Fatigue and brain arousal in patients with major depressive disorder
- PMID: 33275166
- PMCID: PMC7981331
- DOI: 10.1007/s00406-020-01216-w
Fatigue and brain arousal in patients with major depressive disorder
Abstract
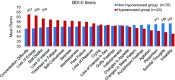
Fatigue is considered a key symptom of major depressive disorder (MDD), yet the term lacks specificity. It can denote a state of increased sleepiness and lack of drive (i.e., downregulated arousal) as well as a state of high inner tension and inhibition of drive with long sleep onset latencies (i.e., upregulated arousal), the latter typically found in depression. It has been proposed to differentiate fatigue along the dimension of brain arousal. We investigated whether such stratification within a group of MDD patients would reveal a subgroup with distinct clinical features. Using an automatic classification of EEG vigilance stages, an arousal stability score was calculated for 15-min resting EEGs of 102 MDD patients with fatigue. 23.5% of the patients showed signs of hypoarousal with EEG patterns indicating drowsiness or sleep; this hypoaroused subgroup was compared with remaining patients (non-hypoaroused subgroup) concerning self-rated measures of depressive symptoms, sleepiness, and sleep. The hypoaroused subgroup scored higher on the Beck Depression Inventory items "loss of energy" (Z = - 2.13, p = 0.033; ɳ2 = 0.044, 90% CI 0.003-0.128) and "concentration difficulty" (Z = - 2.40, p = 0.017; ɳ2 = 0.056, 90% CI 0.009-0.139), and reported higher trait and state sleepiness (p < 0.05) as compared to the non-hypoaroused group. The non-hypoaroused subgroup, in contrast, reported more frequently the presence of suicidal ideation (Chi2 = 3.81, p = 0.051; ɳ2 = 0.037, 90% CI 0.0008-0.126). In this study, we found some evidence that stratifying fatigued MDD patients by arousal may lead to subgroups that are pathophysiologically and clinically more homogeneous. Brain arousal may be a worth while target in clinical research for better understanding the mechanisms underlying suicidal tendencies and to improve treatment response.
Keywords: Brain arousal regulation; Depression; EEG; Fatigue; Neurophysiology.
Conflict of interest statement
UH was an advisory board member for Lilly, Lundbeck, Servier, Takeda and Otsuka; a consultant for Bayer and Nycomed; and a speaker for Bristol-Myers Squibb, Medice Arzneimittel, Novartis, and Roche. CU, GS, FMS, CS, TH declare no conflict of interest.
Figures

References
-
- World Health Organisation, WHO (2018) Fact sheet No 369: Depression. Available at: http://www.who.int/mediacentre/factsheets/fs369/en/. Accessed 1 May 2020
-
- Hegerl U. Largely unnoticed flaws in the fundamentals of depression diagnosis: The semantics of core symptoms. Aust N Z J Psychiatry. 2014;48(12):1166–1166. - PubMed
-
- Ghanean H, Ceniti AK, Kennedy SH. Fatigue in patients with major depressive disorder: prevalence, burden and pharmacological approaches to management. CNS Drugs. 2018;32(1):65–74. - PubMed
-
- Morris G, Berk M, Galecki P, et al. The neuro-immune pathophysiology of central and peripheral fatigue in systemic immune-inflammatory and neuro-immune diseases. Mol Neurobiol. 2016;53:1195–1219. - PubMed
-
- Hegerl U, Lam RW, Malhi GS, et al. Conceptualising the neurobiology of fatigue. Aust N Z J Psychiatry. 2013;47:312–316. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

