Associations between breast cancer survivorship and adverse mental health outcomes: A matched population-based cohort study in the United Kingdom
- PMID: 33411711
- PMCID: PMC7822529
- DOI: 10.1371/journal.pmed.1003504
Associations between breast cancer survivorship and adverse mental health outcomes: A matched population-based cohort study in the United Kingdom
Abstract
Background: Breast cancer is the most common cancer diagnosed in women globally, and 5-year net survival probabilities in high-income countries are generally >80%. A cancer diagnosis and treatment are often traumatic events, and many women struggle to cope during this period. Less is known, however, about the long-term mental health impact of the disease, despite many women living several years beyond their breast cancer and mental health being a major source of disability in modern societies. The objective of this study was to quantify the risk of several adverse mental health-related outcomes in women with a history of breast cancer followed in primary care in the United Kingdom National Health Service, compared to similar women who never had cancer.
Methods and findings: We conducted a matched cohort study using data routinely collected in primary care across the UK to quantify associations between breast cancer history and depression, anxiety, and other mental health-related outcomes. All women with incident breast cancer in the Clinical Practice Research Datalink (CPRD) GOLD primary care database between 1988 and 2018 (N = 57,571, mean = 62 ± 14 years) were matched 1:4 to women with no prior cancer (N = 230,067) based on age, primary care practice, and eligibility of the data for linkage to hospital data sources. Cox models were used to estimate associations between breast cancer survivorship and each mental health-related outcome, further adjusting for diabetes, body mass index (BMI), and smoking and drinking status at baseline. Breast cancer survivorship was positively associated with anxiety (adjusted hazard ratio (HR) = 1.33; 95% confidence interval (CI): 1.29-1.36; p < 0.001), depression (1.35; 1.32-1.38; p < 0.001), sexual dysfunction (1.27; 1.17-1.38; p < 0.001), and sleep disorder (1.68; 1.63-1.73; p < 0.001), but not with cognitive dysfunction (1.00; 0.97-1.04; p = 0.88). Positive associations were also found for fatigue (HR = 1.28; 1.25-1.31; p < 0.001), pain (1.22; 1.20-1.24; p < 0.001), receipt of opioid analgesics (1.86; 1.83-1.90; p < 0.001), and fatal and nonfatal self-harm (1.15; 0.97-1.36; p = 0.11), but CI was wide, and the relationship was not statistically significant for the latter. HRs for anxiety and depression decreased over time (p-interaction <0.001), but increased risks persisted for 2 and 4 years, respectively, after cancer diagnosis. Increased levels of pain and sleep disorder persisted for 10 years. Younger age was associated with larger HRs for depression, cognitive dysfunction, pain, opioid analgesics use, and sleep disorders (p-interaction <0.001 in each case). Limitations of the study include the potential for residual confounding by lifestyle factors and detection bias due to cancer survivors having greater healthcare contact.
Conclusions: In this study, we observed that compared to women with no prior cancer, breast cancer survivors had higher risk of anxiety, depression, sleep problems, sexual dysfunction, fatigue, receipt of opioid analgesics, and pain. Relative risks estimates tended to decrease over time, but anxiety and depression were significantly increased for 2 and 4 years after breast cancer diagnosis, respectively, while associations for fatigue, pain, and sleep disorders were elevated for at least 5-10 years after diagnosis. Early diagnosis and increased awareness among patients, healthcare professionals, and policy makers are likely to be important to mitigate the impacts of these raised risks.
Conflict of interest statement
I have read the journal's policy and the authors of this manuscript have the following competing interests: RW reports that CPRD has financial relationships with its clients, including the London School of Hygiene & Tropical Medicine, in relation to providing access to research data and services both related to and outside of the submitted work. SS reports personal fees from Roche, Clinigen, Eli Lilly, and Novartis, not related to this work. KB reports grants from Wellcome Trust, the Royal Society, Medical Research Council, and British Heart Foundation, outside the submitted work. GF and HC have no conflict of interest to disclose.
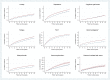
Figures



Similar articles
-
Quality of life and mental health in breast cancer survivors compared with non-cancer controls: a study of patient-reported outcomes in the United Kingdom.J Cancer Surviv. 2021 Aug;15(4):564-575. doi: 10.1007/s11764-020-00950-3. Epub 2020 Oct 21. J Cancer Surviv. 2021. PMID: 33089480 Free PMC article.
-
Common mental health disorders in adults with inflammatory skin conditions: nationwide population-based matched cohort studies in the UK.BMC Med. 2023 Aug 4;21(1):285. doi: 10.1186/s12916-023-02948-x. BMC Med. 2023. PMID: 37542272 Free PMC article.
-
Associations Between Breast Cancer Survivorship and Adverse Mental Health Outcomes: A Systematic Review.J Natl Cancer Inst. 2018 Dec 1;110(12):1311-1327. doi: 10.1093/jnci/djy177. J Natl Cancer Inst. 2018. PMID: 30403799 Free PMC article.
-
Early, medium and long-term mental health in cancer survivors compared with cancer-free comparators: matched cohort study using linked UK electronic health records.EClinicalMedicine. 2024 Sep 16;76:102826. doi: 10.1016/j.eclinm.2024.102826. eCollection 2024 Oct. EClinicalMedicine. 2024. PMID: 39318789 Free PMC article.
-
Supportive care after curative treatment for breast cancer (survivorship care): resource allocations in low- and middle-income countries. A Breast Health Global Initiative 2013 consensus statement.Breast. 2013 Oct;22(5):606-15. doi: 10.1016/j.breast.2013.07.049. Epub 2013 Sep 3. Breast. 2013. PMID: 24007941 Review.
Cited by
-
Health status and associated factors of middle-aged and older adult cancer survivors in India: results from the Longitudinal Ageing Study in India.BMC Cancer. 2022 Oct 22;22(1):1087. doi: 10.1186/s12885-022-10111-7. BMC Cancer. 2022. PMID: 36273166 Free PMC article.
-
Estrogen-Receptor-Positive Breast Cancer in Postmenopausal Women: The Role of Body Composition and Physical Exercise.Int J Environ Res Public Health. 2021 Sep 18;18(18):9834. doi: 10.3390/ijerph18189834. Int J Environ Res Public Health. 2021. PMID: 34574758 Free PMC article. Review.
-
The impact of sleep on breast cancer-specific mortality: a Mendelian randomisation study.BMC Cancer. 2025 Feb 26;25(1):357. doi: 10.1186/s12885-025-13681-4. BMC Cancer. 2025. PMID: 40011859 Free PMC article.
-
Development and Evaluation of the Usefulness, Usability, and Feasibility of iNNOV Breast Cancer: Mixed Methods Study.JMIR Cancer. 2022 Feb 15;8(1):e33550. doi: 10.2196/33550. JMIR Cancer. 2022. PMID: 35166682 Free PMC article.
-
A web-based survey of SARS-CoV-2 vaccination and its adverse effects in Chinese postoperative patients with breast cancer: a cross-sectional study.Gland Surg. 2022 Sep;11(9):1497-1506. doi: 10.21037/gs-22-454. Gland Surg. 2022. PMID: 36221281 Free PMC article.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

