Circulating Platelet-Derived Extracellular Vesicles Are a Hallmark of Sars-Cov-2 Infection
- PMID: 33430260
- PMCID: PMC7825711
- DOI: 10.3390/cells10010085
Circulating Platelet-Derived Extracellular Vesicles Are a Hallmark of Sars-Cov-2 Infection
Abstract
Sars-Cov-2 infection causes fever and cough that may rapidly lead to acute respiratory distress syndrome (ARDS). Few biomarkers have been identified but, unfortunately, these are individually poorly specific, and novel biomarkers are needed to better predict patient outcome. The aim of this study was to evaluate the diagnostic performance of circulating platelets (PLT)-derived extracellular vesicles (EVs) as biomarkers for Sars-Cov-2 infection, by setting a rapid and reliable test on unmanipulated blood samples. PLT-EVs were quantified by flow cytometry on two independent cohorts of Sars-CoV-2+ (n = 69), Sars-Cov-2- (n = 62) hospitalized patients, and healthy controls. Diagnostic performance of PLT-EVs was evaluated by receiver operating characteristic (ROC) curve. PLT-EVs count were higher in Sars-Cov-2+ compared to Sars-Cov-2- patients or HC. ROC analysis of the combined cohorts showed an AUC = 0.79 and an optimal cut-off value of 1472 EVs/μL, with 75% sensitivity and 74% specificity. These data suggest that PLT-EVs might be an interesting biomarker deserving further investigations to test their predictive power.
Keywords: COVID-19; Sars-Cov-2; circulating biomarker; extracellular vesicles; platelets.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
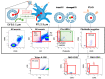

References
-
- Cascella M., Rajnik M., Cuomo A., Dulebohn S.C., Di Napoli R. StatPearls. StatPearls Publishing LLC.; Treasure Island, FL, USA: 2020. Features, Evaluation, and Treatment of Coronavirus. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

