Circulating insulin-like growth factor-I, total and free testosterone concentrations and prostate cancer risk in 200 000 men in UK Biobank
- PMID: 33252839
- PMCID: PMC8048461
- DOI: 10.1002/ijc.33416
Circulating insulin-like growth factor-I, total and free testosterone concentrations and prostate cancer risk in 200 000 men in UK Biobank
Abstract
Insulin-like growth factor-I (IGF-I) and testosterone have been implicated in prostate cancer aetiology. Using data from a large prospective full-cohort with standardised assays and repeat blood measurements, and genetic data from an international consortium, we investigated the associations of circulating IGF-I, sex hormone-binding globulin (SHBG), and total and calculated free testosterone concentrations with prostate cancer incidence and mortality. For prospective analyses, risk was estimated using multivariable-adjusted Cox regression in 199 698 male UK Biobank participants. Hazard ratios (HRs) were corrected for regression dilution bias using repeat hormone measurements from a subsample. Two-sample Mendelian randomisation (MR) analysis of IGF-I and risk used genetic instruments identified from UK Biobank men and genetic outcome data from the PRACTICAL consortium (79 148 cases and 61 106 controls). We used cis- and all (cis and trans) SNP MR approaches. A total of 5402 men were diagnosed with and 295 died from prostate cancer (mean follow-up 6.9 years). Higher circulating IGF-I was associated with elevated prostate cancer diagnosis (HR per 5 nmol/L increment = 1.09, 95% CI 1.05-1.12) and mortality (HR per 5 nmol/L increment = 1.15, 1.02-1.29). MR analyses also supported the role of IGF-I in prostate cancer diagnosis (cis-MR odds ratio per 5 nmol/L increment = 1.34, 1.07-1.68). In observational analyses, higher free testosterone was associated with a higher risk of prostate cancer (HR per 50 pmol/L increment = 1.10, 1.05-1.15). Higher SHBG was associated with a lower risk (HR per 10 nmol/L increment = 0.95, 0.94-0.97), neither was associated with prostate cancer mortality. Total testosterone was not associated with prostate cancer. These findings implicate IGF-I and free testosterone in prostate cancer development and/or progression.
Keywords: IGF-I; Mendelian randomisation; prospective analysis; prostate cancer; testosterone.
© 2020 The Authors. International Journal of Cancer published by John Wiley & Sons Ltd on behalf of UICC.
Conflict of interest statement
Dr Holmes has collaborated with Boehringer Ingelheim in research, and in adherence to the University of Oxford's Clinical Trial Service Unit & Epidemiological Studies Unit (CSTU) staff policy, did not accept personal honoraria or other payments from pharmaceutical companies. All other authors have no competing interests to declare.
Figures
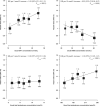




References
-
- Ferlay J, Ervik M, Lam F, et al. Global Cancer Observatory: Cancer Today. International Agency for Research on Cancer: Lyon, France; 2018.
-
- Pollak M. The insulin and insulin‐like growth factor receptor family in neoplasia: an update. Nat Rev Cancer. 2012;12:159‐169. - PubMed
-
- Morgentaler A, Traish AM. Shifting the paradigm of testosterone and prostate cancer: the saturation model and the limits of androgen‐dependent growth. Eur Urol. 2009;55:310‐320. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- 29017/CRUK_/Cancer Research UK/United Kingdom
- FS/18/23/33512/BHF_/British Heart Foundation/United Kingdom
- MC_UU_12013/3/MRC_/Medical Research Council/United Kingdom
- MC_QA137853/MRC_/Medical Research Council/United Kingdom
- DH_/Department of Health/United Kingdom
- MC_UU_00011/1/MRC_/Medical Research Council/United Kingdom
- C60192/A28516/CRUK_/Cancer Research UK/United Kingdom
- R01 CA128978/CA/NCI NIH HHS/United States
- LEAP 205212/Z/16/Z/WT_/Wellcome Trust/United Kingdom
- U19 CA148537/CA/NCI NIH HHS/United States
- C18281/A19169/CRUK_/Cancer Research UK/United Kingdom
- C8221/A20986/CRUK_/Cancer Research UK/United Kingdom
- U01 CA098233/CA/NCI NIH HHS/United States
- MC_PC_17228/MRC_/Medical Research Council/United Kingdom
- 28516/CRUK_/Cancer Research UK/United Kingdom
- U01 CA098710/CA/NCI NIH HHS/United States
- U01 CA188392/CA/NCI NIH HHS/United States
- C8221/A19170/CRUK_/Cancer Research UK/United Kingdom
- C8221/A29017/CRUK_/Cancer Research UK/United Kingdom
- U01 CA098216/CA/NCI NIH HHS/United States
- HHSN268201200008C/HL/NHLBI NIH HHS/United States
- MC_UU_12013/1/MRC_/Medical Research Council/United Kingdom
- U19 CA148112/CA/NCI NIH HHS/United States
- U01 CA098758/CA/NCI NIH HHS/United States
- MC_UU_12013/2/MRC_/Medical Research Council/United Kingdom
- U19 CA148065/CA/NCI NIH HHS/United States
- WT_/Wellcome Trust/United Kingdom
- HHSN268201200008I/HL/NHLBI NIH HHS/United States
- 001/WHO_/World Health Organization/International
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

