Intra-articular vs. intravenous administration: a meta-analysis of tranexamic acid in primary total knee arthroplasty
- PMID: 33267906
- PMCID: PMC7709322
- DOI: 10.1186/s13018-020-02119-1
Intra-articular vs. intravenous administration: a meta-analysis of tranexamic acid in primary total knee arthroplasty
Abstract
Background: The optimal dosage and administration approach of tranexamic acid (TXA) in primary total knee arthroplasty (TKA) remains controversial. In light of recently published 14 randomized controlled trials (RCTs), the study aims to incorporate the newly found evidence and compare the efficacy and safety of intra-articular (IA) vs. intravenous (IV) application of TXA in primary TKA.
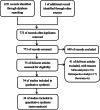
Methods: PubMed, Embase, Web of Science, and Cochrane Library were searched for RCTs comparing IA with IV TXA for primary TKA. Primary outcomes included total blood loss (TBL) and drain output. Secondary outcomes included hidden blood loss (HBL), hemoglobin (Hb) fall, blood transfusion rate, perioperative complications, length of hospital stay, and tourniquet time.
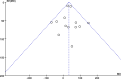
Result: In all, 34 RCTs involving 3867 patients were included in our meta-analysis. Significant advantages of IA were shown on TBL (MD = 33.38, 95% CI = 19.24 to 47.51, P < 0.001), drain output (MD = 28.44, 95% CI = 2.61 to 54.27, P = 0.03), and postoperative day (POD) 3+ Hb fall (MD = 0.24, 95% CI = 0.09 to 0.39, P = 0.001) compared with IV. There existed no significant difference on HBL, POD1 and POD2 Hb fall, blood transfusion rate, perioperative complications, length of hospital stay, and tourniquet time between IA and IV.
Conclusion: Intra-articular administration of TXA is superior to intravenous in primary TKA patients regarding the performance on TBL, drain output, and POD3+ Hb fall, without increased risk of perioperative complications. Therefore, intra-articular administration is the recommended approach in clinical practice for primary TKA.
Keywords: Intra-articular administration; Intravenous administration; Total knee arthroplasty; Tranexamic acid.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- Fillingham YA, Ramkumar DB, Jevsevar DS, et al. Tranexamic acid use in total joint arthroplasty: the clinical practice guidelines endorsed by the American Association of Hip and Knee Surgeons, American Society of Regional Anesthesia and Pain Medicine, American Academy of Orthopaedic Surgeons, Hip Society, and Knee Society. J Arthroplasty. 2018;33(10):3065–3069. doi: 10.1016/j.arth.2018.08.002. - DOI - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials