Clinical Usefulness of Furosemide to Prevent Volume Overload Among Children and Young Adults with Transfusion-Dependent Thalassemia: A Randomized, Open-Label, Crossover Study
- PMID: 33402857
- PMCID: PMC7778446
- DOI: 10.2147/JBM.S285647
Clinical Usefulness of Furosemide to Prevent Volume Overload Among Children and Young Adults with Transfusion-Dependent Thalassemia: A Randomized, Open-Label, Crossover Study
Abstract
Purpose: Red blood cell transfusion is a key element of treatment among patients with transfusion-dependent thalassemia (TDT). Volume overload and HCC syndrome (hypertension, convulsion, and intracranial hemorrhage) are fatal complications related to transfusion. Furosemide has been widely used to prevent hypertension secondary to volume overload with unclear supportive evidence. This study aimed to evaluate the efficacy of furosemide to prevent volume overload among children and young adults diagnosed with TDT.
Methods: Patients diagnosed with TDT were enrolled and randomized to receive either furosemide pretransfusion or no furosemide pretransfusion. After 3 weeks to 4 months of wash-out periods, those patients underwent the alternate regimens as per crossover design of the study. Clinical and laboratory parameters including blood pressure and NT-proBNP levels were measured before and after each transfusion. The difference of those parameters between two randomized groups and their potential associated factors were analyzed.
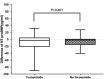
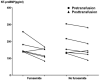
Results: In all, 30 patients undergoing 60 red blood cell transfusions were enrolled in the study. All were randomized and crossover was designed as receiving and not receiving furosemide pretransfusion. No transfusion reactions, symptoms of volume overload and HCC syndrome were observed. No statistically significant correlation was found between pretransfusion furosemide and the difference between pre- and posttransfusion systolic blood pressure (2 mmHg systolic blood pressure difference in pretransfusion furosemide and 1.5 mmHg in no pretransfusion furosemide; p-value = 0.721), as well as between pretransfusion furosemide and the difference between pre- and posttransfusion NT-proBNP levels (-3.8 pg/mL NT-proBNP level difference in pretransfusion furosemide and -2.4 pg/mL in no pretransfusion furosemide; p-value = 0.490). No significant correlation was also observed even in selected patients with high NT-proBNP levels (p-value = 0.262). Associated factors affecting the difference between pre- and posttransfusion NT-proBNP levels were analyzed, and none of those were affected concerning the difference in the levels.
Conclusion: Furosemide has been included in standard transfusion guidelines in many institutions. Our study provided important evidence of the unnecessary use of the drug in preventing volume overload particularly in pediatric and young adult patients with TDT.
Thai clinical trials registry tctr number: TCTR20180209001. Registered 6 February 2018, https://www.clinicaltrials.in.th/.
Keywords: NT-proBNP; furosemide; thalassemia; transfusion; volume overload.
© 2020 Photia et al.
Conflict of interest statement
All authors report no conflicts of interest in this work.
Figures

Similar articles
-
Cardiac stress biomarkers after red blood cell transfusion in patients at risk for transfusion-associated circulatory overload: a prospective observational study.Transfusion. 2018 Sep;58(9):2139-2148. doi: 10.1111/trf.14820. Transfusion. 2018. PMID: 30204946
-
Transfusion-associated circulatory overload-a systematic review of diagnostic biomarkers.Transfusion. 2019 Feb;59(2):795-805. doi: 10.1111/trf.15068. Epub 2018 Nov 29. Transfusion. 2019. PMID: 30488959 Free PMC article.
-
Influence of cross-match on posttransfusion packed cell volume in feline packed red blood cell transfusion.J Vet Emerg Crit Care (San Antonio). 2014 Jul-Aug;24(4):429-36. doi: 10.1111/vec.12204. Epub 2014 Jul 15. J Vet Emerg Crit Care (San Antonio). 2014. PMID: 25039745
-
Association between vitamin D levels and left ventricular function and NT-proBNP levels among thalassemia major children with iron overload.Ann Pediatr Cardiol. 2016 May-Aug;9(2):126-31. doi: 10.4103/0974-2069.181495. Ann Pediatr Cardiol. 2016. PMID: 27212846 Free PMC article.
-
Systematic Literature Review of the Burden of Disease and Treatment for Transfusion-dependent β-Thalassemia.Clin Ther. 2020 Feb;42(2):322-337.e2. doi: 10.1016/j.clinthera.2019.12.003. Epub 2019 Dec 24. Clin Ther. 2020. PMID: 31882227
Cited by
-
Coagulation and Fibrinolysis Dysregulation in β-Thalassemia Major: Potential Impact of Splenectomy and Medications on Thrombotic Risk.Clin Appl Thromb Hemost. 2025 Jan-Dec;31:10760296251359291. doi: 10.1177/10760296251359291. Epub 2025 Jul 14. Clin Appl Thromb Hemost. 2025. PMID: 40660796 Free PMC article.
References
LinkOut - more resources
Full Text Sources
Research Materials

