.1371/journal.pone.0193587. eCollection 2018. PLoS One. 2018. PMID: 29494659 Free PMC article.
-
Systematic reviews of the effectiveness of day care for people with severe mental disorders: (1) acute day hospital versus admission; (2) vocational rehabilitation; (3) day hospital versus outpatient care.Health Technol Assess. 2001;5(21):1-75. doi: 10.3310/hta5210. Health Technol Assess. 2001. PMID: 11532238 Review.
Cited by
-
Indigeneity and Likelihood of Discharge to Psychiatric Hospital in an Australian Deliberate Self-Poisoning Hospital-Treated Cohort.Int J Environ Res Public Health. 2022 Sep 27;19(19):12238. doi: 10.3390/ijerph191912238. Int J Environ Res Public Health. 2022. PMID: 36231541 Free PMC article.
-
Suicide risk following ED presentation with self-harm varies by hospital.Soc Psychiatry Psychiatr Epidemiol. 2024 Jun;59(6):1063-1071. doi: 10.1007/s00127-023-02561-6. Epub 2023 Oct 20. Soc Psychiatry Psychiatr Epidemiol. 2024. PMID: 37861710 Free PMC article.
-
A Multicenter Registry Experience for Suicidal Behaviors in Iran (2019-2022).Arch Iran Med. 2024 Jul 1;27(7):371-378. doi: 10.34172/aim.28558. Arch Iran Med. 2024. PMID: 39072385 Free PMC article.
-
Evaluation of a national clinical programme for the management of self-harm in hospital emergency departments: impact on patient outcomes and the provision of care.BMC Psychiatry. 2023 Dec 7;23(1):917. doi: 10.1186/s12888-023-05340-4. BMC Psychiatry. 2023. PMID: 38062378 Free PMC article.
-
Global prevalence of psychosocial assessment following hospital-treated self-harm: systematic review and meta-analysis.BJPsych Open. 2024 Jan 11;10(1):e29. doi: 10.1192/bjo.2023.625. BJPsych Open. 2024. PMID: 38205598 Free PMC article. Review.
References
-
- National Institute for Health and Care Excellence. Self-harm: The Short-Term Physical and Psychological Management and Secondary Prevention of Self-Harm in Primary and Secondary Care. National Institute for Health and Care Excellence, 2004.
-
- Cassidy E, Arensman E, Keeley HS, Reidy J. Saving Lives and Reducing Harmful Outcomes: Care Systems for Self-Harm and Suicidal Behaviour. National Guidelines for the Assessment and Management of Patients Presenting to Irish Emergency Departments following Self-Harm. Health Service Executive Suicidal Behaviour Working Group, 2012.
-
- Carroll R, Metcalfe C, Gunnell D. Hospital management of self-harm patients and risk of repetition: systematic review and meta-analysis. J Affect Disord 2014; 168: 476–83. - PubMed
-
- Steeg S, Emsley R, Carr M, Cooper J, Kapur N. Routine hospital management of self-harm and risk of further self-harm: propensity score analysis using record-based cohort data. Psychol Med 2018; 48: 315–26. - PubMed
LinkOut - more resources
Full Text Sources

