Glycemic indices predict outcomes after aneurysmal subarachnoid hemorrhage: a retrospective single center comparative analysis
- PMID: 33420311
- PMCID: PMC7794316
- DOI: 10.1038/s41598-020-80513-9
Glycemic indices predict outcomes after aneurysmal subarachnoid hemorrhage: a retrospective single center comparative analysis
Abstract
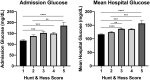
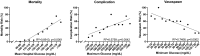
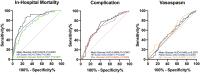
Although hyperglycemia is associated with worse outcomes after aneurysmal subarachnoid hemorrhage (aSAH), there is no consensus on the optimal glucose control metric, acceptable in-hospital glucose ranges, or suitable insulin regimens in this population. In this single-center retrospective cohort study of aSAH patients, admission glucose, and hospital glucose mean (MHG), minimum (MinG), maximum (MaxG), and variability were compared. Primary endpoints (mortality, complications, and vasospasm) were assessed using multivariate logistic regressions. Of the 217 patients included, complications occurred in 83 (38.2%), 124 (57.1%) had vasospasm, and 41 (18.9%) died. MHG was independently associated with (p < 0.001) mortality, MaxG (p = 0.017) with complications, and lower MinG (p = 0.015) with vasospasm. Patients with MHG ≥ 140 mg/dL had 10 × increased odds of death [odds ratio (OR) = 10.3; 95% CI 4.6-21.5; p < 0.0001] while those with MinG ≤ 90 mg/dL had nearly 2× increased odds of vasospasm (OR = 1.8; 95% CI 1.01-3.21; p = 0.0422). While inpatient insulin was associated with increased complications and provided no mortality benefit, among those with MHG ≥ 140 mg/dL insulin therapy resulted in lower mortality (OR = 0.3; 95% CI 0.1-0.9; p = 0.0358), but no increased complication risk. While elevated MHG and MaxG are highly associated with poorer outcomes after aSAH, lower MinG is associated with increased vasospasm risk. Future trials should consider initiating insulin therapy based on MHG rather than other hyperglycemia measures.
Conflict of interest statement
The authors declare no competing interests.
Figures
Similar articles
-
Low total cholesterol and high density lipoprotein are independent predictors of poor outcomes following aneurysmal subarachnoid hemorrhage: A preliminary report.Clin Neurol Neurosurg. 2020 Oct;197:106062. doi: 10.1016/j.clineuro.2020.106062. Epub 2020 Jul 2. Clin Neurol Neurosurg. 2020. PMID: 32688095
-
Clinical characteristics and outcomes of neurogenic stress cadiomyopathy in aneurysmal subarachnoid hemorrhage.Clin Neurol Neurosurg. 2013 Jul;115(7):909-14. doi: 10.1016/j.clineuro.2012.09.006. Epub 2012 Sep 26. Clin Neurol Neurosurg. 2013. PMID: 23021080
-
Relationship between hyperglycemia and symptomatic vasospasm after subarachnoid hemorrhage.Crit Care Med. 2005 Jul;33(7):1603-9; quiz 1623. doi: 10.1097/01.ccm.0000168054.60538.2b. Crit Care Med. 2005. PMID: 16003069
-
Efficacy of Cilostazol in Prevention of Delayed Cerebral Ischemia after Aneurysmal Subarachnoid Hemorrhage: A Meta-Analysis.J Stroke Cerebrovasc Dis. 2018 Nov;27(11):2979-2985. doi: 10.1016/j.jstrokecerebrovasdis.2018.06.027. Epub 2018 Aug 6. J Stroke Cerebrovasc Dis. 2018. PMID: 30093204 Review.
-
Simvastatin for the prevention of symptomatic cerebral vasospasm following aneurysmal subarachnoid hemorrhage: a single-institution prospective cohort study.J Neurosurg. 2009 May;110(5):968-74. doi: 10.3171/2008.10.JNS08901. J Neurosurg. 2009. PMID: 19199459 Review.
Cited by
-
Pharmacotherapy in SAH: Clinical Trial Lessons.CNS Neurol Disord Drug Targets. 2024;23(11):1308-1319. doi: 10.2174/0118715273251761231127095039. CNS Neurol Disord Drug Targets. 2024. PMID: 38243987 Review.
-
The prognostic value of hyperglycemia in aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis.Neurosurg Rev. 2022 Dec;45(6):3717-3728. doi: 10.1007/s10143-022-01870-9. Epub 2022 Sep 28. Neurosurg Rev. 2022. PMID: 36169785
-
A 90-Day Prognostic Model Based on the Early Brain Injury Indicators after Aneurysmal Subarachnoid Hemorrhage: the TAPS Score.Transl Stroke Res. 2023 Apr;14(2):200-210. doi: 10.1007/s12975-022-01033-4. Epub 2022 May 14. Transl Stroke Res. 2023. PMID: 35567655 Clinical Trial.
-
Clinical relevance of glucose metrics during the early brain injury period after aneurysmal subarachnoid hemorrhage: An opportunity for continuous glucose monitoring.Front Neurol. 2022 Sep 12;13:977307. doi: 10.3389/fneur.2022.977307. eCollection 2022. Front Neurol. 2022. PMID: 36172028 Free PMC article. Review.
-
Value of Glycemic Indices for Delayed Cerebral Ischemia after Aneurysmal Subarachnoid Hemorrhage: A Retrospective Single-Center Study.Brain Sci. 2024 Aug 23;14(9):849. doi: 10.3390/brainsci14090849. Brain Sci. 2024. PMID: 39335345 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

