Heterogeneity in Genomic Risk Assessment from Tissue Based Prognostic Signatures Used in the Biopsy Setting and the Impact of Magnetic Resonance Imaging Targeted Biopsy
- PMID: 33356482
- PMCID: PMC8443270
- DOI: 10.1097/JU.0000000000001559
Heterogeneity in Genomic Risk Assessment from Tissue Based Prognostic Signatures Used in the Biopsy Setting and the Impact of Magnetic Resonance Imaging Targeted Biopsy
Abstract
Purpose: Genomic prognostic signatures are used on prostate biopsy tissue for cancer risk assessment, but tumor heterogeneity and multifocality may be an issue. We evaluated the variability in genomic risk assessment from different biopsy cores within the prostate using 3 prognostic signatures (Decipher, CCP, GPS).
Materials and methods: Men in this study came from 2 prospective prostate cancer trials of patients undergoing multiparametric magnetic resonance imaging and magnetic resonance imaging targeted biopsy with genomic profiling of positive biopsy cores. We explored the relationship among tumor grade, magnetic resonance imaging risk and genomic risk for each signature. We evaluated the variability in genomic risk assessment between different biopsy cores and assessed how often magnetic resonance imaging targeted biopsy or the current standard of care (profiling the core with the highest grade) resulted in the highest genomic risk level.
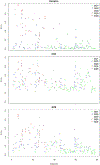
Results: In all, 224 positive biopsy cores from 78 men with prostate cancer were profiled. For each signature, higher biopsy grade (p <0.001) and magnetic resonance imaging risk level (p <0.001) were associated with higher genomic scores. Genomic scores from different biopsy cores varied with risk categories changing by 21% to 62% depending on which core or signature was used. Magnetic resonance imaging targeted biopsy and profiling the core with the highest grade resulted in the highest genomic risk level in 72% to 84% and 75% to 87% of cases, respectively, depending on the signature used.
Conclusions: There is variation in genomic risk assessment from different biopsy cores regardless of the signature used. Magnetic resonance imaging directed biopsy or profiling the highest grade core resulted in the highest genomic risk level in most cases.
Keywords: biomarkers; genomics; magnetic resonance imaging; prostatic neoplasms.
Figures



Comment in
-
Editorial Comment.J Urol. 2021 May;205(5):1351. doi: 10.1097/JU.0000000000001559.01. Epub 2021 Feb 26. J Urol. 2021. PMID: 33635091 No abstract available.
References
-
- Dall’Era MA, Dall’Era MA, Albertsen PC, et al. : Active Surveillance for Prostate Cancer: A Systematic Review of the Literature. Eur Urol. 2012: 62: 976–83 - PubMed
-
- Moldovan PC, Van den Broeck T, Sylvester R, et al. : What Is the Negative Predictive Value of Multiparametric Magnetic Resonance Imaging in Excluding Prostate Cancer at Biopsy? A Systematic Review and Meta-analysis from the European Association of Urology Prostate Cancer Guidelines Panel. Eur Urol. 2017: 72: 250–266. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

