Clinical Characteristics and Outcomes in Patients with COVID-19 and Cancer: a Systematic Review and Meta-analysis
- PMID: 33261978
- PMCID: PMC7674130
- DOI: 10.1016/j.clon.2020.11.006
Clinical Characteristics and Outcomes in Patients with COVID-19 and Cancer: a Systematic Review and Meta-analysis
Abstract
Much of routine cancer care has been disrupted due to the perceived susceptibility to SARS-CoV-2 infection in cancer patients. Here, we systematically review the current evidence base pertaining to the prevalence, presentation and outcome of COVID-19 in cancer patients, in order to inform policy and practice going forwards. A keyword-structured systematic search was conducted on Pubmed, Cochrane, Embase and MedRxiv databases for studies reporting primary data on COVID-19 in cancer patients. Studies were critically appraised using the NIH National Heart, Lung and Blood Institute's quality assessment tool set. The pooled prevalence of cancer as a co-morbidity in patients with COVID-19 and pooled in-hospital mortality risk of COVID-19 in cancer patients were derived by random-effects meta-analyses. In total, 110 studies from 10 countries were included. The pooled prevalence of cancer as a co-morbidity in hospitalised patients with COVID-19 was 2.6% (95% confidence interval 1.8%, 3.5%, I2: 92.0%). Specifically, 1.7% (95% confidence interval 1.3%, 2.3%, I2: 57.6.%) in China and 5.6% (95% confidence interval 4.5%, 6.7%, I2: 82.3%) in Western countries. Patients most commonly presented with non-specific symptoms of fever, dyspnoea and chest tightness in addition to decreased arterial oxygen saturation, ground glass opacities on computer tomography and non-specific changes in inflammatory markers. The pooled in-hospital mortality risk among patients with COVID-19 and cancer was 14.1% (95% confidence interval 9.1%, 19.8%, I2: 52.3%). We identified impeding questions that need to be answered to provide the foundation for an iterative review of the developing evidence base, and inform policy and practice going forwards. Analyses of the available data corroborate an unfavourable outcome of hospitalised patients with COVID-19 and cancer. Our findings encourage future studies to report detailed social, demographic and clinical characteristics of cancer patients, including performance status, primary cancer type and stage, as well as a history of anti-cancer therapeutic interventions.
Keywords: COVID-19; Cancer; SARS-CoV-2; mortality; prevalence; systematic review.
Copyright © 2020 The Royal College of Radiologists. Published by Elsevier Ltd. All rights reserved.
Figures
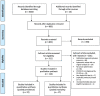



References
-
- Jordan R.E., Adab P., Cheng K.K. Covid-19: risk factors for severe disease and death. BMJ. 2020;368:m1198. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

