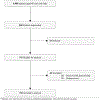
Perceived Versus Actual Risks of 30-Day Readmission in Patients With Cardiovascular Disease
- PMID: 33430612
- PMCID: PMC7855013
- DOI: 10.1161/CIRCOUTCOMES.120.006586
Perceived Versus Actual Risks of 30-Day Readmission in Patients With Cardiovascular Disease
Abstract
Background: Cardiovascular disease (CVD) is the leading cause of hospitalization in the United States, and patients with CVD are at a high risk of readmission after discharge. We examined whether patients' perceived risk of readmission at discharge was associated with actual 30-day readmissions in patients hospitalized with CVD.
Methods: We recruited 730 patients from the Duke Heart Center who were admitted for treatment of CVD between January 1, 2015, and August 31, 2017. A standardized survey was linked with electronic health records to ascertain patients' perceived risk of readmission, and other sociodemographic, psychosocial, behavioral, and clinical data before discharge. All-cause readmission within 30 days after discharge was examined.
Results: Nearly 1-in-3 patients perceived a high risk of readmission at index admission and those who perceived a high risk had significantly more readmissions within 30 days than patients who perceived low risks of readmission (23.6% versus 15.8%, P=0.016). Among those who perceived a high risk of readmission, non-White patients (odds ratio [OR], 2.07 [95% CI, 1.28-3.36]), those with poor self-rated health (OR, 2.30 [95% CI, 1.38-3.85]), difficulty accessing care (OR, 2.72 [95% CI, 1.24-6.00]), and prior hospitalizations in the past year (OR, 2.13 [95% CI, 1.21-3.74]) were more likely to be readmitted. Among those who perceived a low risk of readmission, patients who were widowed (OR, 2.69 [95% CI, 1.60-4.51]) and reported difficulty accessing care (OR, 1.89 [95% CI, 1.07-3.33]) were more likely to be readmitted.
Conclusions: Patients who perceived a high risk of readmission had a higher rate of 30-day readmission than patients who perceived a low risk. These findings have important implications for identifying CVD patients at a high risk of 30-day readmission and targeting the factors associated with perceived and actual risks of readmission.
Keywords: cardiovascular disease; electronic health records; heart failure; hospitalization; risk.
Figures
Similar articles
-
Factors associated with racial differences in all-cause 30-day readmission in adults with cardiovascular disease: an observational study of a large healthcare system.BMJ Open. 2022 Nov 24;12(11):e051661. doi: 10.1136/bmjopen-2021-051661. BMJ Open. 2022. PMID: 36424114 Free PMC article.
-
Access to routine care and risks for 30-day readmission in patients with cardiovascular disease.Am Heart J. 2018 Feb;196:9-17. doi: 10.1016/j.ahj.2017.10.001. Epub 2017 Oct 5. Am Heart J. 2018. PMID: 29421019 Free PMC article.
-
Readmissions Following a Hospitalization for Cardiovascular Events in Dialysis Patients: A Retrospective Cohort Study.J Am Heart Assoc. 2018 Feb 13;7(4):e007231. doi: 10.1161/JAHA.117.007231. J Am Heart Assoc. 2018. PMID: 29440035 Free PMC article.
-
Causes and predictors of 30-day readmission after cardiovascular implantable electronic devices implantation: Insights from Nationwide Readmissions Database.J Cardiovasc Electrophysiol. 2018 Mar;29(3):456-462. doi: 10.1111/jce.13396. Epub 2017 Dec 20. J Cardiovasc Electrophysiol. 2018. PMID: 29193418
-
Identifying Nonclinical Factors Associated With 30-Day Readmission in Patients with Cardiovascular Disease: Protocol for an Observational Study.JMIR Res Protoc. 2017 Jun 15;6(6):e118. doi: 10.2196/resprot.7434. JMIR Res Protoc. 2017. PMID: 28619703 Free PMC article.
Cited by
-
What CVD risk factors predict self-perceived risk of having a myocardial infarction? A cross-sectional study.Int J Cardiol Cardiovasc Risk Prev. 2022 Jan 13;12:200125. doi: 10.1016/j.ijcrp.2022.200125. eCollection 2022 Mar. Int J Cardiol Cardiovasc Risk Prev. 2022. PMID: 35243482 Free PMC article.
-
Reducing rehospitalization in cardiac patients: a randomized, controlled trial of a cardiac care management program ("Cardiolotse") in Germany.BMC Med. 2024 Oct 21;22(1):480. doi: 10.1186/s12916-024-03691-7. BMC Med. 2024. PMID: 39428539 Free PMC article. Clinical Trial.
-
Effectiveness of Telemedicine Visits in Reducing 30-Day Readmissions Among Patients With Heart Failure During the COVID-19 Pandemic.J Am Heart Assoc. 2022 Apr 5;11(7):e023935. doi: 10.1161/JAHA.121.023935. Epub 2022 Mar 1. J Am Heart Assoc. 2022. PMID: 35229656 Free PMC article.
-
Predictors of 30-Day Re-admission in Cardiac Patients at Heart Hospital, Qatar.Heart Views. 2023 Jul-Sep;24(3):125-135. doi: 10.4103/heartviews.heartviews_91_22. Epub 2023 Jul 5. Heart Views. 2023. PMID: 37584026 Free PMC article.
References
-
- Benjamin EJ, Muntner P, Bittencourt MS. Heart disease and stroke statistics-2019 update: a report from the American Heart Association. Circulation. 2019;139:e56–e528. - PubMed
-
- Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. New England Journal of Medicine. 2009;360:1418–1428. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous