Comparison of survival in elderly patients treated with uretero-cutaneostomy or ileal conduit after radical cystectomy
- PMID: 33441098
- PMCID: PMC7807694
- DOI: 10.1186/s12877-020-01861-9
Comparison of survival in elderly patients treated with uretero-cutaneostomy or ileal conduit after radical cystectomy
Abstract
Background: In bladder cancer patients with age ≥ 80 years old, there have been controversies in performing uretero-cutaneostomy or ileal conduit as urinary diversion after radical cystectomy. Limited study evaluated overall survival (OS) and cancer-specific survival (CSS) between the two urinary diversions in elderly patients. This study is to compare OS and CSS between uretero-cutaneostomy and ileal conduit after radical cystectomy in bladder cancer patients with age ≥ 80 years old.
Patients and methods: Data were extracted from the Surveillance, Epidemiology, and End Results (SEER) database. Bladder cancer patients diagnosed between 2004 and 2016 with age ≥ 80 years old who underwent radical cystectomy with either UC or IC were selected. After propensity score matching, Cox regression and Kaplan-Meier analysis were used to analyze the survival. We calculated statistical power for survival.
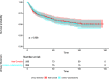
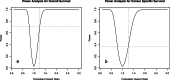
Results: Of 1394 patients who met the inclusion criteria, 1093 underwent ileal conduit and 301 underwent uretero-cutaneostomy. After propensity score matching, 285 patients were included in each group. Multivariable Cox analysis showed urinary diversion was not a risk factor of OS and CSS (HR 1.044, [95% CI 0.867-1.257] and 1.012 [0.748-1.368], respectively). Both OS and CSS were not significantly different, with median survival of ileal conduit and uretero-cutaneostomy were 19 [16-24] months and 19 [15-26] months respectively. Additionally, We found OS had the following risk factors: tumor stage (distant vs regional vs localized, 5.332 [3.610-7.875] vs 1.730 [1.375-2.176] vs 1), node density (>0.2 vs ≤0.2 vs none, 1.410 [1.047-1.898] vs 0.941 [0.658-1.344] vs 1) and age (1.067 [1.032-1.103] for each year). While CSS had the following risk factors: tumor stage (distant vs regional vs localized, 4.035 [2.046-7.959] vs 2.476 [1.651-3.713] vs 1), node density (>0.2 vs ≤0.2 vs none, 2.501 [1.645-3.804] vs 1.062 [0.590-1.914] vs 1) and tumor size (greater than 3 cm vs less than 3 cm, 1.596 [1.057-2.412] vs 1). Our analysis obtained 0.707 power for overall survival.
Conclusion: Urinary diversion by uretero-cutaneostomy or by ileal conduit was not associated with overall and cancer-specific survival. It is reasonable to consider uretero-cutaneostomy as a regular procedure of urinary diversion in elderly bladder cancer patients after radical cystectomy to avoid associate complications.
Keywords: 80 and over; Aged; SEER program; Urinary bladder neoplasms; Urinary diversion.
Conflict of interest statement
Shang Huang and Xuecheng Bi report grant from Health Commission of Guangdong Province, during the conduct of the study.
Figures

Comment in
-
Geriatrics.J Urol. 2021 Jun;205(6):1801-1804. doi: 10.1097/JU.0000000000001724. Epub 2021 Apr 1. J Urol. 2021. PMID: 33792370 No abstract available.
Similar articles
-
The impact of orthotopic neobladder vs ileal conduit urinary diversion after cystectomy on the survival outcomes in patients with bladder cancer: A propensity score matched analysis.Cancer Med. 2020 Oct;9(20):7590-7600. doi: 10.1002/cam4.3404. Epub 2020 Sep 1. Cancer Med. 2020. PMID: 32869540 Free PMC article.
-
Comparison of postoperative acute kidney injury between ileal conduit and neobladder urinary diversions after radical cystectomy: A propensity score matching analysis.Medicine (Baltimore). 2016 Sep;95(36):e4838. doi: 10.1097/MD.0000000000004838. Medicine (Baltimore). 2016. PMID: 27603401 Free PMC article.
-
Incidence and risk factors of 30-day early and 90-day late morbidity and mortality of radical cystectomy during a 13-year follow-up: a comparative propensity-score matched analysis of complications between neobladder and ileal conduit.Jpn J Clin Oncol. 2014 Jul;44(7):677-85. doi: 10.1093/jjco/hyu051. Epub 2014 May 3. Jpn J Clin Oncol. 2014. PMID: 24791782
-
[A case of late recurrence of urothelial carcinoma in an ileal conduit after radical cystectomy and ileal conduit diversion for bladder cancer].Hinyokika Kiyo. 2012 Feb;58(2):109-12. Hinyokika Kiyo. 2012. PMID: 22450840 Review. Japanese.
-
[Indications and current results of substitution enteroplasty following radical cystectomy].Bull Acad Natl Med. 2005 Jan;189(1):123-32; discussion 132-4. Bull Acad Natl Med. 2005. PMID: 16119885 Review. French.
Cited by
-
Robotic-assisted radical cystectomy with cutaneous ureterostomies: a contemporary multicenter analysis.World J Urol. 2024 Apr 23;42(1):251. doi: 10.1007/s00345-024-04942-1. World J Urol. 2024. PMID: 38652316
-
Comparison of long-term outcomes between ileal conduit and transuretero-cutaneostomy urinary diversion after radical cystectomy: a systematic review and meta-analysis.Rep Pract Oncol Radiother. 2024 Mar 18;29(1):103-112. doi: 10.5603/rpor.99098. eCollection 2024. Rep Pract Oncol Radiother. 2024. PMID: 39165596 Free PMC article.
-
Robot-assisted radical cystectomy with the clinical application of "Y-shaped" end-to-side ureteral anastomosis in elderly and obese patients.BMC Urol. 2025 Mar 20;25(1):56. doi: 10.1186/s12894-024-01684-5. BMC Urol. 2025. PMID: 40114107 Free PMC article.
-
Twenty-Four-Month Efficacy of Ureteroureterostomy Combined With Unilateral Nephrostomy Following Radical Cystectomy.Cureus. 2022 Oct 19;14(10):e30478. doi: 10.7759/cureus.30478. eCollection 2022 Oct. Cureus. 2022. PMID: 36415445 Free PMC article.
-
The Association between Urinary Diversion Type and Other-Cause Mortality in Radical Cystectomy Patients.Cancers (Basel). 2024 Jan 19;16(2):429. doi: 10.3390/cancers16020429. Cancers (Basel). 2024. PMID: 38275870 Free PMC article.
References
-
- Weiner AB, Keeter MK, Manjunath A, Meeks JJ. Discrepancies in staging, treatment, and delays to treatment may explain disparities in bladder cancer outcomes: An update from the National Cancer Data Base (2004–2013) Urol Oncol. 2018;36(237):e239–e237. - PubMed
-
- Nieuwenhuijzen JA, de Vries RR, Bex A, van der Poel HG, Meinhardt W, Antonini N, Horenblas S. Urinary diversions after cystectomy: the association of clinical factors, complications and functional results of four different diversions. Eur Urol. 2008;53:834–842. doi: 10.1016/j.eururo.2007.09.008. - DOI - PubMed
-
- Vakalopoulos I, Dimitriadis G, Anastasiadis A, Gkotsos G, Radopoulos D. Does intubated uretero-ureterocutaneostomy provide better health-related quality of life than orthotopic neobladder in patients after radical cystectomy for invasive bladder cancer? Int Urol Nephrol. 2011;43:743–748. doi: 10.1007/s11255-011-9904-2. - DOI - PubMed
-
- Nahar B, Koru-Sengul T, Miao F, Prakash NS, Venkatramani V, Gauri A, Alonzo D, Alameddine M, Swain S, Punnen S, et al. Comparison of readmission and short-term mortality rates between different types of urinary diversion in patients undergoing radical cystectomy. World J Urol. 2018;36:393–399. doi: 10.1007/s00345-017-2140-3. - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

