Prediction of mechanical ventilation greater than 24 hours in critically ill obstetric patients: ten years of data from a tertiary teaching hospital in mainland China
- PMID: 33422023
- PMCID: PMC7796589
- DOI: 10.1186/s12884-020-03524-4
Prediction of mechanical ventilation greater than 24 hours in critically ill obstetric patients: ten years of data from a tertiary teaching hospital in mainland China
Abstract
Background: Maternal admission to the intensive care unit (ICU) during pregnancy or in the postpartum period is a marker of severe acute maternal morbidity. Mechanical ventilation is an important and basic method of maintaining life support in the ICU, but prolonged mechanical ventilation (PMV) is associated with a prolonged length of hospital stay and other adverse outcomes. Therefore, we conducted this retrospective study to describe morbidity and further try to identify the risk factors for PMV in critically ill obstetric women.
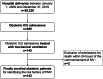
Methods: The clinical data were obtained from a single-centre retrospective comparative study of 143 critically ill obstetric patients at a tertiary teaching hospital in mainland China between January 1, 2009, and December 31, 2019. PMV was defined as a mechanical ventilation length of more than 24 h. Clinical and obstetric parameters were collected to analyse the risk factors for PMV. Patients were separated into groups with and without PMV. Potential risk factors were identified by univariate testing. Multivariate logistic regression was used to evaluate independent predictors of PMV.
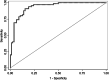
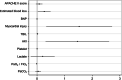
Results: Out of 29,236 hospital deliveries, 265 critically ill obstetric patients entered the ICU. One hundred forty-five (54.7%) of them were treated with mechanical ventilation. Two were excluded because of death within 24 h. Sixty-five critically ill obstetric patients (45.5%) underwent PMV. The independent risk factors for PMV included estimated blood loss (odds ratio (OR) =1.296, P=0.029), acute kidney injury (AKI) (OR=4.305, P=0.013), myocardial injury (OR=4.586, P=0.012), and PaO2/FiO2 (OR=0.989, P< 0.001). The area under the receiver operating characteristic (ROC) curve based on the predicted probability of the logistic regression was 0.934.
Conclusions: Estimated blood loss, AKI, myocardial injury, and PaO2/FiO2 were independent risk factors for PMV in critically ill obstetric patients.
Keywords: Critically ill obstetric patients; Prolonged mechanical ventilation; Risk factors.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
[Analysis of risk factors of prolonged intensive care unit stay of critically ill obstetric patients: a 5-year retrospective review in 3 hospitals in Beijing].Zhongguo Wei Zhong Bing Ji Jiu Yi Xue. 2011 Aug;23(8):449-53. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue. 2011. PMID: 21878165 Chinese.
-
Performance of the Obstetric Early Warning Score in critically ill patients for the prediction of maternal death.Am J Obstet Gynecol. 2017 Jan;216(1):58.e1-58.e8. doi: 10.1016/j.ajog.2016.09.103. Epub 2016 Oct 15. Am J Obstet Gynecol. 2017. PMID: 27751799
-
Using artificial intelligence to predict prolonged mechanical ventilation and tracheostomy placement.J Surg Res. 2018 Aug;228:179-187. doi: 10.1016/j.jss.2018.03.028. Epub 2018 Apr 11. J Surg Res. 2018. PMID: 29907209
-
Liberation from prolonged mechanical ventilation.Crit Care Clin. 2002 Jul;18(3):569-95. doi: 10.1016/s0749-0704(02)00016-7. Crit Care Clin. 2002. PMID: 12140914 Review.
-
Risk Factors for Prolonged Mechanical Ventilation and Weaning Failure: A Systematic Review.Respiration. 2022;101(10):959-969. doi: 10.1159/000525604. Epub 2022 Aug 17. Respiration. 2022. PMID: 35977525 Free PMC article.
Cited by
-
Acute kidney injury in elderly patients receiving invasive mechanical ventilation: early versus late onset.Eur J Med Res. 2024 Dec 18;29(1):590. doi: 10.1186/s40001-024-02157-z. Eur J Med Res. 2024. PMID: 39695893 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

