CaSR-Mediated hBMSCs Activity Modulation: Additional Coupling Mechanism in Bone Remodeling Compartment
- PMID: 33396907
- PMCID: PMC7795180
- DOI: 10.3390/ijms22010325
CaSR-Mediated hBMSCs Activity Modulation: Additional Coupling Mechanism in Bone Remodeling Compartment
Abstract
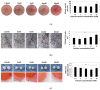
Near the bone remodeling compartments (BRC), extracellular calcium concentration (Ca2+o) is locally elevated and bone marrow stromal cells (BMSCs) close to the BRC can be exposed to high calcium concentration. The calcium-sensing receptor (CaSR) is known to play a key role in maintaining extracellular calcium homeostasis by sensing fluctuations in the levels of extracellular calcium (Ca2+o). When human BMSCs (hBMSCs) were exposed to various calcium concentrations (1.8, 3, 5, 10, 30 mM), moderate-high extracellular calcium concentrations (3-5 mM) stimulated proliferation, while a high calcium concentration (30 mM) inhibited the proliferation. Exposure to various calcium concentrations did not induce significant differences in the apoptotic cell fraction. Evaluation of multi-lineage differentiation potential showed no significant difference among various calcium concentration groups, except for the high calcium concentration (30 mM) treated group, which resulted in increased calcification after in vitro osteogenic differentiation. Treatment of NPS2143, a CaSR inhibitor, abolished the stimulatory effect on hBMSCs proliferation and migration indicating that CaSR is involved. These results suggest that the calcium concentration gradient near the BRC may play an important role in bone remodeling by acting as an osteoblast-osteoclast coupling mechanism through CaSR.
Keywords: bone remodeling; calcium-sensing receptor; osteoblast-osteoclast coupling; proliferation.
Conflict of interest statement
The authors declare no conflict of interest.
Figures






References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

