Prognostic Value of Abdominal Aortic Calcification: A Systematic Review and Meta-Analysis of Observational Studies
- PMID: 33439672
- PMCID: PMC7955302
- DOI: 10.1161/JAHA.120.017205
Prognostic Value of Abdominal Aortic Calcification: A Systematic Review and Meta-Analysis of Observational Studies
Abstract
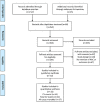
Background The prognostic importance of abdominal aortic calcification (AAC) viewed on noninvasive imaging modalities remains uncertain. Methods and Results We searched electronic databases (MEDLINE and Embase) until March 2018. Multiple reviewers identified prospective studies reporting AAC and incident cardiovascular events or all-cause mortality. Two independent reviewers assessed eligibility and risk of bias and extracted data. Summary risk ratios (RRs) were estimated using random-effects models comparing the higher AAC groups combined (any or more advanced AAC) to the lowest reported AAC group. We identified 52 studies (46 cohorts, 36 092 participants); only studies of patients with chronic kidney disease (57%) and the general older-elderly (median, 68 years; range, 60-80 years) populations (26%) had sufficient data to meta-analyze. People with any or more advanced AAC had higher risk of cardiovascular events (RR, 1.83; 95% CI, 1.40-2.39), fatal cardiovascular events (RR, 1.85; 95% CI, 1.44-2.39), and all-cause mortality (RR, 1.98; 95% CI, 1.55-2.53). Patients with chronic kidney disease with any or more advanced AAC had a higher risk of cardiovascular events (RR, 3.47; 95% CI, 2.21-5.45), fatal cardiovascular events (RR, 3.68; 95% CI, 2.32-5.84), and all-cause mortality (RR, 2.40; 95% CI, 1.95-2.97). Conclusions Higher-risk populations, such as the elderly and those with chronic kidney disease with AAC have substantially greater risk of future cardiovascular events and poorer prognosis. Providing information on AAC may help clinicians understand and manage patients' cardiovascular risk better.
Keywords: abdominal aortic calcification; all‐cause mortality; cardiovascular events and deaths; chronic kidney disease; general population.
Conflict of interest statement
None.
Figures



References
-
- Budoff MJ, Shaw LJ, Liu ST, Weinstein SR, Mosler TP, Tseng PH, Flores FR, Callister TQ, Raggi P, Berman DS. Long‐term prognosis associated with coronary calcification: observations from a registry of 25,253 patients. J Am Coll Cardiol. 2007;49:1860–1870. - PubMed
-
- Szulc P. Abdominal aortic calcification: a reappraisal of epidemiological and pathophysiological data. Bone. 2016;84:25–37. - PubMed
-
- Strong JP, Malcom GT, McMahan CA, Tracy RE, Newman WP III, Herderick EE, Cornhill JF. Prevalence and extent of atherosclerosis in adolescents and young adults: implications for prevention from the pathobiological determinants of atherosclerosis in youth study. JAMA. 1999;281:727–735. - PubMed
-
- Allam AHA, Thompson RC, Eskander MA, Mandour Ali MA, Sadek A, Rowan CJ, Sutherland ML, Sutherland JD, Frohlich B, Michalik DE, et al. Is coronary calcium scoring too late? Total body arterial calcium burden in patients without known CAD and normal MPI. J Nucl Cardiol. 2018;25:1990–1998. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

