Evolving utilization of donation after circulatory death livers in liver transplantation: The day of DCD has come
- PMID: 33368701
- PMCID: PMC7969458
- DOI: 10.1111/ctr.14211
Evolving utilization of donation after circulatory death livers in liver transplantation: The day of DCD has come
Abstract
Compared to donation after brain death (DBD), livers procured for transplantation from donation after circulatory death (DCD) donors experience more ischemia-reperfusion injury and higher rates of ischemic cholangiopathy due to the period of warm ischemic time (WIT) following withdrawal of life support. As a result, utilization of DCD livers for liver transplant (LT) has generally been limited to short WITs and younger aged donor grafts, causing many recovered DCD organs to be discarded without consideration for transplant. This study assesses how DCD liver utilization and outcomes have changed over time, using OPTN data from adult, first-time, deceased donor, whole-organ LTs between January 1995 and December 2019. Results show that increased clinical experience with DCD LT has translated into increased use of livers from DCD donors, shorter ischemic times, shorter lengths of hospitalization after transplant, and lower rates of retransplantation. The data also reveal that over the past decade, the rate of increase in DCD LTs conducted in the United States has outpaced that of DBD. Together, these trends signal an opportunity for the field of liver transplantation to mitigate the organ shortage by capitalizing on DCD liver allografts that are currently not being utilized.
Keywords: ex vivo liver perfusion; graft survival; liver transplant; machine perfusion; retransplantation.
© 2020 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd.
Conflict of interest statement
CONFLICT OF INTEREST
The authors have no conflicts of interest.
Figures

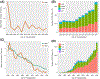
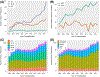



References
-
- Thuong M, Ruiz A, Evrard P, et al. New classification of donation after circulatory death donors definitions and terminology. Transpl Int. 2016;29:749–759. - PubMed
-
- Jay CL, Lyuksemburg V, Ladner DP, et al. Ischemic cholangiopathy after controlled donation after cardiac death liver transplantation: A meta-analysis. Ann Surg. 2011;14:604–610. - PubMed
-
- Fujita S, Mizuno S, Fujikawa T, et al. Liver transplantation from donation after cardiac death: A single center experience. Transplantation. 2007;84:46–49. - PubMed
-
- Manzarbeitia CY, Ortiz JA, Jeon H, et al. Long-term outcome of controlled, non-heart-beating donor liver transplantation. Transplantation. 2004;78:211–215. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

