Current Knowledge on Graves' Orbitopathy
- PMID: 33374706
- PMCID: PMC7793490
- DOI: 10.3390/jcm10010016
Current Knowledge on Graves' Orbitopathy
Abstract
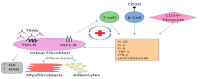
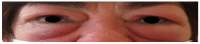
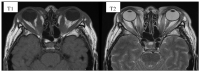
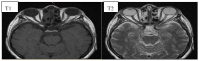
(1) Background: Graves' orbitopathy (GO) is an autoimmune inflammation of the orbital tissues and the most common extra-thyroid symptom of Graves' disease (GD). Mild cases of GO are often misdiagnosed, which prolongs the diagnostic and therapeutic process, leading to exacerbation of the disease. A severe course of GO may cause permanent vision loss. (2) Methods: The article presents an analysis of GO-its etiopathogenesis, diagnostics, current treatment and potential future therapeutic options based on a review of the currently available literature of the subject. (3) Results: Current treatment of the active GO consists predominantly in intravenous glucocorticoids (GCs) administration in combination with orbital radiotherapy. The growing knowledge on the pathogenesis of the disease has contributed to multiple trials of the use of immunosuppressive drugs and monoclonal antibodies which may be potentially effective in the treatment of GO. Immunosuppressive treatment is not effective in patients in whom a chronic inflammatory process has caused fibrous changes in the orbits. In such cases surgical treatment is performed-including orbital decompression, adipose tissue removal, oculomotor muscle surgery, eyelid alignment and blepharoplasty. (4) Conclusions: Management of GO is difficult and requires interdisciplinary cooperation in endocrinology; ophthalmology, radiation oncology and surgery. The possibilities of undertaking a reliable assessment and comparison of the efficacy and safety of the therapeutic strategies are limited due to the heterogeneity of the available studies conducted mostly on small group of patients, with no comparison with classic systemic steroid therapy. The registration by FDA of Teprotumumab, an IGF1-R antagonist, in January 2020 may be a milestone in future management of active GO. However, many clinical questions require to be investigated first.
Keywords: Graves’ disease; Graves’ orbitopathy; clinical activity score; glucocorticoids; immunosuppressive treatment; radiotherapy.
Conflict of interest statement
The authors declare no conflict of interest
Figures
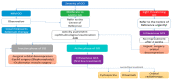
References
-
- Bartalena L., Baldeschi L., Dickinson A., Eckstein A., Kendall-Taylor P., Marcocci C., Mourits M., Perros P., Boboridis K., Boschi A., et al. Consensus statement of the European Group on Graves’ orbitopathy (EUGOGO) on management of GO. Eur. J. Endocrinol. 2008;158:273–285. doi: 10.1530/EJE-07-0666. - DOI - PubMed
-
- Tanda M.L., Piantanida E., Liparulo L., Veronesi G., Lai A., Sassi L., Pariani N., Gallo D., Azzolini C., Ferrario M., et al. Prevalence and natural history of Graves’ orbitopathy in a large series of patients with newly diagnosed graves’ hyperthyroidism seen at a single center. J. Clin. Endocrinol. Metab. 2013;98:1443–1449. doi: 10.1210/jc.2012-3873. - DOI - PubMed
-
- Villadolid M.C., Yokoyama N., Izumi M., Nishikawa T., Kimura H., Ashizawa K., Kiriyama T., Uetani M., Nagataki S. Untreated Graves’ disease patients without clinical ophthalmopathy demonstrate a high frequency of extraocular muscle (EOM) enlargement by magnetic resonance. J. Clin. Endocrinol. Metab. 1995;80:2830–2833. doi: 10.1210/jcem.80.9.7673432. - DOI - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

