Online adaptive dose restoration in intensity modulated proton therapy of lung cancer to account for inter-fractional density changes
- PMID: 33458323
- PMCID: PMC7807540
- DOI: 10.1016/j.phro.2020.06.004
Online adaptive dose restoration in intensity modulated proton therapy of lung cancer to account for inter-fractional density changes
Abstract
Background and purpose: In proton therapy, inter-fractional density changes can severely compromise the effective delivery of the planned dose. Such dose distortion effects can be accounted for by treatment plan adaptation, that requires considerable automation for widespread implementation in clinics. In this study, the clinical benefit of an automatic online adaptive strategy called dose restoration (DR) was investigated. Our objective was to assess to what extent DR could replace the need for a comprehensive offline adaptive strategy.
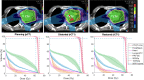
Materials and methods: The fully automatic and robust DR workflow was evaluated in a cohort of 14 lung IMPT patients that had a planning-CT and two repeated 4D-CTs (rCT1,rCT2). Initial plans were generated using 4D-robust optimization (including breathing-motion, setup and range errors). DR relied on isodose contours generated from the initial dose and associated patient specific weighted objectives to mimic this initial dose in repeated-CTs. These isodose contours, with their corresponding objectives, were used during re-optimization to compensate proton range distortions disregarding re-contouring. Robustness evaluations were performed for the initial, not-adapted and restored (adapted) plans.
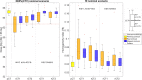
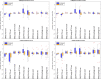
Results: The resulting DVH-bands showed overall improvement in DVH metrics and robustness levels for restored plans, with respect to not-adapted plans. According to CTV coverage criteria (D95%>95%Dprescription) in not-adapted plans, 35% (5/14) of the cases needed offline adaptation. After DR, Median(D95%) was increased by 1.1 [IQR,0.4] Gy and only one patient out of 14 (7%) still needed offline adaptation because of important anatomical changes.
Conclusions: DR has the potential to improve CTV coverage and reduce offline adaptation rate.
Keywords: Adaptive proton therapy; Adaptive radiation therapy; Automated adaptation; Proton therapy; Range uncertainties.
© 2020 The Authors.
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures


Similar articles
-
Evaluation of the clinical value of automatic online dose restoration for adaptive proton therapy of head and neck cancer.Radiother Oncol. 2022 May;170:190-197. doi: 10.1016/j.radonc.2022.03.011. Epub 2022 Mar 25. Radiother Oncol. 2022. PMID: 35346754
-
Deformed dose restoration to account for tumor deformation and position changes for adaptive proton therapy.Med Phys. 2023 Feb;50(2):675-687. doi: 10.1002/mp.16149. Epub 2022 Dec 29. Med Phys. 2023. PMID: 36502527
-
Feasibility of online IMPT adaptation using fast, automatic and robust dose restoration.Phys Med Biol. 2018 Apr 20;63(8):085018. doi: 10.1088/1361-6560/aaba8c. Phys Med Biol. 2018. PMID: 29595145
-
Intensity-modulated proton therapy (IMPT) interplay effect evaluation of asymmetric breathing with simultaneous uncertainty considerations in patients with non-small cell lung cancer.Med Phys. 2020 Nov;47(11):5428-5440. doi: 10.1002/mp.14491. Epub 2020 Oct 13. Med Phys. 2020. PMID: 32964474 Free PMC article.
-
Technical Note: Treatment planning system (TPS) approximations matter - comparing intensity-modulated proton therapy (IMPT) plan quality and robustness between a commercial and an in-house developed TPS for nonsmall cell lung cancer (NSCLC).Med Phys. 2019 Nov;46(11):4755-4762. doi: 10.1002/mp.13809. Epub 2019 Sep 21. Med Phys. 2019. PMID: 31498885
Cited by
-
Comparison of 3D and 4D robustly optimized proton treatment plans for non-small cell lung cancer patients with tumour motion amplitudes larger than 5 mm.Phys Imaging Radiat Oncol. 2023 Jun 24;27:100465. doi: 10.1016/j.phro.2023.100465. eCollection 2023 Jul. Phys Imaging Radiat Oncol. 2023. PMID: 37449022 Free PMC article.
-
Image guidance and interfractional anatomical variation in paediatric abdominal radiotherapy.Br J Radiol. 2023 Jun 1;96(1146):20230058. doi: 10.1259/bjr.20230058. Epub 2023 May 10. Br J Radiol. 2023. PMID: 37102707 Free PMC article.
-
Online adaptive planning methods for intensity-modulated radiotherapy.Phys Med Biol. 2023 May 11;68(10):10.1088/1361-6560/accdb2. doi: 10.1088/1361-6560/accdb2. Phys Med Biol. 2023. PMID: 37068488 Free PMC article. Review.
-
Surveying the clinical practice of treatment adaptation and motion management in particle therapy.Phys Imaging Radiat Oncol. 2023 Jun 9;27:100457. doi: 10.1016/j.phro.2023.100457. eCollection 2023 Jul. Phys Imaging Radiat Oncol. 2023. PMID: 37361612 Free PMC article. No abstract available.
-
Potential of automated online adaptive proton therapy to reduce margins for oesophageal cancer.Phys Imaging Radiat Oncol. 2025 Jan 31;33:100712. doi: 10.1016/j.phro.2025.100712. eCollection 2025 Jan. Phys Imaging Radiat Oncol. 2025. PMID: 40123774 Free PMC article.
References
-
- Kesarwala A.H., Ko C.J., Ning H., Xanthopoulos E., Haglund K.E., O’Meara W.P. Intensity-modulated proton therapy for elective nodal irradiation and involvedfield radiation in the definitive treatment of locally advanced non–small-cell lung cancer: a dosimetric study. Clin Lung Cancer. 2015;16:237–244. doi: 10.1016/j.cllc.2014.12.001. - DOI - PMC - PubMed
-
- Ferris M.J., Martin K.S., Switchenko J.M., Kayode O.A., Wolf J., Dang Q. Sparing Cardiac Substructures With Optimized Volumetric Modulated Arc Therapy and Intensity Modulated Proton Therapy in Thoracic Radiation for Locally Advanced Non-small Cell Lung Cancer. Pract Radiat Oncol. 2019;9:e473–e481. doi: 10.1016/j.prro.2019.04.013. - DOI - PMC - PubMed
-
- Nichols R.C., Huh S.N., Henderson R.H., Mendenhall N.P., Flampouri S., Li Z. Proton radiation therapy offers reduced normal lung and bone marrow exposure for patients receiving dose-escalated radiation therapy for unresectable stage iii non-smallcell lung cancer: a dosimetric study. Clin Lung Cancer. 2019;12:252–257. doi: 10.1016/j.cllc.2011.03.027. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

