Effects of aging on brain networks during swallowing: general linear model and independent component analyses
- PMID: 33441738
- PMCID: PMC7806781
- DOI: 10.1038/s41598-020-79782-1
Effects of aging on brain networks during swallowing: general linear model and independent component analyses
Abstract
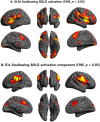
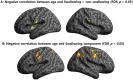
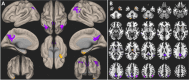
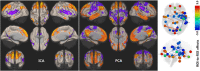
Swallowing disorders occur more frequently in older adults. However, the effects of the aging process on neural activation when swallowing are unclear. We aimed to identify neural regions activated during swallowing and evaluate changes in neural activation and neural networks with aging. Using a general linear model (GLM) and independent component (IC) analyses, blood oxygen level-dependent (BOLD) signals were observed in the lateral precentral gyrus, postcentral gyrus, anterior insular cortices, supramarginal gyri, and medial frontal gyrus during swallowing. The right thalamus and anterior cingulate gyri were found to be active areas by GLM and IC analyses, respectively. In the correlational analyses, age was negatively correlated with BOLD signals of the lateral precentral gyri, postcentral gyri, and insular cortices in swallowing tasks. Additionally, correlation analyses between ICs of all participants and age revealed negative correlations in the right supramarginal gyrus, both anterior cingulate cortices, putamen, and cerebellum. In the network analysis, the BOLD signal positively correlated with age in the default mode network (DMN), and was negatively correlated in the lateral precentral gyri, postcentral gyri, and insular cortices. The amplitude of low-frequency fluctuations was significantly decreased in the DMN and increased in swallowing-related areas during swallowing tasks. These results suggest that aging has negative effects on the activation of swallowing-related regions and task-induced deactivation of the DMN. These changes may be used to detect early functional decline during swallowing.
Conflict of interest statement
The authors declare no competing interests.
Figures

Similar articles
-
Correlation Between Swallowing and Cognitive Brain Networks in Older Adults via Functional MRI.J Oral Rehabil. 2024 Dec;51(12):2588-2599. doi: 10.1111/joor.13855. Epub 2024 Sep 20. J Oral Rehabil. 2024. PMID: 39305044
-
Cerebral areas processing swallowing and tongue movement are overlapping but distinct: a functional magnetic resonance imaging study.J Neurophysiol. 2004 Oct;92(4):2428-43. doi: 10.1152/jn.01144.2003. Epub 2004 May 26. J Neurophysiol. 2004. PMID: 15163677 Clinical Trial.
-
Effects of Motor Imagery and Visual Neurofeedback on Activation in the Swallowing Network: A Real-Time fMRI Study.Dysphagia. 2019 Dec;34(6):879-895. doi: 10.1007/s00455-019-09985-w. Epub 2019 Feb 15. Dysphagia. 2019. PMID: 30771088 Free PMC article.
-
Neural activation of swallowing and swallowing-related tasks in healthy young adults: an attempt to separate the components of deglutition.Hum Brain Mapp. 2009 Oct;30(10):3209-26. doi: 10.1002/hbm.20743. Hum Brain Mapp. 2009. PMID: 19247994 Free PMC article.
-
Spontaneous low-frequency fluctuations in the BOLD signal in schizophrenic patients: anomalies in the default network.Schizophr Bull. 2007 Jul;33(4):1004-12. doi: 10.1093/schbul/sbm052. Epub 2007 Jun 7. Schizophr Bull. 2007. PMID: 17556752 Free PMC article. Review.
Cited by
-
Clinical utility of fMRI in evaluating of LSD effect on pain-related brain networks in healthy subjects.Heliyon. 2024 Jul 17;10(15):e34401. doi: 10.1016/j.heliyon.2024.e34401. eCollection 2024 Aug 15. Heliyon. 2024. PMID: 39165942 Free PMC article.
-
Clinical determinants and neural correlates of presbyphagia in community-dwelling older adults.Front Aging Neurosci. 2022 Jul 28;14:912691. doi: 10.3389/fnagi.2022.912691. eCollection 2022. Front Aging Neurosci. 2022. PMID: 35966778 Free PMC article.
-
The Cortical and Subcortical Neural Control of Swallowing: A Narrative Review.Dysphagia. 2024 Apr;39(2):177-197. doi: 10.1007/s00455-023-10613-x. Epub 2023 Aug 21. Dysphagia. 2024. PMID: 37603047 Review.
-
A network approach to the investigation of childhood irritability: probing frustration using social stimuli.J Child Psychol Psychiatry. 2024 Jul;65(7):959-972. doi: 10.1111/jcpp.13937. Epub 2023 Dec 20. J Child Psychol Psychiatry. 2024. PMID: 38124618 Free PMC article.
-
Exploring the Associations Between Dysphagia and Health-Related Outcomes in Older Adults: Results from the ilSirente Study.Nutrients. 2025 Jun 28;17(13):2149. doi: 10.3390/nu17132149. Nutrients. 2025. PMID: 40647257 Free PMC article.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

