Mechanisms of Hypoxia in COVID-19 Patients: A Pathophysiologic Reflection
- PMID: 33281323
- PMCID: PMC7689135
- DOI: 10.5005/jp-journals-10071-23547
Mechanisms of Hypoxia in COVID-19 Patients: A Pathophysiologic Reflection
Abstract
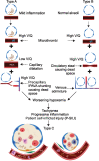
Coronavirus disease-2019 (COVID-19) causes severe hypoxemia which fulfills the criteria of acute respiratory distress syndrome (ARDS) but is not accompanied by typical features of the syndrome. The combination of factors including low P/F ratios, high A-a gradient, relatively preserved lung mechanics, and normal pulmonary pressures may imply a process occurring on the vascular side of the alveolar-capillary unit. The scant but rapidly evolving data available on the pathophysiology are seemingly conflicting, indicating the relative dominance of intrapulmonary shunting or dead space in different studies. In this hypothesis paper, we attempt to gather and explain these observations within a unified conceptual framework by invoking the relative contributions of microvascular thrombosis, along with two proposed vascular mechanisms of capillary flow redistribution and flow through intrapulmonary arteriovenous anastomoses (IPAVA). How to cite this article: Nitsure M, Sarangi B, Shankar GH, Reddy VS, Walimbe A, Sharma V, et al. Mechanisms of Hypoxia in COVID-19 Patients: A Pathophysiologic Reflection. Indian J Crit Care Med 2020;24(10):967-970.
Keywords: Acute respiratory distress syndrome; COVID-19; Hypoxemia; Intrapulmonary arteriovenous anastomoses.
Copyright © 2020; Jaypee Brothers Medical Publishers (P) Ltd.
Conflict of interest statement
Source of support: Nil Conflict of interest: None
Figures
References
-
- Mauri T, Spinelli E, Scotti E, Colussi G, Basile MC, Crotti S, et al. Potential for lung recruitment and ventilation-perfusion mismatch in patients with the acute respiratory distress syndrome from coronavirus disease 2019. Crit Care Med. 2020 doi: 10.1097/CCM.0000000000004386. DOI: - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources