Intramedullary injury combined with osteoporosis therapeutics regulates targeted local osteogenesis
- PMID: 33436871
- PMCID: PMC7804436
- DOI: 10.1038/s41598-020-80316-y
Intramedullary injury combined with osteoporosis therapeutics regulates targeted local osteogenesis
Abstract
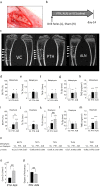
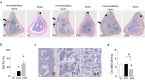
Bone marrow ablation prompts transient bone formation in nearly the entire medullary cavity before marrow regeneration occurs. Here, we establish a procedure to direct bone formation in a desired particular site within the medullary cavity for support of biomedical devices. Local intramedullary injury was performed in the tibiae of rats and parathyroid hormone (PTH), alendronate, or saline was administered. Newly generated bone in the medulla was assessed by micro-CT and histology. To evaluate the function of newly generated bone, animals received intramedullary injury in tibiae followed by daily PTH. At day-14, implants were placed in the endocortical bone and the bone response to the implants was assessed. The fate of newly generated bone was compared with and without implants. We found that neither intramedullary injury nor medication alone resulted in bone formation. However, when combined, substantial bone was generated locally inside the diaphyseal medulla. Newly formed bone disappeared without implant placement but was retained with implants. Bone was especially retained around and between the implants. This study found that local bone marrow disruption followed by PTH or alendronate generated substantial cancellous bone locally in the diaphyseal medulla. This approach offers promise as a tissue engineering tool in medicine and dentistry.
Conflict of interest statement
The authors declare no competing interests.
Figures
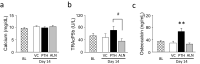

Similar articles
-
Effect of alendronate and intermittent parathyroid hormone on implant fixation in ovariectomized rats.J Orthop Sci. 2009 Mar;14(2):138-43. doi: 10.1007/s00776-008-1311-x. Epub 2009 Apr 1. J Orthop Sci. 2009. PMID: 19337803
-
Effects of PTH treatment on tibial bone of ovariectomized rats assessed by in vivo micro-CT.Osteoporos Int. 2009 Nov;20(11):1823-35. doi: 10.1007/s00198-009-0882-5. Epub 2009 Mar 5. Osteoporos Int. 2009. PMID: 19262974 Free PMC article.
-
Do antiosteoporotic drugs improve bone regeneration in vivo?Eur J Trauma Emerg Surg. 2020 Apr;46(2):287-299. doi: 10.1007/s00068-019-01144-y. Epub 2019 Apr 26. Eur J Trauma Emerg Surg. 2020. PMID: 31028428
-
Early effects of parathyroid hormone on bisphosphonate/steroid-associated compromised osseous wound healing.Osteoporos Int. 2014 Mar;25(3):1141-50. doi: 10.1007/s00198-013-2570-8. Epub 2013 Dec 4. Osteoporos Int. 2014. PMID: 24301537 Free PMC article.
-
[Parathyroid and bone. Evidence and perspective of parathyroid therapy for patients with osteoporosis].Clin Calcium. 2007 Dec;17(12):1888-94. Clin Calcium. 2007. PMID: 18057665 Review. Japanese.
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

