Large airway diseases in pediatrics: a pictorial essay
- PMID: 33403124
- PMCID: PMC7747119
- DOI: 10.1177/2058460120972694
Large airway diseases in pediatrics: a pictorial essay
Abstract
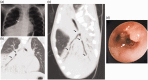
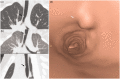
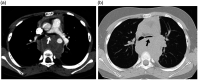
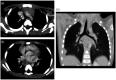
"Large airway diseases" is being used as an all-encompassing phrase to describe a broad spectrum of pathological entities, which involves the trachea, main, lobar, and segmental bronchi of up to 3 mm diameter. Imaging modalities such as radiography, computed tomography, and magnetic resonance imaging contribute to the identification and diagnosis of each entity. Knowledge of clinical information, normal cross-sectional anatomy, and imaging characteristics of large airway diseases is necessary for appropriate radiologic evaluation. This review provides information about congenital and acquired diseases of the large airways in the pediatric population.
Keywords: CT; Chest; airways; bronchi; pediatric; trachea.
© The Foundation Acta Radiologica 2020.
Conflict of interest statement
Declaration of Conflicting Interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
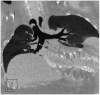
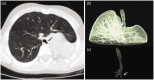
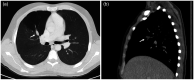
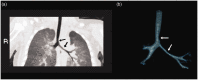
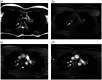
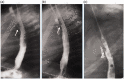
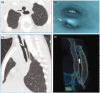
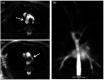

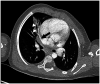
References
-
- Chassagnon G, Morel B, Carpentier E, et al. Tracheobronchial branching abnormalities: lobe-based classification scheme. Radiographics 2016; 36:358–373. - PubMed
-
- Lee EY, Greenberg BS, Boiselle PM. Multidetector computed tomography of pediatric large airway diseases: state-of-the-art. Radiol Clin N Am 2011; 49:869–893. - PubMed
-
- Ghaye B, Szapiro D, Fanchamps JM, et al. Congenital bronchial abnormalities revisited. Radiographics 2001; 21:105–119. - PubMed
-
- Semple ΤT, Calder A, Owens CM, et al. Current and future approaches to large airways imaging in adults and children. Clin Radiol 2017; 27:356–374. - PubMed
LinkOut - more resources
Full Text Sources

