Priority-setting dilemmas, moral distress and support experienced by nurses and physicians in the early phase of the COVID-19 pandemic in Norway
- PMID: 33430698
- PMCID: PMC7879232
- DOI: 10.1177/0969733020981748
Priority-setting dilemmas, moral distress and support experienced by nurses and physicians in the early phase of the COVID-19 pandemic in Norway
Abstract
Background: The global COVID-19 pandemic has imposed challenges on healthcare systems and professionals worldwide and introduced a ´maelstrom´ of ethical dilemmas. How ethically demanding situations are handled affects employees' moral stress and job satisfaction.
Aim: Describe priority-setting dilemmas, moral distress and support experienced by nurses and physicians across medical specialties in the early phase of the COVID-19 pandemic in Western Norway.
Research design: A cross-sectional hospital-based survey was conducted from 23 April to 11 May 2020.
Ethical considerations: Ethical approval granted by the Regional Research Ethics Committee in Western Norway (131421).
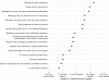
Findings: Among the 1606 respondents, 67% had experienced priority-setting dilemmas the previous two weeks. Healthcare workers who were directly involved in COVID-19 care, were redeployed or worked in psychiatry/addiction medicine experienced it more often. Although 59% of the respondents had seen adverse consequences due to resource scarcity, severe consequences were rare. Moral distress levels were generally low (2.9 on a 0-10 scale), but higher in selected groups (redeployed, managers and working in psychiatry/addiction medicine). Backing from existing collegial and managerial structures and routines, such as discussions with colleagues and receiving updates and information from managers that listened and acted upon feedback, were found more helpful than external support mechanisms. Priority-setting guidelines were also helpful.
Discussion: By including all medical specialties, nurses and physicians, and various institutions, the study provides information on how the COVID-19 mitigation also influenced those not directly involved in the COVID-19 treatment of patients. In the next stages of the pandemic response, support for healthcare professionals directly involved in outbreak-affected patients, those redeployed or those most impacted by mitigation strategies must be a priority.
Conclusion: Empirical research of healthcare workers experiences under a pandemic are important to identify groups at risks and useful support mechanisms.
Keywords: Clinical ethics; ethics and leadership/management; moral distress; moral/ethical climate of organisations; organisational ethics; professional ethics.
Conflict of interest statement
Figures


References
-
- Blumenthal-Barby J, Boyd K, Earp BD, et al. Pandemic medical ethics. J Med Ethics 2020; 46: 353–354. - PubMed
-
- Rosenbaum L. Facing Covid-19 in Italy – ethics, logistics, and therapeutics on the epidemic’s front line. New Engl J Med 2020; 382: 1873–1875. - PubMed
-
- Emanuel EJ, Persad G, Upshur R, et al. Fair allocation of scarce medical resources in the time of Covid-19. New Engl J Med 2020; 382: 2049–2055. - PubMed
-
- Truog RD, Mitchell C, Daley GQ. The toughest triage – allocating ventilators in a pandemic. N Engl J Med 2020; 382: 1973–1975. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

