Residual, differential neurobehavioral deficits linger after multiple recovery nights following chronic sleep restriction or acute total sleep deprivation
- PMID: 33274389
- PMCID: PMC8274462
- DOI: 10.1093/sleep/zsaa224
Residual, differential neurobehavioral deficits linger after multiple recovery nights following chronic sleep restriction or acute total sleep deprivation
Abstract
Study objectives: The amount of recovery sleep needed to fully restore well-established neurobehavioral deficits from sleep loss remains unknown, as does whether the recovery pattern differs across measures after total sleep deprivation (TSD) and chronic sleep restriction (SR).
Methods: In total, 83 adults received two baseline nights (10-12-hour time in bed [TIB]) followed by five 4-hour TIB SR nights or 36-hour TSD and four recovery nights (R1-R4; 12-hour TIB). Neurobehavioral tests were completed every 2 hours during wakefulness and a Maintenance of Wakefulness Test measured physiological sleepiness. Polysomnography was collected on B2, R1, and R4 nights.
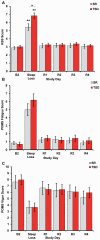
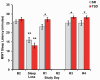
Results: TSD and SR produced significant deficits in cognitive performance, increases in self-reported sleepiness and fatigue, decreases in vigor, and increases in physiological sleepiness. Neurobehavioral recovery from SR occurred after R1 and was maintained for all measures except Psychomotor Vigilance Test (PVT) lapses and response speed, which failed to completely recover. Neurobehavioral recovery from TSD occurred after R1 and was maintained for all cognitive and self-reported measures, except for vigor. After TSD and SR, R1 recovery sleep was longer and of higher efficiency and better quality than R4 recovery sleep.
Conclusions: PVT impairments from SR failed to reverse completely; by contrast, vigor did not recover after TSD; all other deficits were reversed after sleep loss. These results suggest that TSD and SR induce sustained, differential biological, physiological, and/or neural changes, which remarkably are not reversed with chronic, long-duration recovery sleep. Our findings have critical implications for the population at large and for military and health professionals.
Keywords: MWT; chronic sleep restriction; cognitive; fatigue; psychomotor vigilance test; recovery; sleepiness; total sleep deprivation; vigor.
© Sleep Research Society 2020. Published by Oxford University Press on behalf of the Sleep Research Society. All rights reserved. For permissions, please e-mail journals.permissions@oup.com.
Figures

References
-
- National Sleep Foundation. 2005 Sleep in America Poll – adult sleep habits and styles. Sleep Health. 2015;1(2):e4.
-
- Bonnet MH, et al. . We are chronically sleep deprived. Sleep. 1995;18(10):908–911. - PubMed
-
- Balkin TJ, et al. . Sleep loss and sleepiness: current issues. Chest. 2008;134(3):653–660. - PubMed
-
- Tartar JL, et al. . Sleep restriction and delayed sleep associate with psychological health and biomarkers of stress and inflammation in women. Sleep Health. 2015;1(4):249–256. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Research Materials

