Increased Behavioral Deficits and Inflammation in a Mouse Model of Co-Morbid Traumatic Brain Injury and Post-Traumatic Stress Disorder
- PMID: 33342261
- PMCID: PMC7755938
- DOI: 10.1177/1759091420979567
Increased Behavioral Deficits and Inflammation in a Mouse Model of Co-Morbid Traumatic Brain Injury and Post-Traumatic Stress Disorder
Abstract
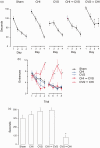
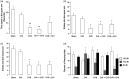
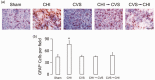
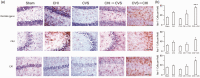
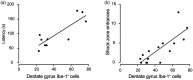
Comorbid post-traumatic stress disorder with traumatic brain injury (TBI) produce more severe affective and cognitive deficits than PTSD or TBI alone. Both PTSD and TBI produce long-lasting neuroinflammation, which may be a key underlying mechanism of the deficits observed in co-morbid TBI/PTSD. We developed a model of co-morbid TBI/PTSD by combining the closed head (CHI) model of TBI with the chronic variable stress (CVS) model of PTSD and examined multiple behavioral and neuroinflammatory outcomes. Male C57/Bl6 mice received sham treatment, CHI, CVS, CHI then CVS (CHI → CVS) or CVS then CHI (CVS → CHI). The CVS → CHI group had deficits in Barnes maze or active place avoidance not seen in the other groups. The CVS → CHI, CVS and CHI → CVS groups displayed increased basal anxiety level, based on performance on elevated plus maze. The CVS → CHI had impaired performance on Barnes Maze, and Active Place Avoidance. These performance deficits were strongly correlated with increased hippocampal Iba-1 level an indication of activated MP/MG. These data suggest that greater cognitive deficits in the CVS → CHI group were due to increased inflammation. The increased deficits and neuroinflammation in the CVS → CHI group suggest that the order by which a subject experiences TBI and PTSD is a major determinant of the outcome of brain injury in co-morbid TBI/PTSD.
Keywords: astrocytes; behavior; cognition; macrophage/microglia; memory.
Conflict of interest statement
Figures



Similar articles
-
Cognitive deficits develop 1month after diffuse brain injury and are exaggerated by microglia-associated reactivity to peripheral immune challenge.Brain Behav Immun. 2016 May;54:95-109. doi: 10.1016/j.bbi.2016.01.009. Epub 2016 Jan 14. Brain Behav Immun. 2016. PMID: 26774527 Free PMC article.
-
Gait and Conditioned Fear Impairments in a Mouse Model of Comorbid TBI and PTSD.Behav Neurol. 2018 Sep 20;2018:6037015. doi: 10.1155/2018/6037015. eCollection 2018. Behav Neurol. 2018. PMID: 30327687 Free PMC article.
-
Transplantation of human neural stem cells restores cognition in an immunodeficient rodent model of traumatic brain injury.Exp Neurol. 2016 Jul;281:1-16. doi: 10.1016/j.expneurol.2016.04.008. Epub 2016 Apr 11. Exp Neurol. 2016. PMID: 27079998
-
Pathophysiological Bases of Comorbidity: Traumatic Brain Injury and Post-Traumatic Stress Disorder.J Neurotrauma. 2018 Jan 15;35(2):210-225. doi: 10.1089/neu.2016.4953. Epub 2017 Nov 3. J Neurotrauma. 2018. PMID: 29017388 Review.
-
Traumatic Brain Injury and Posttraumatic Stress Disorder: Conceptual, Diagnostic, and Therapeutic Considerations in the Context of Co-Occurrence.J Neuropsychiatry Clin Neurosci. 2018 Spring;30(2):91-100. doi: 10.1176/appi.neuropsych.17090180. Epub 2017 Nov 14. J Neuropsychiatry Clin Neurosci. 2018. PMID: 29132272 Review.
Cited by
-
Investigating TSPO levels in occupation-related posttraumatic stress disorder.Sci Rep. 2023 Mar 27;13(1):4970. doi: 10.1038/s41598-023-31327-y. Sci Rep. 2023. PMID: 36973385 Free PMC article.
-
Context is key: glucocorticoid receptor and corticosteroid therapeutics in outcomes after traumatic brain injury.Front Cell Neurosci. 2024 Mar 11;18:1351685. doi: 10.3389/fncel.2024.1351685. eCollection 2024. Front Cell Neurosci. 2024. PMID: 38529007 Free PMC article. Review.
-
Scientific rationale for the use of α2A-adrenoceptor agonists in treating neuroinflammatory cognitive disorders.Mol Psychiatry. 2023 Nov;28(11):4540-4552. doi: 10.1038/s41380-023-02057-4. Epub 2023 Apr 7. Mol Psychiatry. 2023. PMID: 37029295 Free PMC article. Review.
-
Post-traumatic Stress Disorder: Focus on Neuroinflammation.Mol Neurobiol. 2023 Jul;60(7):3963-3978. doi: 10.1007/s12035-023-03320-z. Epub 2023 Apr 1. Mol Neurobiol. 2023. PMID: 37004607 Review.
-
Single-Nucleus RNA Sequencing Reveals That Gabra6+ Neurons in Prefrontal Cortex Promote the Progression of PTSD After Shockwave-Induced TBI.Adv Sci (Weinh). 2025 Feb;12(5):e2407000. doi: 10.1002/advs.202407000. Epub 2024 Dec 12. Adv Sci (Weinh). 2025. PMID: 39665190 Free PMC article.
References
-
- Abdel Baki S. G., Kao H.-Y., Kelemen E., Fenton A. A., Bergold P. J. (2009). A hierarchy of neurobehavioral tasks discriminates between mild and moderate brain injury in rats. Brain Research, 1280, 98–106. - PubMed
-
- Aungst S. L., K S., Thompson S. M., Stoica B. M., Faden A. I. (2014). Repeated mild traumatic brain injury causes chronic neuroinflammation, changes in hippocampal synaptic plasticity, and associated cognitive deficits. Journal of Cerebral Blood Flow and Metabolism: Official Journal of the International Society of Cerebral Blood Flow and Metabolism, 34(7), 1223–1232. - PMC - PubMed
-
- Barnes C. A. (1979). Memory deficits associated with senescence: A neurophysiological and behavioral study in the rat. Journal of Comparative and Physiological Psychology, 93(1), 74–104. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
