Impact of baseline clinical and radiological features on outcome of chronic rhinosinusitis in granulomatosis with polyangiitis
- PMID: 33430923
- PMCID: PMC7802308
- DOI: 10.1186/s13075-020-02401-x
Impact of baseline clinical and radiological features on outcome of chronic rhinosinusitis in granulomatosis with polyangiitis
Abstract
Background: Granulomatosis with polyangiitis (GPA) causes a recurring inflammation in nose and paranasal sinuses that clinically resembles chronic rhinosinusitis (CRS) of other aetiologies. While sinonasal inflammation is not among the life-threatening features of GPA, patients report it to have major negative impact on quality of life. A relatively large proportion of GPA patients have severe CRS with extensive damage to nose and sinus structures evident by CT, but risk factors for severe CRS development remain largely unknown. In this study, we aimed to identify clinical and radiological predictors of CRS-related damage in GPA.
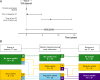
Methods: We included GPA patients who had clinical data sets from time of diagnosis, and two or more paranasal sinus CT scans obtained ≥12 months apart available for analysis. We defined time from first to last CT as the study observation period, and evaluated CRS development across this period using CT scores for inflammatory sinus bone thickening (osteitis), bone destructions, and sinus opacifications (here defined as mucosal disease). In logistic regression, we applied osteitis as main outcome measure for CRS-related damage.
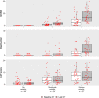
Results: We evaluated 697 CT scans obtained over median 5 years observation from 116 GPA patients. We found that 39% (45/116) of the GPA patients remained free from CRS damage across the study observation period, while 33% (38/116) had progressive damage. By end of observation, 32% (37/116) of the GPA patients had developed severe osteitis. We identified mucosal disease at baseline as a predictor for osteitis (odds ratio 1.33), and we found that renal involvement at baseline was less common in patients with severe osteitis at last CT (41%, 15/37) than in patients with no osteitis (60%, 27/45).
Conclusions: In this largely unselected GPA patient cohort, baseline sinus mucosal disease associated with CRS-related damage, as measured by osteitis at the end of follow-up. We found no significant association with clinical factors, but the data set indicated an inverse relationship between renal involvement and severe sinonasal affliction.
Keywords: Chronic rhinosinusitis; Granulomatosis with polyangiitis; Inflammation; Osteitis; Paranasal sinuses; Saddle nose deformity.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

Similar articles
-
Development of CT-based methods for longitudinal analyses of paranasal sinus osteitis in granulomatosis with polyangiitis.BMC Med Imaging. 2019 Feb 4;19(1):13. doi: 10.1186/s12880-019-0315-7. BMC Med Imaging. 2019. PMID: 30717680 Free PMC article.
-
Impact of Paranasal Sinus Surgery in Granulomatosis With Polyangiitis: A Longitudinal Computed Tomography Study.Laryngoscope. 2020 Aug;130(8):E460-E468. doi: 10.1002/lary.28639. Epub 2020 Apr 3. Laryngoscope. 2020. PMID: 32243590
-
Radiological markers of granulomatosis with polyangiitis with nasal involvement.Pol Arch Intern Med. 2021 Jul 30;131(7-8):649-657. doi: 10.20452/pamw.15998. Epub 2021 May 18. Pol Arch Intern Med. 2021. PMID: 34002970
-
Sinonasal imaging findings in granulomatosis with polyangiitis (Wegener granulomatosis): A systematic review.Am J Rhinol Allergy. 2017 Jan 1;31(1):16-21. doi: 10.2500/ajra.2017.31.4408. Am J Rhinol Allergy. 2017. PMID: 28234146
-
Immunological Mechanisms of Sensorineural Hearing Impairment in Patients with Different Clinical Phenotypes of Chronic Rhinosinusitis: A Narrative Review.Immunol Invest. 2025 Apr;54(3):396-411. doi: 10.1080/08820139.2024.2437638. Epub 2024 Dec 9. Immunol Invest. 2025. PMID: 39654361 Review.
Cited by
-
Rhinosinusitis: Evidence and experience - 2024.Braz J Otorhinolaryngol. 2025 May 19;91(5):101595. doi: 10.1016/j.bjorl.2025.101595. Online ahead of print. Braz J Otorhinolaryngol. 2025. PMID: 40398368 Free PMC article.
-
The Nasal Microbiome in ANCA-Associated Vasculitis: Picking the Nose for Clues on Disease Pathogenesis.Curr Rheumatol Rep. 2021 Jul 1;23(7):54. doi: 10.1007/s11926-021-01015-9. Curr Rheumatol Rep. 2021. PMID: 34196846 Free PMC article. Review.
References
-
- Jennette JC, Falk RJ, Andrassy K, Bacon PA, Churg J, Gross WL, et al. Nomenclature of systemic vasculitides. Arthritis Rheum. 1994;37(2):187–92. - PubMed
-
- Jennette JC, Falk RJ, Bacon PA, Basu N, Cid MC, Ferrario F, et al. 2012 Revised international chapel hill consensus conference nomenclature of vasculitides. Arthritis Rheum. 2013;65(1):1–11. - PubMed
-
- Leavitt RY, Fauci AS, Bloch DA, Michel BA, Hunder GG, Arend WP, et al. The American College of Rheumatology 1990 criteria for the classification of Wegener’s granulomatosis. Arthritis Rheum. 1990;33(8):1101–7. - PubMed
-
- Holle JU, Gross WL, Latza U, NÖlle B, Ambrosch P, Heller M, Fertmann R, Reinhold–Keller E. Improved outcome in 445 patients with Wegener’s granulomatosis in a German vasculitis center over four decades. Arthritis & Rheum. 2011;63(1):257–66. - PubMed
-
- Puéchal X, Pagnoux C, Perrodeau É. Hamidou M, Boffa JJ, Kyndt X, Lifermann F, Papo T, Merrien D, Smail A, Delaval P. Long-term outcomes among participants in the WEGENT trial of remission-maintenance therapy for granulomatosis with polyangiitis (Wegener’s) or microscopic polyangiitis. Arthritis Rheumatol. 2016;68(3):690–701. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

