Impact of progressive resistance training on CT quantified muscle and adipose tissue compartments in pancreatic cancer patients
- PMID: 33253318
- PMCID: PMC7703876
- DOI: 10.1371/journal.pone.0242785
Impact of progressive resistance training on CT quantified muscle and adipose tissue compartments in pancreatic cancer patients
Abstract
Objectives: Loss of body weight is often seen in pancreatic cancer and also predicts poor prognosis. Thus, maintaining muscle mass is an essential treatment goal. The primary aim was to investigate whether progressive resistance training impacts muscle and adipose tissue compartments. Furthermore, the effect of body composition on overall survival (OS) was investigated.
Methods: In the randomized SUPPORT-study, 65 patients were assigned to 6-month resistance training (2x/week) or a usual care control group. As secondary endpoint, muscle strength of the upper and lower extremities was assessed before and after the intervention period. Routine CT scans were assessed on lumbar L3/4 level for quantification of total-fat-area, visceral-fat-area, subcutaneous-fat-area, intramuscular-fat-area, visceral-to-subcutaneous fat ratio (VFR), muscle-area (MA), muscle-density and skeletal-muscle-index (SMI). OS data were retrieved.
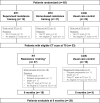
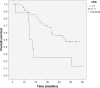
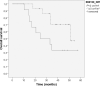
Results: Of 65 patients, 53 had suitable CT scans at baseline and 28 completed the intervention period with suitable CT scans. There were no significant effects observed of resistance training on body composition (p>0.05; effect sizes ω2p <0.02). Significant moderate to high correlations were found between MA and muscle strength parameters (r = 0.57-0.85; p<0.001). High VFR at baseline was a predictor of poor OS (VFR≥1.3 vs. <1.3; median OS 14.6 vs. 45.3 months; p = 0.012). Loss of muscle mass was also a predictor of poor OS (loss vs. gain of SMI; median OS 24.6 vs. 50.8 months; p = 0.049).
Conclusion: There is anabolic potential in patients with resectable pancreatic cancer. A progressive resistance training may help patients to maintain their muscle mass and avoid muscle depletion. CT-quantified muscle mass at the level of L3/4 showed a good correlation to muscle strength. Therefore, maintaining muscle mass and muscle strength through structured resistance training could help patients to maintain their physical functioning. A high VFR at baseline and a high loss of muscle mass are predictors of poor OS. Registered on ClinicalTrials.gov (NCT01977066).
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
References
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

