Ecthyma gangrenosum due to Pseudomonas aeruginosa sepsis as initial manifestation of X-linked agammaglobulinemia: a case report
- PMID: 33261572
- PMCID: PMC7704585
- DOI: 10.1186/s12887-020-02436-8
Ecthyma gangrenosum due to Pseudomonas aeruginosa sepsis as initial manifestation of X-linked agammaglobulinemia: a case report
Abstract
Background: X-linked agammaglobulinemia (XLA, OMIM#300,300), caused by mutations in the Bruton tyrosine kinase (BTK) gene, is a rare monogenic inheritable immunodeficiency disorder. Ecthyma gangrenosum is a cutaneous lesion caused by Pseudomonas aeruginosa that typically occurs in patients with XLA and other immunodeficiencies.
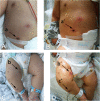
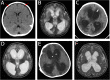
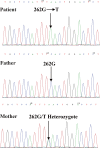
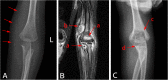
Case presentation: We report the case of a 20-month-old boy who presented with fever, vomiting, diarrhea, and ecthyma gangrenosum. Blood, stool, and skin lesion culture samples were positive for P. aeruginosa. A diagnosis of XLA was established, and the c.262G > T mutation in exon 4 of BTK was identified with Sanger sequencing. Symptoms improved following treatment with antibiotics and immunoglobulin infusion.
Conclusions: Primary immunodeficiency (i.e., XLA) should be suspected in male infants with P. aeruginosa sepsis, highlighting the importance of genetic and immune testing in these patients.
Keywords: Ecthyma gangrenosum; Pseudomonas aeruginosa; X-linked agammaglobulinemia; male infants.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- Lackey AE, Ahmad F. In: X-linked Agammaglobulinemia. StatPearls, editor. Treasure Island: StatPearls Publishing, StatPearls Publishing LLC.; 2020. - PubMed
Publication types
MeSH terms
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical

