mHealth spectroscopy of blood hemoglobin with spectral super-resolution
- PMID: 33365364
- PMCID: PMC7755164
- DOI: 10.1364/optica.390409
mHealth spectroscopy of blood hemoglobin with spectral super-resolution
Abstract
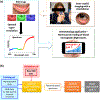
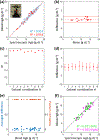
Although blood hemoglobin (Hgb) testing is a routine procedure in a variety of clinical situations, noninvasive, continuous, and real-time blood Hgb measurements are still challenging. Optical spectroscopy can offer noninvasive blood Hgb quantification, but requires bulky optical components that intrinsically limit the development of mobile health (mHealth) technologies. Here, we report spectral super-resolution (SSR) spectroscopy that virtually transforms the built-in camera (RGB sensor) of a smartphone into a hyperspectral imager for accurate and precise blood Hgb analyses. Statistical learning of SSR enables us to reconstruct detailed spectra from three color RGB data. Peripheral tissue imaging with a mobile application is further combined to compute exact blood Hgb content without a priori personalized calibration. Measurements over a wide range of blood Hgb values show reliable performance of SSR blood Hgb quantification. Given that SSR does not require additional hardware accessories, the mobility, simplicity, and affordability of conventional smartphones support the idea that SSR blood Hgb measurements can be used as an mHealth method.
Conflict of interest statement
Disclosures. SMP, MAV, MMH, and YLK are the inventors of provisional patent applications related to this work that have been filed to the U.S. Patents and Trademark Office by the Purdue Research Foundation (application Nos. 62945816 and 62945808 filed December 10, 2019). YLK is a founding member of HemaChrome, LLC. All other authors declare no conflicts of interest.
Figures

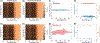

Similar articles
-
Compressive recovery of smartphone RGB spectral sensitivity functions.Opt Express. 2021 Apr 12;29(8):11947-11961. doi: 10.1364/OE.420069. Opt Express. 2021. PMID: 33984965 Free PMC article.
-
mHealth hyperspectral learning for instantaneous spatiospectral imaging of hemodynamics.PNAS Nexus. 2023 Mar 29;2(4):pgad111. doi: 10.1093/pnasnexus/pgad111. eCollection 2023 Apr. PNAS Nexus. 2023. PMID: 37113981 Free PMC article.
-
Combined reflectance spectroscopy and stochastic modeling approach for noninvasive hemoglobin determination via palpebral conjunctiva.Physiol Rep. 2014 Jan 8;2(1):e00192. doi: 10.1002/phy2.192. eCollection 2014 Jan 1. Physiol Rep. 2014. PMID: 24744871 Free PMC article.
-
Sensor-Based mHealth Authentication for Real-Time Remote Healthcare Monitoring System: A Multilayer Systematic Review.J Med Syst. 2019 Jan 6;43(2):33. doi: 10.1007/s10916-018-1149-5. J Med Syst. 2019. PMID: 30612191
-
Emerging Technologies of Three-Dimensional Printing and Mobile Health in COVID-19 Immunity and Regenerative Dentistry.Tissue Eng Part C Methods. 2023 May;29(5):163-182. doi: 10.1089/ten.TEC.2022.0160. Epub 2023 Mar 24. Tissue Eng Part C Methods. 2023. PMID: 36200626 Review.
Cited by
-
Prediction of anemia in real-time using a smartphone camera processing conjunctival images.PLoS One. 2024 May 13;19(5):e0302883. doi: 10.1371/journal.pone.0302883. eCollection 2024. PLoS One. 2024. PMID: 38739605 Free PMC article.
-
Identification and Quantification of Jaundice by Trans-Conjunctiva Optical Imaging Using a Human Brain-like Algorithm: A Cross-Sectional Study.Diagnostics (Basel). 2023 May 17;13(10):1767. doi: 10.3390/diagnostics13101767. Diagnostics (Basel). 2023. PMID: 37238251 Free PMC article.
-
Optical density based quantification of total haemoglobin concentrations with spectroscopic optical coherence tomography.Sci Rep. 2021 Apr 21;11(1):8680. doi: 10.1038/s41598-021-88063-4. Sci Rep. 2021. PMID: 33883617 Free PMC article.
-
Prediction of anemia and estimation of hemoglobin concentration using a smartphone camera.PLoS One. 2021 Jul 14;16(7):e0253495. doi: 10.1371/journal.pone.0253495. eCollection 2021. PLoS One. 2021. PMID: 34260592 Free PMC article.
-
A deep learning model for novel systemic biomarkers in photographs of the external eye: a retrospective study.Lancet Digit Health. 2023 May;5(5):e257-e264. doi: 10.1016/S2589-7500(23)00022-5. Epub 2023 Mar 23. Lancet Digit Health. 2023. PMID: 36966118 Free PMC article.
References
-
- Hsia CCW, “Mechanisms of disease - respiratory function of hemoglobin,” N. Engl. J. Med 338, 239–247 (1998). - PubMed
-
- Cannon JW, “Hemorrhagic shock,” N. Engl. J. Med 378, 370–379 (2018). - PubMed
-
- Hasan MN, Fraiwan A, Thota P, Oginni T, Olanipekun GM, Hassan-Hanga F, Little J, Obaro SK, and Gurkan UA, “Clinical testing of hemechip in Nigeria for point-of-care screening of sickle cell disease,” Blood 132, 1095 (2018). - PubMed
-
- Juul SE, Derman RJ, and Auerbach M, “Perinatal iron deficiency: implications for mothers and infants,” Neonatology 115, 269–274 (2019). - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
