Comorbid Major Depressive Disorder in Schizophrenia: A Systematic Review and Meta-Analysis
- PMID: 33252130
- PMCID: PMC8451068
- DOI: 10.1093/schbul/sbaa153
Comorbid Major Depressive Disorder in Schizophrenia: A Systematic Review and Meta-Analysis
Abstract
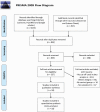
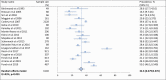
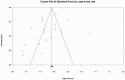
Comorbid major depressive disorder (MDD) in schizophrenia (SZ; SZ-MDD) has been identified as a major prognostic factor. However, the prevalence and associated factors of SZ-MDD have never been explored in a meta-analysis. All studies assessing the prevalence of SZ-MDD in stabilized outpatients with a standardized scale or with structured interviews were included. The Medline, Web of Science, PsycINFO, and Google Scholar databases were searched. Using random effects models, we calculated the pooled estimate of the prevalence of SZ-MDD. We used meta-regression and subgroup analyses to evaluate the potential moderators of the prevalence estimates, and we used the leave-one-out method for sensitivity analyses. Of the 5633 potentially eligible studies identified, 18 studies (n = 6140 SZ stabilized outpatients) were retrieved in the systematic review and included in the meta-analysis. The pooled estimate of the prevalence of SZ-MDD was 32.6% (95% CI: 27.9-37.6); there was high heterogeneity (I2 = 92.6%), and Egger's test did not reveal publication bias (P = .122). The following factors were found to be sources of heterogeneity: publication in or after 2015, the inclusion of patients from larger studies, the assessment tools, the inclusion of patients with substance use disorder or somatic chronic diseases, age, education level, the lifetime number of hospitalizations, and antidepressant use. Two-thirds of the extracted variables could not be explored due to an insufficient amount of published data. The prevalence of MDD is high among SZ individuals. Healthcare providers and public health officials should have an increased awareness of the burden of SZ-MDD.
Keywords: antidepressant; depression; meta-analysis; prevalence; psychiatry; schizophrenia; treatment.
© The Author(s) 2020. Published by Oxford University Press on behalf of the Maryland Psychiatric Research Center.All rights reserved. For permissions, please email: journals.permissions@oup.com.
Figures
Similar articles
-
Co-Morbidity between Major Depression and Schizophrenia: Prevalence and Clinical Characteristics.Psychiatr Danub. 2020 Spring;32(1):78-83. doi: 10.24869/psyd.2020.78. Psychiatr Danub. 2020. PMID: 32303036
-
Remission of depression in patients with schizophrenia and comorbid major depressive disorder: results from the FACE-SZ cohort.Br J Psychiatry. 2018 Aug;213(2):464-470. doi: 10.1192/bjp.2018.87. Epub 2018 Jun 6. Br J Psychiatry. 2018. PMID: 29871707
-
Prevalence and correlates of major depressive disorder, bipolar disorder and schizophrenia among nursing home residents without dementia: systematic review and meta-analysis.Br J Psychiatry. 2020 Jan;216(1):6-15. doi: 10.1192/bjp.2019.5. Br J Psychiatry. 2020. PMID: 30864533
-
A cross-sectional survey to investigate the prevalence of pain in Japanese patients with major depressive disorder and schizophrenia.Compr Psychiatry. 2015 May;59:91-7. doi: 10.1016/j.comppsych.2015.02.004. Epub 2015 Feb 17. Compr Psychiatry. 2015. PMID: 25724075
-
Prevalence of comorbid substance use in major depressive disorder in community and clinical settings, 1990-2019: Systematic review and meta-analysis.J Affect Disord. 2020 Apr 1;266:288-304. doi: 10.1016/j.jad.2020.01.141. Epub 2020 Jan 26. J Affect Disord. 2020. PMID: 32056890
Cited by
-
Factors associated with death, hospitalization, resignation, and sick leave from work among patients with schizophrenia in Japan: a nested case-control study using a large claims database.BMC Psychiatry. 2024 Jan 3;24(1):22. doi: 10.1186/s12888-023-05474-5. BMC Psychiatry. 2024. PMID: 38172827 Free PMC article.
-
Glutamate Efflux across the Blood-Brain Barrier: New Perspectives on the Relationship between Depression and the Glutamatergic System.Metabolites. 2022 May 20;12(5):459. doi: 10.3390/metabo12050459. Metabolites. 2022. PMID: 35629963 Free PMC article. Review.
-
Prevalence of treatment-resistant depression and associated factors among major depressive disorder follow-up patients at Saint Amanuel Mental Specialised Hospital in Ethiopia: a cross-sectional study.BMJ Open. 2024 Nov 27;14(11):e087006. doi: 10.1136/bmjopen-2024-087006. BMJ Open. 2024. PMID: 39609013 Free PMC article.
-
Effects of COVID-19-related stress and fear on depression in schizophrenia patients and the general population.Schizophrenia (Heidelb). 2022 Mar 5;8(1):15. doi: 10.1038/s41537-022-00213-3. Schizophrenia (Heidelb). 2022. PMID: 35249110 Free PMC article.
-
Depression in healthcare workers: Results from the nationwide AMADEUS survey.Int J Nurs Stud. 2022 Nov;135:104328. doi: 10.1016/j.ijnurstu.2022.104328. Epub 2022 Jul 23. Int J Nurs Stud. 2022. PMID: 35952535 Free PMC article.
References
-
- Fond G, Lancon C, Auquier P, Boyer L. Prévalence de la dépression majeure en France en population générale et en populations spécifiques de 2000 à 2018 : une revue systématique de la littérature. Presse Médicale. 2019;48(4):365–375. - PubMed
-
- Johnson DA. Studies of depressive symptoms in schizophrenia. Br J Psychiatry. 1981;139:89–101. - PubMed
-
- Andrianarisoa M, Boyer L, Godin O, et al. ; FACE-SCZ Group . Childhood trauma, depression and negative symptoms are independently associated with impaired quality of life in schizophrenia. Results from the national FACE-SZ cohort. Schizophr Res. 2017;185:173–181. - PubMed
-
- Godin O, Leboyer M, Schürhoff F, et al. ; FACE-SZ (FondaMental Academic Centers of Expertise for Schizophrenia) Group . Predictors of rapid high weight gain in schizophrenia: longitudinal analysis of the French FACE-SZ cohort. J Psychiatr Res. 2017;94:62–69. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical