Increased development of radiographic hip osteoarthritis in individuals with high bone mass: a prospective cohort study
- PMID: 33407835
- PMCID: PMC7788917
- DOI: 10.1186/s13075-020-02371-0
Increased development of radiographic hip osteoarthritis in individuals with high bone mass: a prospective cohort study
Abstract
Background: Individuals with high bone mass (HBM) have a greater odds of prevalent radiographic hip osteoarthritis (OA), reflecting an association with bone-forming OA sub-phenotypes (e.g. osteophytosis, subchondral sclerosis). As the role of bone mineral density (BMD) in hip OA progression is unclear, we aimed to determine if individuals with HBM have increased incidence and/or progression of bone-forming OA sub-phenotypes.
Methods: We analysed an adult cohort with and without HBM (L1 and/or total hip BMD Z-score > + 3.2) with pelvic radiographs collected at baseline and 8-year follow-up. Sub-phenotypes were graded using the OARSI atlas. Superior/inferior acetabular/femoral osteophyte and medial/superior joint space narrowing (JSN) grades were summed and Δosteophyte and ΔJSN derived. Pain and functional limitations were quantified using the WOMAC questionnaire. Associations between HBM status and change in OA sub-phenotypes were determined using multivariable linear/logistic regression, adjusting for age, sex, height, total body fat mass, follow-up time and baseline sub-phenotype grade. Generalised estimating equations accounted for individual-level clustering.
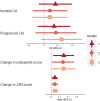
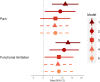
Results: Of 136 individuals, 62% had HBM at baseline, 72% were female and mean (SD) age was 59 (10) years. HBM was positively associated with both Δosteophytes and ΔJSN (adjusted mean grade differences between individuals with and without HBM βosteophyte = 0.30 [0.01, 0.58], p = 0.019 and βJSN = 0.10 [0.01, 0.18], p = 0.019). Incident subchondral sclerosis was rare. HBM individuals had higher WOMAC hip functional limitation scores (β = 8.3 [0.7, 15.98], p = 0.032).
Conclusions: HBM is associated with the worsening of hip osteophytes and JSN over an average of 8 years, as well as increased hip pain and functional limitation.
Keywords: BMD; High bone mass; Hip osteoarthritis; Progression; WOMAC.
Conflict of interest statement
The authors have no competing interests to disclose.
Figures
References
-
- Stewart A, Black A, Robins SP, Reid DM. Bone density and bone turnover in patients with osteoarthritis and osteoporosis. J Rheumatol. 1999;26(3):622–626. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

