Impact of the COVID-19 Pandemic on Lung Cancer Screening Program and Subsequent Lung Cancer
- PMID: 33346080
- PMCID: PMC7947221
- DOI: 10.1016/j.jamcollsurg.2020.12.002
Impact of the COVID-19 Pandemic on Lung Cancer Screening Program and Subsequent Lung Cancer
Abstract
Background: Low-dose CT (LDCT) screening reduces lung cancer mortality by at least 20%. The COVID-19 pandemic required an unprecedented shutdown in our institutional LDCT program. The purpose of this study was to examine the impact of COVID-19 on lung cancer screening and subsequent cancer diagnosis.
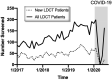
Study design: We analyzed our prospective institutional LDCT screening database, which began in 2012. In all, 2,153 patients have participated. Monthly mean number of LDCTs were compared between baseline (January 2017 to February 2020) and COVID-19 periods (March 2020 to July 2020).
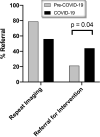
Results: LDCT was suspended on March 13, 2020 and 818 screening visits were cancelled. Phased reopening began on May 5, 2020 and full opening on June 1, 2020. Total monthly mean ± SD LDCTs (146 ± 31 vs 39 ± 40; p < 0.01) and new patient monthly LDCTs (56 ± 14 vs 15 ± 17; p < 0.01) were significantly decreased during the COVID-19 period. New patient monthly LDCTs have remained low despite resuming full operations. Three- and 6-month interval follow-up LDCTs were prioritized and were significantly increased compared with baseline (11 ± 4 vs 30 ± 4; p < 0.01). The "no-show" rate was significantly increased from baseline (15% vs 40%; p < 0.04). Most concerning, the percentage of patients with lung nodules suspicious for malignancy (Lung-RADS 4) were significantly increased after screenings resumed (8% vs 29%; p < 0.01).
Conclusions: COVID-19 caused significant disruption in lung cancer screening, leading to a decrease in new patients screened and an increased proportion of nodules suspicious for malignancy once screening resumed. Using lung cancer and the LDCT screening program as a model, this early analysis showed the unrecognized consequences related to the pandemic for screening programs and cancer care.
Published by Elsevier Inc.
Figures
Comment in
-
Invited Commentary.J Am Coll Surg. 2021 Apr;232(4):605-606. doi: 10.1016/j.jamcollsurg.2020.12.032. J Am Coll Surg. 2021. PMID: 33771318 Free PMC article. No abstract available.
References
-
- Siegel R.L., Miller K.D., Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70:7–30. - PubMed
-
- National Center for Chronic Disease Prevention and Health Promotion . Centers for Disease Control and Prevention; Atlanta, GA: 2014. Office on Smoking and Health. The Health Consequences of Smoking—50 Years of Progress: A Report of the Surgeon General.
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical