Magnetic resonance imaging biomarkers of cerebrospinal fluid tracer dynamics in idiopathic normal pressure hydrocephalus
- PMID: 33381757
- PMCID: PMC7753057
- DOI: 10.1093/braincomms/fcaa187
Magnetic resonance imaging biomarkers of cerebrospinal fluid tracer dynamics in idiopathic normal pressure hydrocephalus
Abstract
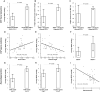
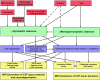
Disturbed clearance of toxic metabolites from the brain via cerebrospinal fluid is emerging as an important mechanism behind dementia and neurodegeneration. To this end, magnetic resonance imaging work-up of dementia diseases is largely focused on anatomical derangements of the brain. This study explores magnetic resonance imaging biomarkers of cerebrospinal fluid tracer dynamics in patients with the dementia subtype idiopathic normal pressure hydrocephalus and a cohort of reference subjects. All study participants underwent multi-phase magnetic resonance imaging up to 48 h after intrathecal administration of the contrast agent gadobutrol (0.5 ml, 1 mmol/ml), serving as cerebrospinal fluid tracer. Imaging biomarkers of cerebrospinal fluid tracer dynamics (i.e. ventricular reflux grades 0-4 and clearance) were compared with anatomical magnetic resonance imaging biomarkers of cerebrospinal fluid space anatomy (Evans' index, callosal angle and disproportional enlargement of subarachnoid spaces hydrocephalus) and neurodegeneration (Schelten's medial temporal atrophy scores, Fazeka's scores and entorhinal cortex thickness). The imaging scores were also related to a pulsatile intracranial pressure score indicative of intracranial compliance. In shunt-responsive idiopathic normal pressure hydrocephalus, the imaging biomarkers demonstrated significantly altered cerebrospinal fluid tracer dynamics (ventricular reflux grades 3-4 and reduced clearance of tracer), deranged cerebrospinal fluid space anatomy and pronounced neurodegeneration. The altered MRI biomarkers were accompanied by pressure indices of impaired intracranial compliance. In conclusion, we present novel magnetic resonance imaging biomarkers characterizing idiopathic normal pressure hydrocephalus pathophysiology, namely measures of cerebrospinal fluid molecular redistribution and clearance, which add information to traditional imaging scores of cerebrospinal fluid space anatomy and neurodegeneration.
Keywords: ICP; MRI biomarkers; cerebrospinal fluid; glymphatic system; idiopathic normal pressure hydrocephalus.
© The Author(s) (2020). Published by Oxford University Press on behalf of the Guarantors of Brain.
Figures



References
-
- Algin O, Hakyemez B, Ocakoglu G, Parlak M. MR cisternography: is it useful in the diagnosis of normal-pressure hydrocephalus and the selection of “good shunt responders”? Diag Interv Radiol (Ankara, Turkey) 2011; 17: 105–11. - PubMed
-
- Brean A, Eide PK. Prevalence of probable idiopathic normal pressure hydrocephalus in a Norwegian population. Acta Neurol Scand 2008; 118: 48–53. - PubMed
-
- Brix MK, Westman E, Simmons A, Ringstad GA, Eide PK, Wagner-Larsen K, et al. The Evans' Index revisited: new cut-off levels for use in radiological assessment of ventricular enlargement in the elderly. Eur J Radiol 2017; 95: 28–32. - PubMed
-
- Chai AB, Leung GKF, Callaghan R, Gelissen IC. P-glycoprotein: a role in the export of amyloid-beta in Alzheimer's disease? FEBS J 2020; 287: 612–25. - PubMed
LinkOut - more resources
Full Text Sources
