Understanding equity of institutional delivery in public health centre by level of care in India: an assessment using benefit incidence analysis
- PMID: 33298077
- PMCID: PMC7724812
- DOI: 10.1186/s12939-020-01331-z
Understanding equity of institutional delivery in public health centre by level of care in India: an assessment using benefit incidence analysis
Abstract
Background: The National Health Mission (NHM), the largest ever publicly funded health programme worldwide, used over half of the national health budget in India and primarily aimed to improve maternal and child health in the country. Though large scale public health investment has improved the health care utilization and health outcomes across states and socio-economic groups in India, little is known on the equity concern of NHM. In this context, this paper examines the utilization pattern and net benefit of public subsidy for institutional delivery by the level of care in India.
Methods: Data from the most recent round of the National Family Health Survey (NFHS 4), conducted during 2015-16, was used in the study. A total of 148,645 last birth delivered in a health centre during the 5 years preceding the survey were used for the analyses. Out-of-pocket (OOP) payment on delivery care was taken as the dependent variable and was analysed by primary care and secondary level of care. Benefits Incidence Analysis (BIA), descriptive statistics, concentration index (CI), and concentration curve (CC) were used to do the analysis.
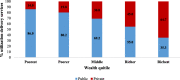
Results: Institutional delivery from the public health centres in India is pro-poor and has a strong economic gradient. However, about 28% mothers from richest wealth quintile did not pay for delivery in public health centres compared to 16% among the poorest wealth quintile. Benefit incidence analyses suggests a pro-poor distribution of institutional delivery both at primary and secondary level of care. In 2015-16, at the primary level, about 32.29% of subsidies were used by the poorest, 27.22% by poorer, 20.39% by middle, 13.36% by richer and 6.73% by the richest wealth quintile. The pattern at the secondary level was similar, though the magnitude was lower. The concentration index of institutional delivery in public health centres was - 0.161 [95% CI, - 0.158, - 0.165] compared to 0.296 [95% CI, 0.289, 0.303] from private health centres.
Conclusion: Provision and use of public subsidy for institutional delivery in public health centres is pro-poor in India. Improving the quality of service in primary health centres is recommended to increase utilisation and reduce OOP payment for health care in India.
Keywords: Benefit incidence; Delivery care; Equity; India; National Health Mission.
Conflict of interest statement
The authors declare that they do not have any competing interest.
Figures

References
-
- WHO. Global Spending on Health: A World in Transition 2019. Glob Rep. 2019;49 Available from: https://www.who.int/health_financing/documents/health-expenditure-report....
-
- WHO . Public spending on health: a closer look at global trends. 2018.
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

