Antenatal interventions for preventing stillbirth, fetal loss and perinatal death: an overview of Cochrane systematic reviews
- PMID: 33336827
- PMCID: PMC8078228
- DOI: 10.1002/14651858.CD009599.pub2
Antenatal interventions for preventing stillbirth, fetal loss and perinatal death: an overview of Cochrane systematic reviews
Abstract
Background: Stillbirth is generally defined as a death prior to birth at or after 22 weeks' gestation. It remains a major public health concern globally. Antenatal interventions may reduce stillbirths and improve maternal and neonatal outcomes in settings with high rates of stillbirth. There are several key antenatal strategies that aim to prevent stillbirth including nutrition, and prevention and management of infections.
Objectives: To summarise the evidence from Cochrane systematic reviews on the effects of antenatal interventions for preventing stillbirth for low risk or unselected populations of women.
Methods: We collaborated with Cochrane Pregnancy and Childbirth's Information Specialist to identify all their published reviews that specified or reported stillbirth; and we searched the Cochrane Database of Systematic Reviews (search date: 29 Feburary 2020) to identify reviews published within other Cochrane groups. The primary outcome measure was stillbirth but in the absence of stillbirth data, we used perinatal mortality (both stillbirth and death in the first week of life), fetal loss or fetal death as outcomes. Two review authors independently evaluated reviews for inclusion, extracted data and assessed quality of evidence using AMSTAR (A Measurement Tool to Assess Reviews) and GRADE tools. We assigned interventions to categories with graphic icons to classify the effectiveness of interventions as: clear evidence of benefit or harm; clear evidence of no effect or equivalence; possible benefit or harm; or unknown benefit or harm or no effect or equivalence.
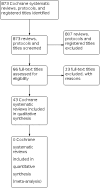
Main results: We identified 43 Cochrane Reviews that included interventions in pregnant women with the potential for preventing stillbirth; all of the included reviews reported our primary outcome 'stillbirth' or in the absence of stillbirth, 'perinatal death' or 'fetal loss/fetal death'. AMSTAR quality was high in 40 reviews with scores ranging from 8 to 11 and moderate in three reviews with a score of 7. Nutrition interventions Clear evidence of benefit: balanced energy/protein supplementation versus no supplementation suggests a probable reduction in stillbirth (risk ratio (RR) 0.60, 95% confidence interval (CI) 0.39 to 0.94, 5 randomised controlled trials (RCTs), 3408 women; moderate-certainty evidence). Clear evidence of no effect or equivalence for stillbirth or perinatal death: vitamin A alone versus placebo or no treatment; and multiple micronutrients with iron and folic acid versus iron with or without folic acid. Unknown benefit or harm or no effect or equivalence: for all other nutrition interventions examined the effects were uncertain. Prevention and management of infections Possible benefit for fetal loss or death: insecticide-treated anti-malarial nets versus no nets (RR 0.67, 95% CI 0.47 to 0.97, 4 RCTs; low-certainty). Unknown evidence of no effect or equivalence: drugs for preventing malaria (stillbirth RR 1.02, 95% CI 0.76 to 1.36, 5 RCTs, 7130 women, moderate certainty in women of all parity; perinatal death RR 1.24, 95% CI 0.94 to 1.63, 4 RCTs, 5216 women, moderate-certainty in women of all parity). Prevention, detection and management of other morbidities Clear evidence of benefit: the following interventions suggest a reduction: midwife-led models of care in settings where the midwife is the primary healthcare provider particularly for low-risk pregnant women (overall fetal loss/neonatal death reduction RR 0.84, 95% CI 0.71 to 0.99, 13 RCTs, 17,561 women; high-certainty), training versus not training traditional birth attendants in rural populations of low- and middle-income countries (stillbirth reduction odds ratio (OR) 0.69, 95% CI 0.57 to 0.83, 1 RCT, 18,699 women, moderate-certainty; perinatal death reduction OR 0.70, 95% CI 0.59 to 0.83, 1 RCT, 18,699 women, moderate-certainty). Clear evidence of harm: a reduced number of antenatal care visits probably results in an increase in perinatal death (RR 1.14 95% CI 1.00 to 1.31, 5 RCTs, 56,431 women; moderate-certainty evidence). Clear evidence of no effect or equivalence: there was evidence of no effect in the risk of stillbirth/fetal loss or perinatal death for the following interventions and comparisons: psychosocial interventions; and providing case notes to women. Possible benefit: community-based intervention packages (including community support groups/women's groups, community mobilisation and home visitation, or training traditional birth attendants who made home visits) may result in a reduction of stillbirth (RR 0.81, 95% CI 0.73 to 0.91, 15 RCTs, 201,181 women; low-certainty) and perinatal death (RR 0.78, 95% CI 0.70 to 0.86, 17 RCTs, 282,327 women; low-certainty). Unknown benefit or harm or no effect or equivalence: the effects were uncertain for other interventions examined. Screening and management of fetal growth and well-being Clear evidence of benefit: computerised antenatal cardiotocography for assessing infant's well-being in utero compared with traditional antenatal cardiotocography (perinatal mortality reduction RR 0.20, 95% CI 0.04 to 0.88, 2 RCTs, 469 women; moderate-certainty). Unknown benefit or harm or no effect or equivalence: the effects were uncertain for other interventions examined.
Authors' conclusions: While most interventions were unable to demonstrate a clear effect in reducing stillbirth or perinatal death, several interventions suggested a clear benefit, such as balanced energy/protein supplements, midwife-led models of care, training versus not training traditional birth attendants, and antenatal cardiotocography. Possible benefits were also observed for insecticide-treated anti-malarial nets and community-based intervention packages, whereas a reduced number of antenatal care visits were shown to be harmful. However, there was variation in the effectiveness of interventions across different settings, indicating the need to carefully understand the context in which these interventions were tested. Further high-quality RCTs are needed to evaluate the effects of antenatal preventive interventions and which approaches are most effective to reduce the risk of stillbirth. Stillbirth (or fetal death), perinatal and neonatal death need to be reported separately in future RCTs of antenatal interventions to allow assessment of different interventions on these rare but important outcomes and they need to clearly define the target populations of women where the intervention is most likely to be of benefit. As the high burden of stillbirths occurs in low- and middle-income countries, further high-quality trials need to be conducted in these settings as a priority.
Copyright © 2020 The Cochrane Collaboration. Published by John Wiley & Sons, Ltd.
Conflict of interest statement
Erika Ota: author of 'Vitamin supplementation for preventing miscarriage', 'Antenatal dietary education and supplementation to increase energy and protein intake', 'Zinc supplementation for improving pregnancy and infant outcome', 'Vitamin E supplementation in pregnancy', 'Vitamin C supplementation in pregnancy', and 'Iodine supplementation for women during the preconception pregnancy and postpartum period'.
Katharina da Silva Lopes: author of 'Vitamin supplementation for preventing miscarriage'.
Md. Obaidur Rahman: none known.
Philippa Middleton: author of 'Omega‐3 fatty acid addition during pregnancy' and 'Zinc supplementation for improving pregnancy and infant outcome'.
Vicki Flenady: I have a Career Development Fellowship grant for my salary from the National Health and Medical Research Council Australia.
Windy MV Wariki: none known.
Ruoyan Tobe‐Gai: author of 'Antenatal dietary education and supplementation to increase energy and protein intake', and 'Zinc supplementation for improving pregnancy and infant outcome'.
Rintaro Mori: author of 'Giving women their own case notes to carry during pregnancy.', 'Vitamin supplementation for preventing miscarriage', 'Antenatal dietary education and supplementation to increase energy and protein intake', and 'Zinc supplementation for improving pregnancy and infant outcome'
Figures





Update of
References
References to included reviews
Alfirevic 2015
Balogun 2016
Bricker 2015
Brown 2015
Buppasiri 2015
-
- Buppasiri P, Lumbiganon P, Thinkhamrop J, Ngamjarus C, Laopaiboon M, Medley N. Calcium supplementation (other than for preventing or treating hypertension) for improving pregnancy and infant outcomes. Cochrane Database of Systematic Reviews 2015, Issue 2. Art. No: CD007079. [DOI: 10.1002/14651858.CD007079.pub3] - DOI - PMC - PubMed
Catling 2015
Chamberlain 2017
Churchill 2007
Coleman 2015
Das 2018
-
- Das JK, Hoodbhoy Z, Salam RA, Bhutta AZ, Valenzuela-Rubio NG, Weise Prinzo Z, et al. Lipid-based nutrient supplements for maternal, birth, and infant developmental outcomes. Cochrane Database of Systematic Reviews 2018, Issue 8. Art. No: CD012610. [DOI: 10.1002/14651858.CD012610.pub2] - DOI - PMC - PubMed
De‐Regil 2015
Dowswell 2015
Duley 2005
Gamble 2006
Grivell 2015
Harding 2017
Heazell 2015
Hofmeyr 2018
Hofmeyr 2019
Iheozor‐Ejiofor 2017
Keats 2019
Lassi 2015
Makrides 2014
Mangesi 2015
McCauley 2015
Meher 2006
Meher 2007
Middleton 2018
Ota 2015a
Ota 2015b
Palacios 2019
Radeva‐Petrova 2014
-
- Radeva-Petrova D, Kayentao K, ter Kuile FO, Sinclair D, Garner P. Drugs for preventing malaria in pregnant women in endemic areas: any drug regimen versus placebo or no treatment. Cochrane Database of Systematic Reviews 2014, Issue 10. Art. No: CD000169. [DOI: 10.1002/14651858.CD000169.pub3] - DOI - PMC - PubMed
Robert Peter 2015
Rumbold 2008
Rumbold 2015a
Rumbold 2015b
Sandall 2016
Shepherd 2017
Sibley 2012
Spencer 2015
-
- Spencer L, Bubner T, Bain E, Middleton P. Screening and subsequent management for thyroid dysfunction pre-pregnancy and during pregnancy for improving maternal and infant health. Cochrane Database of Systematic Reviews 2015, Issue 9. Art. No: CD011263. [DOI: 10.1002/14651858.CD011263.pub2] - DOI - PMC - PubMed
Stampalija 2010
Tieu 2017
-
- Tieu J, McPhee AJ, Crowther CA, Middleton P, Shepherd E. Screening for gestational diabetes mellitus based on different risk profiles and settings for improving maternal and infant health. Cochrane Database of Systematic Reviews 2017, Issue 8. Art. No: CD007222. [DOI: 10.1002/14651858.CD007222.pub4] - DOI - PMC - PubMed
References to excluded reviews
Alexander 2010
Balogun 2016
Bergel 2002
Crowther 2010
Demicheli 2015
East 2019
Gagnon 2007
Jahanfar 2015
Kramer 2006
Lagarde 2009
McBain 2015
Meher 2006a
Muktabhant 2015
Nabhan 2008
Nabhan 2015
Pattinson 2005
Peña‐Rosas 2015a
Peña‐Rosas 2015b
Salam 2015
Sangkomkamhang 2015
-
- Sangkomkamhang US, Lumbiganon P, Prasertcharoensuk W, Laopaiboon M. Antenatal lower genital tract infection screening and treatment programs for preventing preterm delivery. Cochrane Database of Systematic Reviews 2015, Issue 2. Art. No: CD006178. [DOI: 10.1002/14651858.CD006178.pub3] - DOI - PMC - PubMed
Stade 2009
-
- Stade BC, Bailey C, Dzendoletas D, Sgro M, Dowswell T, Bennett D. Psychological and/or educational interventions for reducing alcohol consumption in pregnant women and women planning pregnancy. Cochrane Database of Systematic Reviews 2009, Issue 2. Art. No: CD004228. [DOI: 10.1002/14651858.CD004228.pub2] - DOI - PMC - PubMed
Van Lonkhuijzen 2012
Additional references
Abu‐Saad 2010
-
- Abu-Saad K, Fraser D. Maternal nutrition and birth outcomes. Epidemiologic Reviews 2010;32(1):5-25. - PubMed
Ananth 2010
Bhutta 2011
-
- Bhutta ZA, Yakoob MY, Lawn JE, Rizvi A, Friberg IK, Weissman E, et al. Stillbirths: what difference can we make and at what cost? Lancet 2011;377(9776):1523-38. - PubMed
Blencowe 2010
Blencowe 2016
-
- Blencowe H, Cousens S, Jassir FB, Say L, Chou D, Mathers C, et al. National, regional, and worldwide estimates of stillbirth rates in 2015, with trends from 2000: a systematic analysis. Lancet Global Health 2016;4(2):e98-e108. - PubMed
Challis 2002
-
- Challis K, Osman NB, Nystrom L, Nordahl G, Bergstrom S. Symphysis-fundal height growth chart of an obstetric cohort of 817 Mozambican women with ultrasound-dated singleton pregnancies. Tropical Medicine and International Health 2002;7(8):678-84. - PubMed
Chein 1996
-
- Chein PF, Khan KS, Arnott N. Magnesium sulphate is the treatment of eclampsia and pre-eclampsia: an overview of the evidence from randomized trials. British Journal of Obstetrics and Gynaecology 1996;103:1085-91. - PubMed
Cousens 2011
-
- Cousens S, Blencowe H, Stanton C, Chou D, Ahmed S, Steinhardt L, et al. National, regional, and worldwide estimates of stillbirth rates in 2009 with trends since 1995: a systematic analysis. Lancet 2011;377(9774):1319-30. - PubMed
Crawford 2008
-
- Crawford JT, Tolosa JE, Goldenberg RL. Smoking cessation in pregnancy: why, how, and what next. Clinical Obstetrics and Gynecology 2008;51(2):419-35. - PubMed
De Onis 1998
-
- De Onis M, Villar J, Gulmezoglu M. Nutritional interventions to prevent intrauterine growth retardation: evidence from randomized controlled trials. European Journal of Clinical Nutrition 1998;52 Suppl 1:S83-S93. - PubMed
Di Mario 2007
-
- Di Mario S, Say L, Lincetto O. Risk factors for stillbirth in developing countries: a systematic review of the literature. Sexually Transmitted Diseases 2007;34(7 Suppl):S11-S21. - PubMed
Flenady 2011
-
- Flenady V, Koopmans L, Middleton P, Frøen JF, Smith GC, Gibbons K, et al. Major risk factors for stillbirth in high-income countries: a systematic review and meta-analysis. Lancet 2011;377(9774):1331-40. - PubMed
Flenady 2016
-
- Flenady V, Wojcieszek AM, Middleton P, Ellwood D, Erwich JJ, Coory M, et al. Stillbirths: recall to action in high-income countries. Lancet 2016;387(10019):691-702. - PubMed
Froen 2011
-
- Froen JF, Cacciatore J, McClure EM, Kuti O, Jokhio AH, Islam M, et al. Stillbirths: why they matter. Lancet 2011;377(9774):1353-66. - PubMed
Galal 2012
Goldenberg 2003
-
- Goldenberg RL, Thompson C. The infectious origins of stillbirth. American Journal of Obstetrics and Gynecology 2003;189(3):861-73. - PubMed
Goldenberg 2011
-
- Goldenberg RL, McClure EM, Bhutta ZA, Belizán JM, Reddy UM, Rubens CE, et al, Lancet's Stillbirths Series steering committee. Stillbirths: the vision for 2020. Lancet 2011;377(9779):1798-805. - PubMed
Hammoud 2005
-
- Hammoud AO, Bujold E, Sorokin Y, Schild C, Krapp M, Baumann P. Smoking in pregnancy revisited: findings from a large population-based study. American Journal of Obstetrics and Gynecology 2005;192:1856-63. - PubMed
Haws 2009
Heazell 2016
-
- Heazell AE, Siassakos D, Blencowe H, Burden C, Bhutta ZA, Cacciatore J, et al. Stillbirths: economic and psychosocial consequences. Lancet 2016;387(10018):604-16. [PMID: ] - PubMed
Higgins 2011a
Higgins 2011b
-
- Higgins JP, Altman DG, Sterne JA (editors). Chapter 8: Assessing risk of bias in included studies. In: Higgins JP, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 (updated March 2011). The Cochrane Collaboration, 2011. Available from training.cochrane.org/handbook/archive/v5.1/.
Hoffman 2009
-
- Hoffman C, Galan HL. Assessing the 'at-risk' fetus: Doppler ultrasound. Current Opinion in Obstetrics and Gynecology 2009;21(2):161-6. - PubMed
Hussain 2011
Imdad 2011
Jabeen 2011
Jang 2018
-
- Jang W, Kim H, Lee BE, Chang N. Maternal fruit and vegetable or vitamin C consumption during pregnancy is associated with fetal growth and infant growth up to 6 months: results from the Korean Mothers and Children’s Environmental Health (MOCEH) cohort study. Nutrition Journal 2018;17(1):105. - PMC - PubMed
Lawn 2011
-
- Lawn JE, Blencowe H, Pattinson R, Cousens S, Kumar R, Ibiebele I, et al. Stillbirths: where? When? Why? How to make the data count? Lancet 2011;377(9775):1448-63. - PubMed
Lawn 2016
-
- Lawn JE, Blencowe H, Waiswa P, Amouzou A, Mathers C, Hogan D, et al. Stillbirths: rates, risk factors, and acceleration towards 2030. Lancet 2016;387(10018):587-603. - PubMed
McClure 2007
-
- McClure EM, Goldenberg RL, Bann CM. Maternal mortality, stillbirth and measures of obstetric care in developing and developed countries. International Journal of Gynecology & Obstetrics 2007;96(2):139-46. - PubMed
McClure 2009
Medley 2018
Menzies 2007
-
- Menzies J, Magee LA, Li J, MacNab YC, Yin R, Stuart H, et al. Instituting surveillance guidelines and adverse outcomes in preeclampsia. Obstetrics & Gynecology 2007;110(1):121-7. - PubMed
Moher 2007
Norwitz 2007
-
- Norwitz ER, Snegovskikh VV, Caughey AB. Prolonged pregnancy: when should we intervene? Clinical Obstetrics and Gynecology 2007;50(2):547-57. - PubMed
Pattinson 2011
-
- Pattinson R, Kerber K, Buchmann E, Friberg IK, Belizan M, Lansky S, et al, for The Lancet's Stillbirths Series steering committee. Stillbirths: how can health systems deliver for mothers and babies? Lancet 2011;377(9777):1610-23. - PubMed
Perez‐Lopez 2015
-
- Perez-Lopez FR, Pasupuleti V, Mezones-Holguin E, Benites-Zapata VA, Thota P, Deshpande A, et al. Effect of vitamin D supplementation during pregnancy on maternal and neonatal outcomes: a systematic review and meta-analysis of randomized controlled trials. Fertility and Sterility 2015;103(5):1278-88.e4. [PMID: ] - PubMed
Pollock 2019
-
- Pollock M, Fernandes RM, Becker LA, Pieper D, Hartling L. Chapter V: Overviews of reviews. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, et al., editors. Cochrane Handbook for Systematic Reviews of Interventions version 6.0 (updated July 2019). The Cochrane Collaboration,. Available from https://www.training.cochrane.org/handbook.
Rosenstein 2012
Rumbold 2006
-
- Rumbold AR, Crowther CA, Haslam RR, Dekker GA, Robinson JS, for the ACTSSG. Vitamins C and E and the risks of preeclampsia and perinatal complications. New England Journal of Medicine 2006;354:1796-806. - PubMed
Salihu 2007
-
- Salihu HM, Wilson RE. Epidemiology of prenatal smoking and perinatal outcomes. Early Human Development 2007;83(11):713-20. - PubMed
Sanchez‐Ramos 2003
-
- Sanchez-Ramos L, Olivier F, Delke I, Kaunitz AM. Labor induction versus expectant management for postterm pregnancies: a systematic review with meta-analysis. Obstetrics & Gynecology 2003;101(6):1312-8. - PubMed
Schmid 2007
-
- Schmid GP, Stoner BP, Hawkes S, Broutet N. The need and plan for global elimination of congenital syphilis. Sexually Transmitted Diseases 2007;34(7 Suppl):S5-S10. - PubMed
Schünemann 2013
-
- Schünemann H, Brożek J, Guyatt G, Oxman A, editor(s). Handbook for grading the quality of evidence and the strength of recommendations using the GRADE approach (updated October 2013). GRADE Working Group, 2013. Available from gdt.guidelinedevelopment.org/app/handbook/handbook.html 2013.
Shea 2007
Shrimpton 2009
-
- Shrimpton R, Huffman SL, Zehner ER, Darnton-Hill I, Dalmiya N. Multiple micronutrient supplementation during pregnancy in developing-country settings: policy and program implications of the results of a meta-analysis. Food and Nutrition Bulletin 2009;30:S556-S573. - PubMed
Srinivas 2012
UN 2010
-
- United Nations. Millennium Development Goals. UN Summit on the Millennium Development Goals (http://www.un.org/millenniumgoals) (accessed 2011).
UN 2015
-
- United Nations. Sustainable development goals. sdgs.un.org/goals.
US 2004
-
- US Department of Health and Human Services. The Health Consequences of Smoking. 2004 Surgeon General's Report. U.S. Department of Health and Human Services, 2004.
Van Geertruyden 2004
-
- Van Geertruyden JP, Thomas F, Erhart A, D'Alessandro U. The contribution of malaria in pregnancy to perinatal mortality. American Journal of Tropical Medicine and Hygiene 2004;71(2 Suppl):35-40. - PubMed
Wang 2015
Weiner 2003
Wendland 2012
-
- Wendland EM, Torloni MR, Falavigna M, Trujillo J, Dode MA, Campos MA, et al. Gestational diabetes and pregnancy outcomes--a systematic review of the World Health Organization (WHO) and the International Association of Diabetes in Pregnancy Study Groups (IADPSG) diagnostic criteria. BMC Pregnancy and Childbirth 2012;12:23. [PMID: ] - PMC - PubMed
WHO 2013
-
- WHO. Diagnostic criteria and classification of hyperglycaemia first detected in pregnancy. apps.who.int/iris/bitstream/handle/10665/85975/WHO_NMH_MND_13.2_eng.pdf?... 2013.
WHO 2016
-
- WHO. WHO recommendations on antenatal care for a positive pregnancy experience. www.who.int/publications/i/item/9789241549912 2016. - PubMed
WHO 2020
-
- WHO. KD3B.0 Antepartum fetal death. ICD-11 for Mortality and Morbidity Statistics. Eleventh revision (Version:09/2020) 2020;Available from:https://icd.who.int/browse11/l-m/en#/http%3a%2f%2fid.who.int%2ficd%2fent... Accessed on December 14, 2020..
Zimmermann 2012
-
- Zimmermann MB. The effects of iodine deficiency in pregnancy and infancy. Paediatric and Perinatal Epidemiology 2012;26 Suppl 1:108-17. [PMID: ] - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

